Interview
Share on social media
This article was originally published on TechTalks.com.
Meeting the challenges of AI in health care
Artificial intelligence promises to help us become faster and better and fighting diseases, live healthier lives, and reduce the costs of health care. And in the past decade, there has been plenty of research that shows deep learning, the branch of AI that turns data patterns into predictions, can be a very useful tool at many challenging tasks such as diagnosing different types of cancer, speeding up drug discovery, and providing precision care.
Applying AI to real-world health care problems, however, is a complicated process that involves solving a multitude of problems that go beyond creating AI models that can map inputs to outputs.
In an interview with TechTalks, Tina Manoharan, Global Lead Data Science and AI Center of Excellence and Digital Research Division at Philips, spoke about the opportunities, challenges, and prospects of applying AI in real-world health care applications. Manoharan has experience in both academic AI research and developing products that leverage AI algorithms. She has done her master’s thesis and Ph.D. in supervised machine learning and AR/VR simulations and worked as a research associate during her Ph.D. Today, she is leading efforts to leverage data science and AI to support Philips Clusters, Businesses, and Markets with the creation of smart connected devices, services, and solutions.
The need for AI in health care
The health care sector is in need of a revolution, Manoharan believes. “Healthcare systems and providers are under huge pressure, now more than ever with the COVID-19 pandemic,” she says, to which she adds, “We are dealing with global staff shortages, aging populations, and lifestyle-related chronic diseases.”
At the same time, digital transformation is driving exponential growth of health data. With digitization and connectivity becoming ubiquitous, we’re more capable than ever to collect information about individual and population health. But putting that data to use is a huge challenge.
“I remember clinicians telling me, ‘Just because we have a lot of data, don’t overload me with that, I need relevant and precise information, at the point of decision making,’” says Manoharan.
Artificial intelligence provides unprecedented opportunities to put all this data to good use and help physicians, clinicians, health care workers, and patients to make more informed decisions.
“AI enables our devices, systems, software, and services to be context-aware, precise, personalized, predictive, and pro-active,” Manoharan says. “By turning data into actionable insights for precision health, we will enable precise and personalized care across the health continuum.”
But in addition to improving the precision of health care, AI can make the entire experience of medical care more human. With the help of AI, doctors will spend less time poring over data and medical records and will have more time to spend with patients.
“AI can help free clinicians from more mundane tasks, so that they are able to focus on what they do best and engage with patients in a more precise and personalized way, with the potential to increase value over time,” Manoharan says.
While a lot of the discussion surrounding AI is about software replacing humans, in health care, AI must be considered as an augmenting factor.
“A lot of the decisions that clinicians make on a daily basis are incredibly complex and require more than an AI- or data-driven approach alone. It’s the augmented intelligence and support for decision making at the right time that helps to make a difference to effective patient management,” Manoharan says, adding that taking a human-centered approach to AI development is important. “I strongly believe that clinicians and AI have unique strengths that complement and augment each other, not replace each other.”
Applications of AI in health care
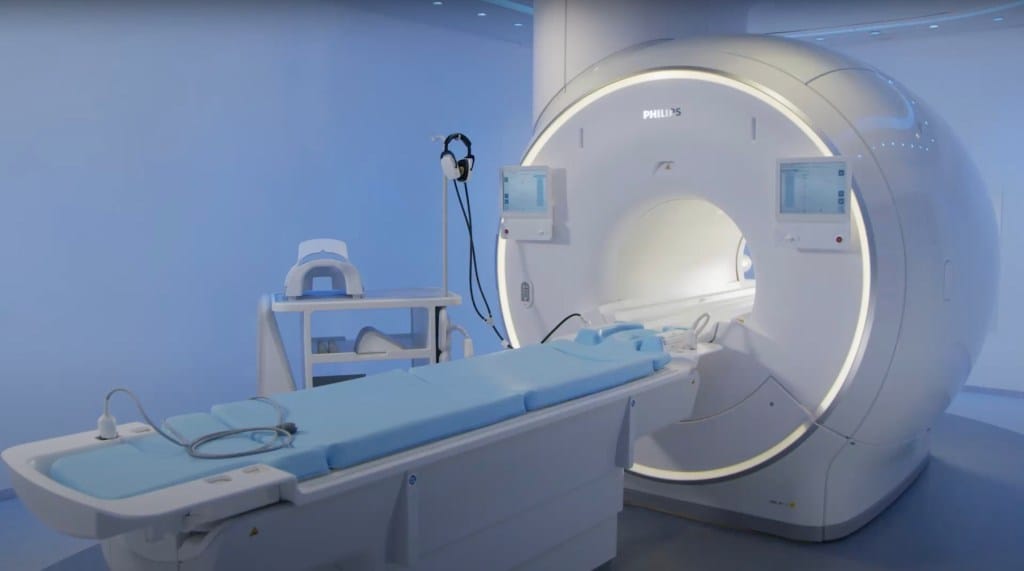
At Philips, Manoharan has been involved in several initiatives to leverage artificial intelligence to improve clinical operations. One example is the use of AI to speed up the medical resonance imaging (MRI) process.
“The challenge here is that MR offers many advantages (e.g., no radiation), but is relatively time-consuming: a complete exam can take up to one hour,” Manoharan says. “Risk of patient motion can lead to poor image quality and result in having to redo the exam.”
Patients are often in pain when going for the MRI scan. The duration of the scan and the confined space cause further stress in the experience. Aside from the uncomfortable experience to patients, the challenges such as repeat scans increase the costs and further tighten the schedule of MRI staff in hospitals.
In 2019, Facebook AI Research and New York University Langone Health launched the fastMRI challenge, a competition that aims to improve the speed of MRI scans by using artificial intelligence. The participants used different deep learning architectures to improve image acquisition capabilities and reduce the time patients need to spend in the MRI scanner.
A deep learning model developed by a team at Philips and the University Medical Center of Leiden (LUMC) was among the top performers in the contest. The deep learning model succeeded in providing an eight-fold speed increase in reconstructing high-quality MRI images. The next step is to incorporate the findings from this and other research projects into products that can be used in real health care settings.
“We are now working on a suite of AI applications that can help speed up the workflow for the entire MR exam—from patient scheduling to creating the report,” Manoharan says.
An example is a system that speeds up the MR exam setup stage by using computer vision to detect breathing while patients are in the scanner. The standard method requires a belt that needs to be adjusted for each patient, a process that can take several minutes. The AI-powered solution, called VitalEye, performs touchless breathing detection and cuts down the preparation time to under one minute.
Philips is also working on the use of AI in intensive care units, where time is of the essence, and making the right decision in a timely manner can have a profound impact on patients’ health.
“Here, the challenge lies in spotting early signs of patient deterioration, when you have to oversee many patients in a highly dynamic and stressful environment,” Manoharan says.
Philips is working on a solution that uses predictive analytics to identify patients who may require an intervention in the next 60 minutes. The solution uses machine learning models trained on historical data from in- and out-patient encounters, medical records, and medical alert systems to calculate risk scores for patients. The output of the AI is provided to health care professionals, who make the final decision.
This could enable healthcare professionals to intervene faster and improve patient outcomes.
The team is also considering integrating the AI models with other tools and technologies to enable intensivists to monitor patients remotely from a central monitoring location using telemedicine and support their colleagues at the bedside.
“In the wake of COVID-19, I expect that we will also see more use of remote monitoring tools, such as wearable biosensors, to follow a patient’s health at home. This could be helpful in the case of patients with chronic conditions,” Manoharan says. “We can then use predictive analytics to predict which patients may need additional care and reach out to them proactively.”
Integrating AI into existing workflows

While every year, we’re seeing a lot of effort go into research of artificial intelligence in health care, the integration of the developed techniques into real applications presents some challenges.
“AI definitely represents a huge opportunity to improve healthcare as it can be very powerful. But to have that impact, it needs to be integrated deeply into the workflow of clinical staff and/or the daily routines of patients,” Manoharan says.
The engineers and developers of AI systems must also make sure their systems fit smoothly into the workflow of health care professionals, who are usually short on time. If an AI system is designed as a separate application that adds extra steps to a clinical procedure, it will be less likely to find traction among practitioners.
“We need to keep in mind that an AI algorithm in itself is not a solution, it’s a tool that needs to be integrated into the workflow,” Manoharan says. “This means you need to understand the workflow first and design a solution with human-AI collaboration in mind. AI must provide you with the right information at the right time in the right form. For example, as a radiologist, if you have an AI solution that helps you interpret an image, you shouldn’t have to switch workstations to open another application to run the algorithm.”
AI requires consolidated health data
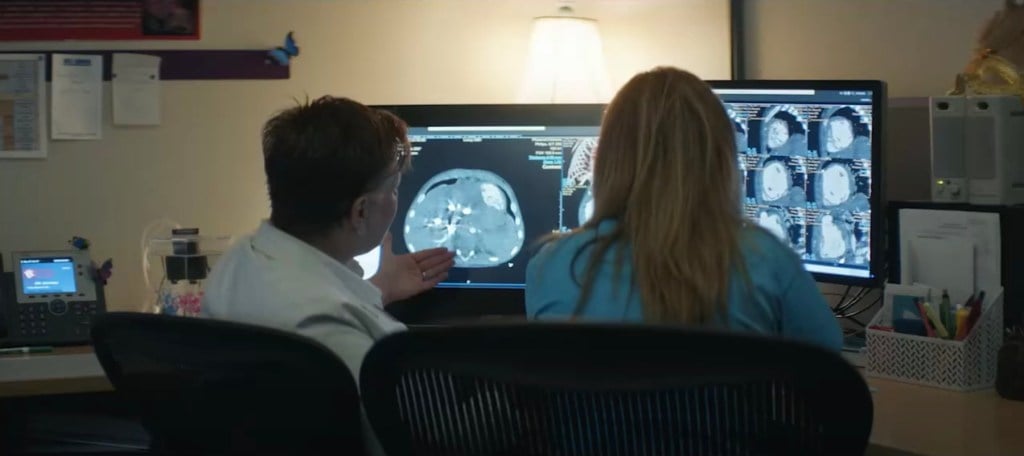
AI systems must also be supported by tools that can integrate them into different IT and data systems. “To get meaningful insights from data with AI, interoperability is really key,” Manoharan says. The interoperability and integration challenge is one of the key factors that separates academic research from practical applications of AI. Research usually revolves around developing AI models that work on carefully curated sets of health data. In real life, however, data is messy, fragmented, and hard to access. In many cases, the lack of a proper data infrastructure is the main barrier in the way of applying AI to existing applications. “Today’s healthcare data is often difficult to exchange, analyze, and interpret. Many point solutions with AI already exist today but the healthcare supplier environment is highly fragmented. Healthcare providers are in need of integrated offerings combining the best available HealthTech innovations from different suppliers into one seamless and complete patient-centric and disease-focused solution,” Manoharan says. Solving this problem will need a concerted effort between tech vendors, hospitals, and health care organizations. “We need to connect data from equipment from multiple vendors, linking to hospital IT systems, and we need data standards that allow you to make sense of data in a uniform way, using one data language; what we call semantic interoperability,” Manoharan, adding, “Connected data lakes are essential here.” Data lakes are large repositories that do not impose schematic restrictions on the data stored in them. Data can be stored in raw formats such as text files, images, and videos, as well as well-structured spreadsheets. The data can then be mined and queried with data science and machine learning tools.
Meeting the integration and legal challenges

To build a holistic view of patients with AI, data needs to follow the patient, Manoharan says. “We need to connect the dots across various medical conditions the patient may have, and along the continuum of care. Linking hospitals to the home, primary care, etc.,” she says. “For this, you also need continuous patient engagement and feedback to understand their experience with the prescribed treatment, and to factor in the patient-reported outcomes into clinical decision-making.”
This, of course, will present some legal challenges. Medical data is sensitive and subject to privacy regulations that vary across jurisdictions. Companies that develop AI solutions for health care and medicine can run afoul of privacy laws if they’re not careful, and the industry is still feeling its way toward finding the balance between access to data and protecting sensitive health data.
“Regional legislation has to enable secure exchange and access to properly annotated data for medical research and clinical practice while safeguarding patient privacy,” Manoharan says.
The effort also requires new approaches from vendors of health technology, which will streamline the development of AI solutions.
“Medical equipment vendors have to start enabling the creation of applications by third parties, like innovative start-ups, or academic clinical centers, through publishing application programming interfaces (API),” Manoharan says.
Manoharan stresses that before an AI-powered product reaches adoption and has an impact on health care, it will face other technical and non-technical barriers such as monetization, implementation effort, actual workflow improvement, and trust. “We need to think of things like, where does the money come from, how our customers will pay for the AI, what are the reimbursement and efficiency gains,” Manoharan says.
The future of AI in health care
Manoharan believes that while many point solutions with AI already exist, the next true leap forward is to integrate offerings into seamless and complete patient-centric solutions that can collaborate to reach precise diagnoses and more optimal treatment pathways.
“We should also pay attention to existing and new challenges and barriers while developing new AI-based technologies,” Manoharan adds.
With the digital transformation driving exponential growth of health data and the industry changing rapidly, we must acknowledge that that we don’t have all the answers yet, Manoharan believes.
“New questions will arise as we continue on this exciting path of discovery and innovation with AI, and we should be open and transparent in addressing them together while keeping our patient and customer needs in the center of everything we do,” she says. “This way, we can confront and conquer some of society’s most pressing challenges. And we can more directly respond to the ever-changing needs of our most important customers across the globe, the people.”
The latest from Philips Research

Global Lead Data Science and AI Center of Excellence and Digital Research Division at Philips
