Bridging gaps in healthcare: three key takeaways from the 2024 Future Health Index
Jun 19, 2024 | 6 minute read
Across the globe, access to care is under pressure. The 2024 Future Health Index – the largest survey of its kind – examined some of the most pressing gaps in today’s healthcare systems, how they are impacting patient care, and how healthcare leaders are taking action to bridge these gaps. This is what we found – and why I am optimistic about creating a future in which we can deliver better care to more patients.

Timely access to care is a cornerstone of a well-functioning healthcare system. However, long wait times and staff shortages are making it increasingly difficult for people to get the care they need when they need it. We find this pressure on access to care not just in remote and rural regions, but even in metropolitan areas. More than 3 in 4 healthcare leaders (77%) in this year’s Future Health Index say delays in care delivery are an issue. This dovetails with other reports, which show that, in the UK for example, the length of time patients are forced to wait for diagnostic tests and treatments such as surgery and cancer care are the worst on record [1]. But when our health is on the line, care delivery should not be delayed. Lost time means missed opportunities for early diagnosis and intervention, potentially leading to worse health outcomes and increased healthcare costs in the long run. The human and economic toll of delayed care is huge [2]. And, as one US hospital executive said during our research interviews, when clinicians are expected to take on tasks outside the scope of their role due to staffing shortages, patients are put at risk. It’s not just access to care that is under pressure – rather, quality of care is at stake too.
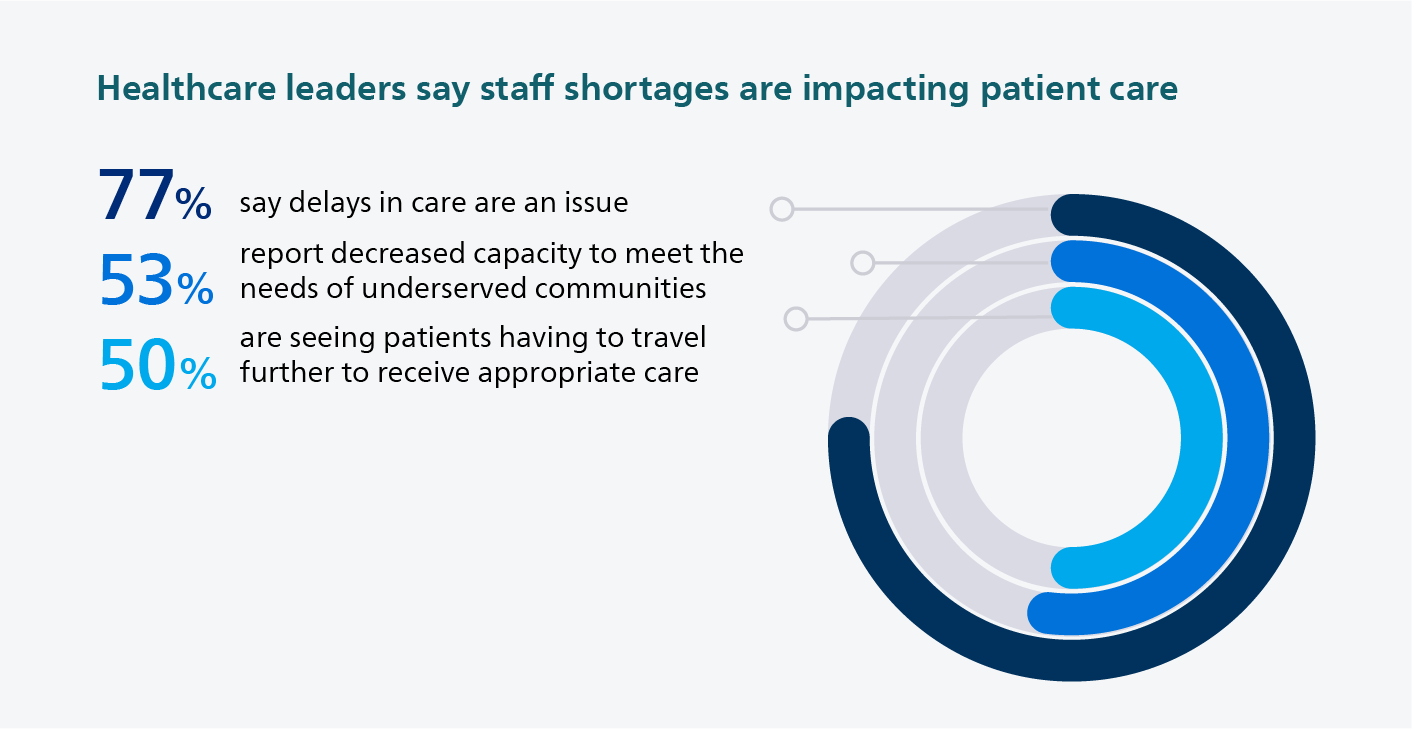
For those who already struggled to get the right care at the right time, the barriers may only be getting larger. More than half of leaders (53%) in the 2024 Future Health Index say that decreased capacity to meet the needs of underserved communities is an issue in their organization. If we don’t radically rethink how and where care is delivered, urban-rural health disparities – which have already grown significantly over the past 20 years in countries such as the US [3] – will only continue to widen. These findings paint a stark picture of the challenges that healthcare systems are facing and how these challenges are impacting patient care. Yet there is also reason for hope. Our research shows that healthcare leaders are addressing challenges head-on, using workflow automation, virtual care, and artificial intelligence (AI) to bridge gaps in healthcare and deliver better care to more patients. These are three themes that stood out for me – and what I think they hold for the future of healthcare.
1. Automation can help relieve staff shortages, if used right
Recruiting more staff is, in many cases, not a realistic option anymore. We need to alleviate the burden on existing staff, by freeing them from cumbersome administrative tasks that can be automated. Almost all healthcare leaders in the 2024 Future Health Index (92%) believe that automation of repetitive tasks and processes is critical for addressing staff shortages, and an equal percentage think it will save healthcare professionals time by reducing administrative work – allowing them to spend more time with patients.

Speaking from my own experience as a clinician, there is nothing healthcare professionals want more than time. The amount of ‘administrivia’ they must perform on a daily basis is beyond frustrating. I remember how, after completing a two-hour angiography procedure on a patient, I would spend another 25-30 minutes documenting what I had just done. And it wasn’t just me. The supporting nurse, the angio technician, the anesthesiologist – all of us sat in our own corner of the room afterwards, typing away at our reports. It took away precious time that we could have spent providing care to patients instead. So, it didn’t come as a surprise to me that clinical documentation or notetaking is among the top three areas where healthcare leaders plan to implement automation in the next three years. Sticking to the example I just gave, it would be much more efficient for technology to, for example, automatically document when the patient entered the angio room, when the catheter was inserted into the femoral artery, what kind of catheter was used, when the stent was deployed, and so on. Synthesizing all that information, generative AI could then create a pre-filled reports tailored for each clinician in the procedure, who would only need to review and approve for their purpose. By having such an intelligent ‘eye in the room’, we can make easy and effortless what used to be time-consuming.

I also understand why some healthcare professionals may have doubts about automation, as seen in the Future Health Index report. Our findings show that 65% of healthcare leaders say their staff are skeptical of automation. With high expectations often comes the concern that we may put our hope into something that ultimately falls short. Quality assurance in automation is a must. More outcome evidence of its effectiveness is essential. Most important, we should always innovate backward from the needs of clinicians, rather than pushing technology for technology’s sake. By innovating on behalf of clinicians to address their most pressing needs, we also avoid inadvertently undermining their professional autonomy (which, truth be told, I was also skeptical of when I was a practicing doctor). Used right, automation is not about replacing the skills of physicians – it’s about liberating them from tedious work they shouldn’t be doing in the first place.
Automation is not about replacing the skills of physicians – it’s about liberating them from tedious work they shouldn’t be doing in the first place.
2. Virtual care can extend the reach of patient care
Healthcare leaders see virtual care as another way of bridging the staffing gap. Last year’s Future Health Index showed how healthcare leaders continued to build out virtual care services after investments peaked during the pandemic. But is it actually working? This year’s survey offers a resounding ‘yes’. Almost 9 in 10 healthcare leaders (89%) are seeing a positive impact of virtual care in easing staff shortages in their organization – whether it’s through increased capacity to serve patients, improved collaboration between staff in different locations, or a reduced need for on-site staff in certain roles. That’s particularly good news for patients who find themselves in remote or rural areas where specialist staff is in short supply. Almost 1 in 3 healthcare leaders worldwide (32%) say virtual care is enabling them to expand specialist care to underserved communities. Our data shows this is especially the case in China, India, and the US, where patients may have to travel long distances to see a specialist care provider. Healthcare leaders from those countries also report decreased clinical response time in our survey, giving patients a better chance of early diagnosis and treatment.

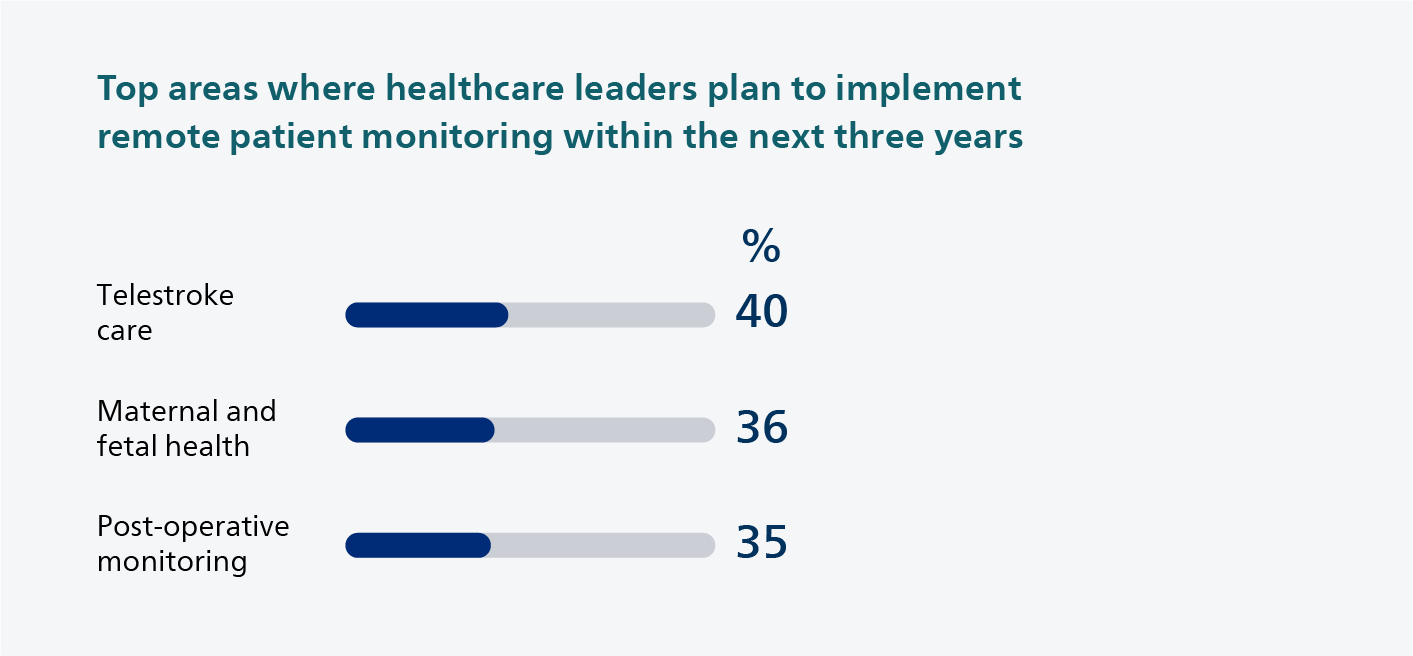
What’s equally encouraging is that healthcare leaders continue to implement remote patient monitoring, indicating a further shift in care from the hospital to the home. Over the next three years, their top areas of investment in remote patient monitoring include telestroke care (40%), maternal and fetal health (36%) and post-operative monitoring (35%). It’s a trend I only expect to gain further traction. Hospital staff is stretched. Beds are scarce. The sooner you can send a patient home, while closely monitoring their health, the better. It offers patients a better experience because they can recover in the comfort of their home or a lower-acuity care setting. It frees up hospital capacity for the next patient. And it also creates new career paths for experienced staff, such as virtual nursing, which can help keep critical expertise in healthcare.
3. Leaders are embracing AI while also calling for appropriate safeguards
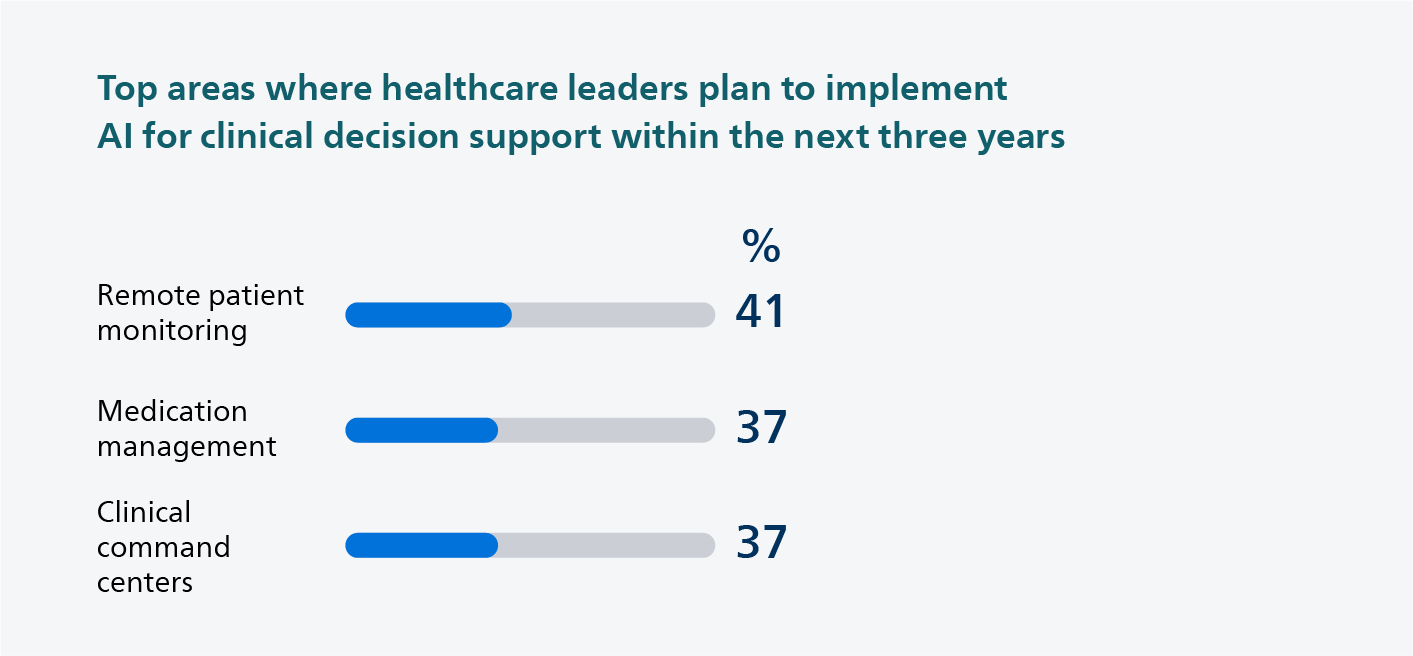
There’s no way of getting around it: AI continues to dominate the conversation about innovation in healthcare, and with good reason. Almost 4 in 10 healthcare leaders (38%) in the 2024 Future Health Index say that staff lose precious time accessing or integrating different patient data, leaving less time to care for patients. There’s no lack of data in healthcare. On the contrary, there’s typically too much of it. What’s often lacking are ways to pull all that disparate data together and turn it into a cohesive patient story that helps clinicians decide what to do next. Clinicians face a wealth of data, but a gap in insights. And AI – built on top of open platforms that liquidate data from different systems and devices – is the way to bridge that gap. Our survey findings show that healthcare leaders are embracing this opportunity full-on. In fact, they have already implemented AI for clinical decision support across different areas of the hospital, with in-hospital patient monitoring, treatment planning, and medication management leading the pack. As leaders increasingly focus on expanding care beyond hospital walls, implementing AI in remote patient monitoring is an area of focus for the next three years. That makes perfect sense, as AI-enabled remote patient monitoring could help predict, for example, if a patient is at risk of developing atrial fibrillation, allowing for early intervention to prevent adverse outcomes.
At the same time, healthcare leaders are also calling for a measured approach to AI. Almost 9 in 10 of them (87%) are concerned about the possibility of data bias in AI applications widening existing disparities in health outcomes. Mitigating this risk is indeed critical. For example, if an algorithm is trained on a tailored data set from patients in a US city, we can’t expect it to perform as well for patients in a city in Asia – or vice versa. We must train AI models with sufficient volume and variety of diverse, high-veracity data to ensure that it can effectively address the specific healthcare needs of various populations and regions. In line with recent recommendations from the American College of Radiology [4], I also foresee the need for increased post-market surveillance to continually monitor the real-world performance of AI applications in diverse healthcare settings. This ongoing evaluation will help identify and address any emerging biases, drift, or performance decay – ensuring that AI truly helps to deliver better care for all.
Find out more in the full report
I invite you to explore the survey findings in more detail in the full Future Health Index 2024 report and reflect on what they mean for your organization. How can smart and responsible use of AI, automation, and virtual care help address gaps to deliver better care to more patients? I hope you find inspiration from your fellow healthcare leaders in the report!