In mid-March, my colleague’s friend Natalie started coming down with symptoms that we’re all too familiar with these days, including a cough and extreme fatigue. The following week, she mostly carried on as normal, taking painkillers and working from home. Then on day 10 things went downhill rapidly. By late morning she could barely breathe and started panicking. Her GP told her to go to the hospital but the local ambulance service was overloaded with suspected cases of COVID-19 and said she’d have to wait eight hours. Without anyone nearby to drive her there, Natalie had to rely on an inhaler from the local pharmacy, and a lot of hope. I’m relieved to say that by the next day, her breathing had improved. But over the following weeks she also relapsed frequently and each time felt terrified by the appearance of any new symptoms. While Natalie gradually got better, she said that the worst part was not knowing how unwell she was at any given moment.
Healthcare is an industry that usually moves slower. But the COVID-19 outbreak has forced health systems and innovators to pivot and adapt quickly. We’ve made 10 years of progress in three months. Connecting care is finally becoming a reality.
This pandemic has forced health systems to pivot and adapt
Three months on and Natalie’s experience might be radically different today. The speed with which healthcare has changed is absolutely incredible. Our industry usually moves slower. But the COVID-19 outbreak has forced health systems and innovators alike to pivot and adapt quickly: countries including the US, China and the UK built thousands of intensive care unit (ICU) beds in just over one week; vaccine trials in humans started months sooner than they normally would; millions of healthcare workers left their loved ones at home to care for critically-ill patients. It’s been truly awe inspiring and heartwarming to witness. And although we’re far from out of the crisis, our industry has made at least 10 years of progress since Natalie first fell ill. One of the biggest leaps forward is that connected care is finally becoming a reality. The spread of the new coronavirus is causing surges of demand right across the continuum. And connected care is the backbone of that continuum. It stands for 24/7 care, joining preventative and personal health with acute needs and chronic care in the home, in the hospital, and in the community.
Customers are telling me that telehealth has reduced the need for PPE and is one of the most important things they have done to combat COVID-19.
Virtual care in the ICU is the new normal
But what exactly has changed? One of the main things I’m hearing from customers is that telehealth has made a huge impact. COVID-19 can cause severe pneumonia, leading to increasing numbers of patients needing care in an ICU. This is a huge worry for healthcare authorities, not simply because of the limited number of ICU beds but also because of staff shortages, burnout, and the risk that doctors and nurses will be infected by the virus themselves – an even bigger risk at the moment due to the global shortage of personal protective equipment or PPE, such as single-use gloves, face masks and aprons. An eICU enables a team of intensivists and critical care nurses to remotely monitor patients in the ICU regardless of patient location, supported by high-definition cameras, predictive analytics, data visualization and advanced reporting capabilities to support their frontline colleagues. Recently, I spoke to Eric Cucchi, a critical care affiliate practitioner at UMass Memorial Medical Center, part of the largest healthcare system in central and western Massachusetts in the US. He told me that eICU bedside camera activations increased more than 1,000% from March to over 5,000 in April, which were directly related to less PPE use and staff exposure. “It’s one of the most important things we’ve done to date. We’ve been able to build ICU surge space easily and seamlessly with full eICU support. This means that our critically ill patients receive the same level of care as the ones in our standard ICU spaces.” Meanwhile, in a recent webinar detailing their response to COVID-19, Northwell Health revealed that they’ve integrated telehealth across the entire continuum. New York’s largest healthcare provider said that they had been trying to do this for three years, and then achieved their goal in just six weeks after the outbreak. Looking beyond the eICU, Northwell has increased telemedicine visits from a few hundred to more than 50,000 since March. In today’s crisis situation, I feel humbled and immensely proud to be supporting such meaningful work with flexible and scalable solutions that help to prevent healthcare systems from being overwhelmed. Thinking back to Natalie, this week I started to imagine how her story might be different today if telehealth technology is implemented at scale.
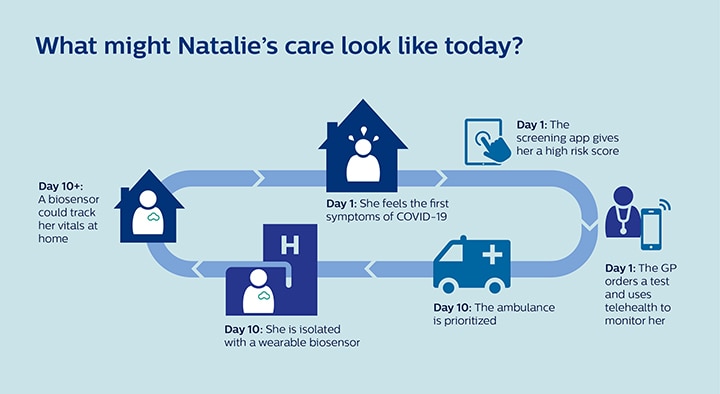
What might Natalie’s care look like today?
Let’s go back to day one, when Natalie felt the first symptoms. Her doctor suggests that she uses a screening app for COVID from her home which works out how likely she is to have the virus and need a test. When she gets a high-risk score, Natalie is then called by her GP, who sends her to be tested early. The test comes back positive, so Natalie is told to isolate at home, from where her doctor can monitor her symptoms remotely. Natalie feels unwell but calm until day 10 when she develops breathing problems. Because she’s already under care for a confirmed case of COVID-19, her need for an ambulance is prioritized and she doesn’t have to wait long. On the way to the hospital, paramedics use a hand-held ultrasound scanner to assess whether she has virus-related complications in her heart or lungs. It means the hospital is ready for her. Once Natalie arrives at the hospital, a wearable biosensor tracks her vital signs while in an isolation room. She is monitored continuously yet remotely, which helps to reduce the number of times nursing staff need to enter in PPE. Natalie is also connected to automated early detection and warning software that continuously analyzes data from the sensor to detect subtle deteriorations in her vital signs. In Natalie’s case, we know her condition improves within 24 hours. But her medical history puts her in a higher risk category, so her doctor might prescribe a different biosensor* to wear at home, which keeps her primary care team updated on her progress. This is important not only for Natalie, who gets to recover back in her own house (which we know patients usually prefer) but also for the hospital, which can focus on caring for more critically ill patients. It would also give her the peace of mind of knowing that she’s being monitored from afar – especially when new symptoms arise. At Philips, connected care is something we’ve been working towards for years. It requires integrated systems and strong partnerships that support seamless data flows and analytics between care providers and across settings. Over the past six months, the pandemic has accelerated the need among our customers and their patients and caregivers more than ever before. It means that the scenario above isn’t a vision of the future: it’s possible today. But it’s not just health systems that need to be able to pivot and adapt fast; we in health tech still have a lot of work to do to transform ourselves as well so we can be there for our customers when it matters most. I look forward to seeing how we apply the lessons from the pandemic to improve healthcare over the coming months and years. For now, I wish Natalie all the best, along with anyone who has been personally affected by the virus. My thoughts are with you. And to the amazing doctors and nurses who care for us all: thank you. * This is not the same as the wearable biosensor designed for use within hospitals.

Share on social media
Topics
Author

Roy Jakobs
CEO Philips Roy Jakobs is the Chief Executive Officer of Royal Philips. As CEO, he is also Chairman of the Board of Management and the Executive Committee.
With his extensive global executive leadership experience, Roy drives Philips’ strategy to help deliver people-centered, high-quality care.
Click here to read more on Roy Jakobs
Follow me on

