An interesting paradox in medicine is that not all malignancy is life-threatening and, surprisingly, sometimes benign conditions can be worse. For example, let’s look at the prostate. Many men die with prostate cancer rather than from it. Very few men living with this disease – increasingly detected through innovative new approaches to diagnosis – will experience any symptoms or problems. Indeed, in one study, occult (hidden) prostate cancer was found in 36% of autopsies performed, with that prevalence reaching 60% in some subpopulations [1]. By contrast, benign complications in the prostate can be far more problematic with greater implications for a man’s quality of life.
An interesting paradox in medicine is that not all malignancy is life-threatening and, surprisingly, sometimes benign conditions can be worse.
Atul Gupta, MD
Chief Medical Officer, Philips Image Guided Therapy
Benign prostatic hyperplasia affecting men’s health
Take benign prostatic hyperplasia (BPH), a condition that will affect half of men over 50 [2] and 80% of those aged over 70 [3]. As its name suggests, it’s a non-cancerous increase in the size of the prostate gland. In some instances, it can lead to lower urinary tract syndrome, which can result in an inability to empty the bladder sufficiently. It’s a growing, and often uncomfortable, condition with a sizable economic burden on health care systems. In the United States alone, the estimated cost is approximately 3.9 billion USD [4]. Typically, a urologist will either prescribe medication or perform a surgical procedure such as transurethral resection of the prostate (TURP). While medication can occasionally offer rapid symptomatic relief, for some men a response could take months. Some medications can also be associated with negative side effects like erectile dysfunction. Although surgical TURP is regarded as a cost-effective alternative to medication, it can cause side effects that can impact a patient’s quality of life, and a recovery time of up to several weeks [5].
Prostate artery embolization gaining traction
However, there is a third route that is increasingly gaining traction: prostate artery embolization (PAE). In fact, it’s one of the most exciting areas of interventional radiology today with dedicated meetings such as STREAMpae offering attendees a comprehensive course on the procedure and new developments regarding its use. Prostate artery embolization was pioneered by the late great Professor Joao Pisco of Saint Louis Hospital in Lisbon – to whom much credit must be given. Indeed, it’s thanks to the work of Professor Pisco and his colleagues that PAE is being described as the very future of BPH treatment. A landmark study conducted by Dr. Pisco’s team including Drs. Tiago Bilhim and Nuno Costa was published in European Urology in December 2019. The team found that the improvements in subjective and objective variables after prostate artery embolization are far superior to those caused simply by placebo effect [6]. This announcement garnered a lot of attention with key opinion leaders such as Keith Pereira MD commenting on the findings.

Dr. Nuno V. Costa hosting an educational workshop on PAE During PAE, X-ray guidance is used to navigate a microcatheter into the prostate arteries, via a pinhole in the wrist or thigh. Selectively embolizing these prostatic arteries [7] causes the prostate to shrink. There are many benefits for patients: it’s less invasive than surgical TURP – yet just as effective – and it can be performed with minimal discomfort for that patient, who can go home hours after the procedure. Secondly, it’s the only BPH treatment that approaches the prostate through the arteries, leaving the urethra untouched, thereby avoiding many potential surgical complications as retrograde ejaculation, erectile dysfunction, incontinence or urethral structures. Thirdly, it may be more cost-effective than the alternatives, a key consideration. That’s not to say that this procedure is without its challenges. The pelvis has an extraordinarily complex 3D anatomy of around 15 different millimeter-sized collateral arteries on each side. That means physicians must be absolutely certain the right vessels are occluded.
The evolution of prostate artery embolization
Many hospitals and outpatient interventional centers are only just starting to perform this intricate procedure. Up to now, uptake has been impeded by the fact that operating physicians need to navigate this challenging anatomy through 2D images of the vasculature. So, imaging of the prostate-feeding arteries and guidance into the prostate is paramount to allow a safe and effective targeting of the prostate, avoiding non-target embolization to surrounding organs. Over the past 10 years, physicians such as Drs. Pisco and Bilhim have worked with cone beam CT in combination with 3D Roadmap to overcome this navigation issue. By using these solutions together, the guide wire and catheter can be navigated through complex vessel structures by providing live fluoroscopy overlay on 3D angiography.
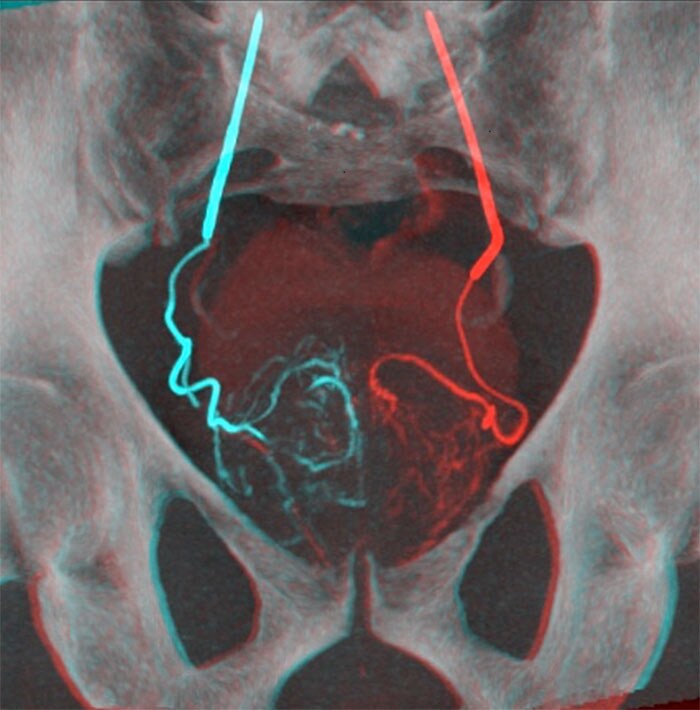
Overlay of 2 CBCT images for the embolization of the left prostatic artery and of the right prostatic artery (Image courtesy of Dr. Tiago Bilhim) I recently asked Dr. Bilhim to sum up his study assessing the outcome of PAE for patients with lower urinary tract syndrome. “The results of our recent study were encouraging and suggest that prostate artery embolization may soon become the standard of care for benign prostatic hyperplasia,” he explained. [8] [9] [10]

Dr. Tiago Bilhim, Atul Gupta, MD and the late Professor Joao Pisco As we enter a new decade, I’m encouraged to see how advances in this field – particularly those pioneered by Dr. Bilhim, the late Professor Pisco, and other leaders in the field of interventional radiology and prostate disease – are transforming the way we treat BPH patients, helping them get home more quickly and with limited side effects. With innovative approaches such as prostate artery embolization leading the way, what other advancements in interventional procedures do you see improving patient quality of life in the new decade? References [1] Brett A. S. (2013) Prevalence of Occult Prostate Cancer at Autopsy is High. NEJM Journal Watch - https://www.jwatch.org/na31811/2013/08/08/prevalence-occult-prostate-cancer-autopsy-high [2] What is Benign Prostatic Hyperplasia (BPH)? - https://www.urologyhealth.org/urologic-conditions/benign-prostatic-hyperplasia-(bph) [3] Egan, K.B. (2016) The epidemiology of benign prostatic hyperplasia associated with lower urinary tract symptoms: prevalence and incident rates. Urologic Clinics, 43(3):289-97. https://www.ncbi.nlm.nih.gov/pubmed/27476122 [4] Saigal, C. S. & Joyce, G (2005) Economic costs of benign prostatic hyperplasia in the private sector. J Urol 173, 1309–13. https://www.auajournals.org/doi/10.1097/01.ju.0000152318.79184.6f [5] Recovery – Transurethral resection of the prostate - https://www.nhs.uk/conditions/transurethral-resection-of-the-prostate-turp/recovery/#targetText=Returning%20to%20your%20normal%20activities,return%20to%20your%20normal%20activities. [6] Pisco J. et al. (2019) Randomised Clinical Trial of Prostatic Artery Embolisation Versus a Sham Procedure for Benign Prostatic Hyperplasia. European Urology. https://www.europeanurology.com/article/S0302-2838(19)30873-5/fulltext [7] Bilhim T., Tinto H.R., Fernandes L. & Pisco J.M. (2012) Radiological anatomy of prostatic arteries. Techniques in Vascular & Interventional Radiology, 15(4):276-285. [8] J Vasc Interv Radiol. 2019 May;30(5):638-644. doi: 10.1016/j.jvir.2019.02.014. https://www.ncbi.nlm.nih.gov/pubmed/31029381 [9] Pisco J.M., Bilhim T., Pinheiro L.C., Fernandes L., Pereira J., Costa N.V., Duarte M. & Oliveira A.G. (2016). Medium- and long-term outcome of prostate artery embolization for patients with benign prostatic hyperplasia: results in 630 patients. Journal of Vascular and Interventional Radiology, 27(8), 1115-1122. https://www.ncbi.nlm.nih.gov/pubmed/27321890 [10] https://cslide.ctimeetingtech.com/cirse2019/attendee/person/99056
Share on social media
Topics
Author

Atul Gupta
Chief Medical Officer, Image Guided Therapy Atul Gupta, MD is Chief Medical Officer at Philips’ Image Guided Therapy and a practicing interventional radiologist. Prior to joining Philips in 2016, Atul served on Philips’ International Medical Advisory Board for more than 10 years. Atul continues to perform both interventional and diagnostic radiology in suburban Philadelphia, in both hospital and office-based lab settings. He has been repeatedly recognized as top physician for his specialty in the media and serves on several advisory boards. He has also published and lectured internationally on a range of interventional procedures.
Follow me on













