January 12, 2017
Philips announces new augmented-reality surgical navigation technology designed for image-guided spine, cranial and trauma surgery
Spine surgery was traditionally an ‘open surgery’ procedure, accessing the affected area via a large incision so that surgeons could physically see and touch the patient’s spine in order to position implants such as pedicle screws. In recent years, however, there has been a definite shift to the use of minimally-invasive techniques, performed by manipulating surgical tools through small incisions in the patient’s skin in order to minimize blood loss and soft tissue damage, and consequently reduce postoperative pain. Due to inherently reduced visibility of the spine during these procedures, surgeons have to rely on real-time imaging and navigation solutions to guide their surgical tools and implants. The same is true for minimally-invasive cranial surgery and surgery on complex trauma fractures.
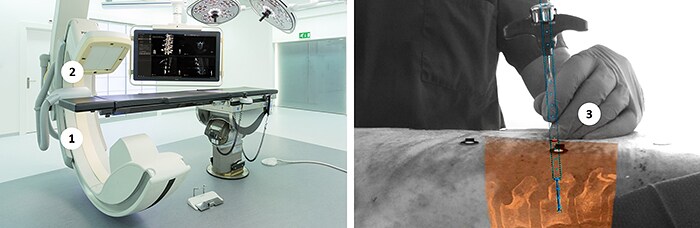
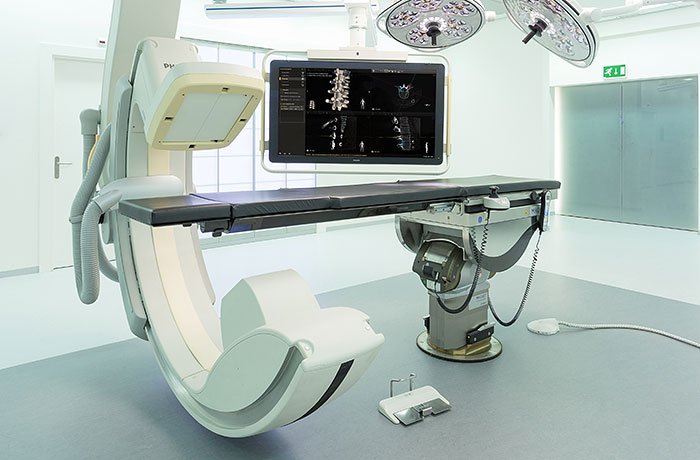
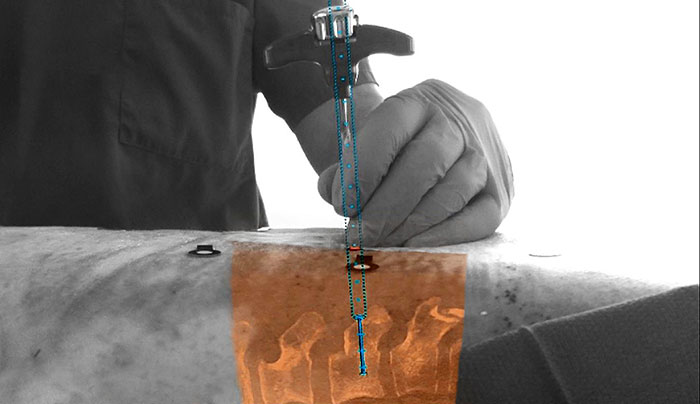
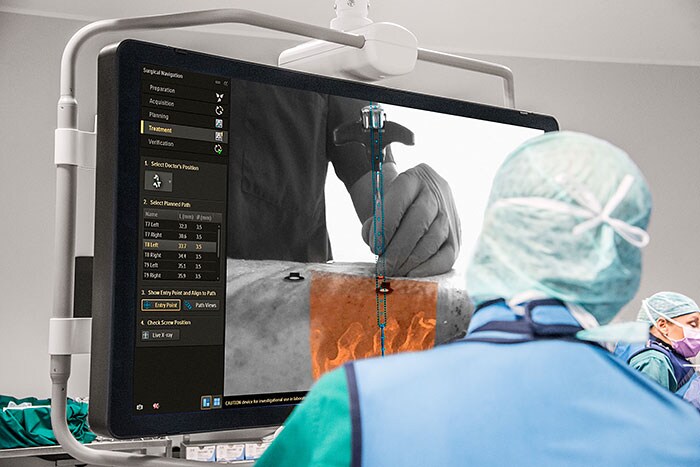
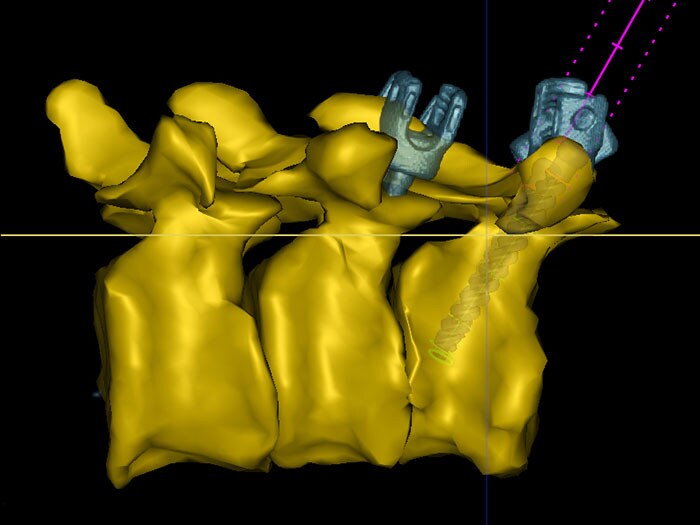
Philips is developing a new augmented-reality surgical navigation technology, which will add additional capabilities to the company’s low-dose X-ray system (1 in picture above). The technology uses high-resolution optical cameras mounted on the flat panel X-ray detector (2) to image the surface of the patient. It then combines the external view captured by the cameras and the internal 3D view of the patient acquired by the X-ray system to construct a 3D augmented-reality view of the patient’s external and internal anatomy (3). This real-time 3D view of the patient’s spine in relation to the incision sites in the skin aims to improve procedure planning, surgical tool navigation and implant accuracy, as well as reducing procedure times. “This unique augmented-reality technology is an example of how we expand our capabilities with innovative solutions in growth areas such as spine, neuro and trauma surgery,” said Ronald Tabaksblat, Business Leader Image-Guided Therapy Systems at Philips. “By teaming up with clinical innovation leaders, we continue to find ways to convert open surgery to minimally-invasive treatment to reduce post-operative pain and expedite recovery.” As part of a joint clinical research program, Philips hybrid ORs with this new capability will be installed in a network of ten clinical collaborators to advance the technology. The results of the first pre-clinical study on the technology have been published in the prestigious SPINE journal, as a result of a collaboration between Philips, Karolinska University Hospital (Stockholm, Sweden) and the Cincinnati Children’s Hospital Medical Center (Cincinnati, USA). The technology was shown to be significantly better with respect to overall accuracy, compared to pedicle screw placement without the aid of Philips’ augmented-reality surgical navigation technology (85% vs 64%, p<0.05). “This new technology allows us to intraoperatively make a high-resolution 3D image of the patient’s spine, plan the optimal device path, and subsequently place pedicle screws using the system’s fully-automatic augmented-reality navigation,” said Dr. Skúlason of the Landspitali University Hospital, Reykjavik, Iceland. “We can also check the overall result in 3D in the OR without the need to move the patient to a CT scanner. And all this can be done without any radiation exposure to the surgeon and with minimal dose to the patient.” The technology was also recently presented at the North American Spine Society Annual Meeting in Boston by Dr. Adrian Elmi-Terander of Karolinska University Hospital, Sweden. Today, Philips’ commercial hybrid OR solutions are already being used for image-guided minimally-invasive surgery (click on this link to watch the video): “Since we no longer do open spine surgery, we depend on imaging and image quality,” commented Prof. Seekamp from the Universitätsklinikum Schleswig-Holstein in Kiel, Germany. “I had expected the operations to take a little longer in the hybrid OR, but in fact just the opposite is true.” Dr. Bemelman, trauma surgeon at the Elisabeth Hospital in Tilburg, the Netherlands, said “We teamed up with vascular, neuro and orthopedic surgeons to create this multi-purpose OR to realize a high room utilization, provide state-of-the-art care and reduce the overall cost for the hospital.”
The first clinical cases using the new surgical navigation system have been successfully treated at Karolinska University Hospital. The collaboration between Karolinska University Hospital and innovation partner Philips aims to combine clinical insights, innovative image-guidance technologies and new navigation concepts to enable more precise surgery. Click here for more information.
About Royal Philips
Royal Philips (NYSE: PHG, AEX: PHIA) is a leading health technology company focused on improving people’s health and enabling better outcomes across the health continuum from healthy living and prevention, to diagnosis, treatment and home care. Philips leverages advanced technology and deep clinical and consumer insights to deliver integrated solutions. Headquartered in the Netherlands, the company is a leader in diagnostic imaging, image-guided therapy, patient monitoring and health informatics, as well as in consumer health and home care. Philips’ health technology portfolio generated 2015 sales of EUR 16.8 billion and employs approximately 70,000 employees with sales and services in more than 100 countries. News about Philips can be found at www.philips.com/newscenter.
Topics
Contacts

Steve Klink
Philips Global Press Office Tel: +31 6 10888824
You are about to visit a Philips global content page
Continue
Fabienne van der Feer
Philips Image Guided Therapy Tel: + 31 622 698 001
You are about to visit a Philips global content page
ContinueMedia assets
Press releases
Get our press releases by e-mail
You are about to visit a Philips global content page
Continue