Like many of you, I am working from home during the COVID-19 pandemic and have limited my movement to an absolute minimum. Yet despite being in a high-risk self-isolating category, I am not isolated. I continue to be in ‘virtual’ touch with colleagues, customers, friends and family. We are hearing the first stories of acquaintances who have contracted the virus or have already lost loved ones. If you are one of them, I wish you strength in these unsettling times. With enormous stress on healthcare systems around the globe, it is more urgent than ever before to step up collaboration, information and knowledge sharing, and agility in the delivery of diagnostic, respiratory and monitoring solutions at scale.
How Philips is helping in the fight against COVID-19
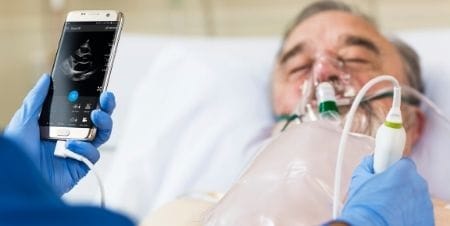
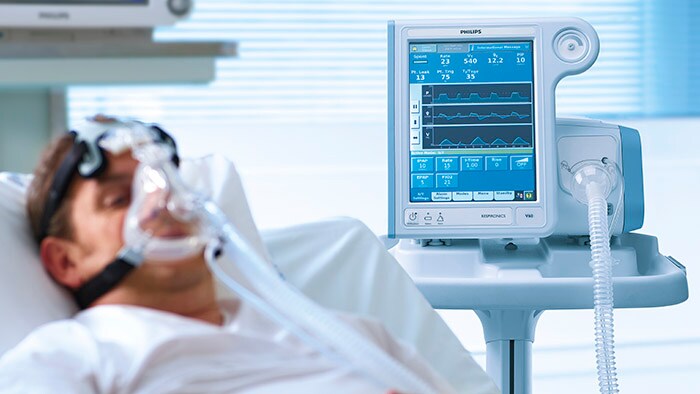
Our CEO Frans van Houten released a statement recently on how our company is responding to the constantly evolving COVID-19 situation. From my home, together with my colleagues around the globe, we are working around the clock to deliver ventilators, monitors, diagnostic equipment and virtual care solutions to support our amazing care providers in their endless efforts to help patients. We have ramped up the production of ventilators, monitors and solutions to help diagnose and treat patients. At the same time, we are helping hospitals to increase their number of ICU beds to accommodate the most critical and acute coronavirus patients. People around the globe are doing everything they can to contain COVID-19 or at least slow down the rate of infection. We should all adhere to the guidelines on social distancing and hygiene and stay up-to-date with the latest information from trusted healthcare sources, so we can act as responsible citizens in a fast-changing situation. The guiding principle for information is that it should be transparent and evidence-based. And one of our most powerful instruments for evidence-based healthcare is the technology to collect, qualify and analyze data in ways that quickly reveal patterns and hidden insights. It highlights the need for robust health-data infrastructures. In the Netherlands, we have contributed to the launch of a COVID-19 data exchange portal that connects providers to support patient transfers. It enables that a patient’s data is easily though securely transferred via the cloud from hospital A to B. Another valuable instrument for coping with a rapidly spreading infection like COVID-19 is ‘virtual care’, sometimes referred to as telehealth. With the large number of patients involved and the face-to-face risk of infecting other patients and staff, online consultations can provide valuable relief to the healthcare system. Philips has made available a dedicated scalable telehealth solution that facilitates the use of online patient screening and monitoring, supported by external call centers. The solution aims to prevent unnecessary visits to general practitioners and hospitals by remotely monitoring the vast majority of COVID-19 patients that are quarantined at home. Patients infected with COVID-19 can be remotely monitored via smart questionnaires about their home situation and state of health, identifying if intervention is needed.
With enormous stress on healthcare systems around the globe, it is more urgent than ever before to step up collaboration, information and knowledge sharing, and agility in the delivery of diagnostic, respiratory and monitoring solutions at scale.
Jeroen Tas
Chief Innovation & Strategy Officer, Philips

In the current situation, where COVID-19 occasionally results in severe pneumonia, there will be an increasing number of patients requiring acute care in hospital or in an intensive care unit (ICU). The numbers swelling to unmanageable proportions is already happening in many countries and remains a real worry for healthcare authorities around the world, not simply because of the limited number of ICU beds and ventilators but also because of staff shortages and burn-out. Trained ICU doctors and nurses are already in short supply and repeated exposure to infected patients will increase their own risk of contracting the virus.
How COVID-19 is spurring the move to virtual care
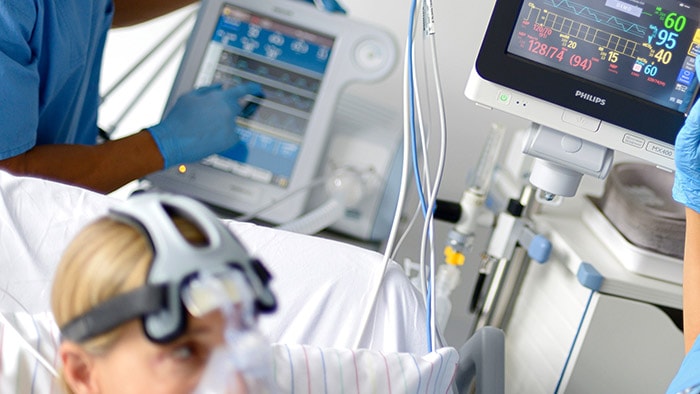
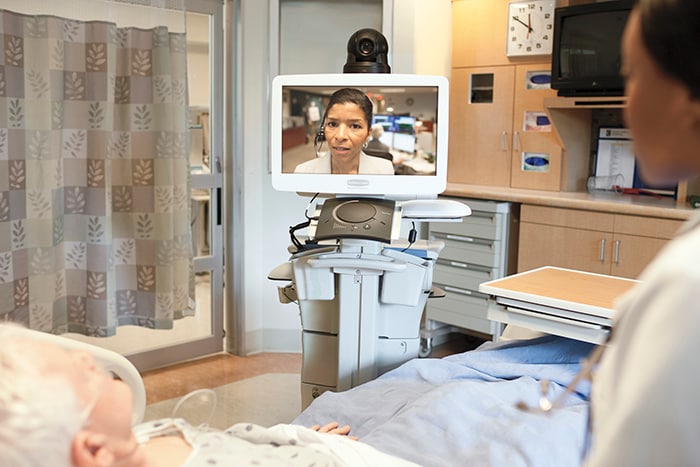
A tele-ICU or eICU enables a co-located team of intensivists and critical care nurses to remotely monitor patients in the ICU regardless of patient location. Intensivists and nurses based in a telehealth eICU hub are supported by high-definition cameras, telemetry, predictive analytics, data visualization and advanced reporting capabilities in order to support their frontline colleagues. Algorithms alert to signs of patient deterioration or improvement. They help care teams to proactively intervene at an earlier stage or to decide which patients have stabilized and can be transferred, allowing scarce ICU beds to be allocated to more acute patients. The tele-ICU can be embedded in a larger Clinical and Operations Center that prioritizes patients on acuity and optimizes the patient flow and logistics. Solutions like these enable more COVID-19 patients to receive care. As we speak, we are helping hospitals with installed eICUs to expand their reach and exchange important information about COVID-19 indicators and protocols. We are supporting others to expand the reach of their ICUs into other settings. Northwell Health recently gave a webinar, during which its clinicians shared their experiences of using their eICU for patients with COVID-19. Advanced telemetry and camera technologies hold out the promise of monitoring acute patients at scale. In the near future, you can expect image analysis software that measures an ICU patient’s temperature, heart rate and respiration rate from a distance of several meters. Using existing patient monitoring solutions, AI is already able to use the acquired data to predict when a patient’s condition is about to deteriorate, hours before a nurse would be able to spot it. And when patients do deteriorate, secure connections to external clinical experts allow appropriate treatment plans to be initiated. When there are staff shortages, such as reduced availability of night-shift staff, monitoring can be done from remote locations, even halfway across the world where people are wide awake. We are already deploying vital signs camera technology to detect deterioration in patients waiting in emergency department waiting rooms so they can receive quick attention. The remote monitoring approach can also be extended to the home, with smart wearables tracking patients who are infected or at risk of infection. These wearables, like a smart patch, can measure body temperature, respiration rate and heart rate, monitor sleep and detect falls. All these measurements can be combined with contextual and behavioral information about the patient to keep them as safe as possible. We are working on rapidly deployable solutions like these for (at risk) patients.
Tele-ICUs and home monitoring are only part of the solution. Bottlenecks don’t only appear in bed and staff availability. They also appear in critical areas such as diagnosis. Ultrasound, X-ray and CT scans are useful tools for COVID-19 diagnosis and follow-up [2], but if patient numbers grow rapidly the radiologists who assess them will be confronted by a much increased workload. If there are not enough radiologists available in a hospital to take care of the local population, tele-radiology services can potentially offer them much needed support. Radiologists from one hospital can remotely support their colleagues in another hospital. Even so, with so many new COVID-19 cases appearing in countries around the world, patients often have to wait hours before getting the results. AI-enabled CT image analysis could potentially help to screen suspected COVID-19 patients within minutes. This in turn could relieve pressure on complex laboratory-based tests to confirm the presence of coronavirus. There are some tough challenges to be solved though before an algorithm can distinguish influenza from COVID-19. A whole raft of innovative new ideas and coping strategies are currently being tested in different countries around the world. In the near future, we could see digital services closing the loop between consultations and the dispatch of care or prescription drugs, drones as vehicles for getting drugs to patients, robots disinfecting contaminated areas. Apps and chat-bots that act as symptom checkers and provide up-to-the-minute travel and infection control advice. Medical wearables that monitor patients at home. 5G-enabled cameras that check for symptoms in seconds. New ways of working that keep diagnostic procedures safe while still allowing fast assessment, such as the robot-guided ultrasound being trialed in China. Anything to keep the risk of disease transmission down to a minimum. Although these innovations won’t play global roles in the acute situation we are in right now, keep an eye on these developments. It may well be that many health systems go back to the drawing board to improve their care based on today’s experiences. I think the most important thing right now is that we work together, put the right measures in place and do it on a global scale, with those beyond the peak helping those who are in the middle of the pandemic. What we learn in the process will allow us to better predict and prepare for the future. One thing is certain, artificial intelligence and virtual care, which are relatively new concepts to much of society, will play their part in combatting the COVID-19 pandemic. Experiencing these technologies first-hand will undoubtedly help to shape the debate about their future role in healthcare and what it means for all of us. Even if we now have to do it ‘virtually’, let’s stick together and support the world’s COVID-19 patients and those who spend endless hours and risk their own lives caring for them.

Share on social media
Topics
Author

Jeroen Tas
Chief Innovation & Strategy Officer Jeroen is an experienced global executive and entrepreneur with a track record of leading innovation in the healthcare, information technology and financial services industries. Leading the company’s global Innovation & Strategy organization, he’s responsible for creating a pipeline of innovative business propositions that address emerging customer needs and enable a high-growth, profitable health continuum strategy.
Follow me on