Making every moment count: how live patient stories can support proactive critical care
Mar 04, 2024 | 3 minute read
In critical care, time is of the essence – but there’s always a lack of it. By automatically bringing disparate patient data together in real time, we can create a live, digital view into each patient’s clinical story as it unfolds in the moment, with actionable alerts helping critical care providers decide what to do next in the moments that matter.
I still remember to this day what it felt like to be a young doctor working in a hospital in a small Canadian city. There I was, fresh out of medical school, tasked with everything from monitoring critically ill patients in the intensive care unit (ICU) to delivering babies overnight and then back to the general ward attending to post-operative patients. I wanted to experience and learn it all. But nothing could have prepared me for the constant stress and overwhelming number of decisions we had to make every day, based on thousands of data points collected from monitors, ventilators, intravenous pumps, and other devices – not to mention lab results, imaging data, and various notes about the patient history. Each morning, we would gather in a huddle of specialists and nurses for a summary briefing, going over all the patients’ data from the night before to construct patient stories that would guide our next actions. Because we typically only had one hour to discuss dozens of patients, there was no room for long expositions. We needed concise interpretations of the most critical information. Often, that meant having to condense a vast array of overnight data points into 3 short sentences – relying on each specialist to render their interpretation. The right specialist was not always available, which meant we had to revisit the same information later in the day. While we were attending to one patient, another patient’s health would sometimes unexpectedly take a turn for the worse, calling for a rapid response. We all made it work together as a team – but at the end of a shift, I couldn’t help wondering if we would have made different decisions if we had had more time and resources. I was constantly second-guessing myself. Times have changed. A lot of the information we used to capture on paper is now stored digitally, in the electronic medical record (EMR). But in many ways, working in critical care has only gotten more challenging. Staff shortages have intensified [1], especially in rural areas [2], while the number of critically ill patients keeps rising as populations continue to age [3]. Information overload is also mounting, with an adult patient in critical care now generating up to 2 GB of high-fidelity data per day [4]. It is creating a perfect storm of challenges, with critical care providers having to attend to more patients and more data with fewer resources and less time. What’s more, clinicians are telling me that patient family members – especially younger ones who have grown up in an era of instant access to information – expect more real-time updates about their loved ones, adding further pressure on care teams. How, then, do we keep critical care sustainable and accessible for everyone in the face of increasing demand? Adding more doctors or nurses is no longer a realistic option in most places. What is needed are new and scalable technologies that can streamline workflows and empower frontline staff to offer the same level of high-quality care across locations, more confidently and more efficiently. I believe there are three elements to this that build on each other – all of which revolve around how we can use real-time data insights to create live, digital patient stories that support care teams in making proactive, informed decisions. Let me explain:
1. Bringing patient data together in one unified view
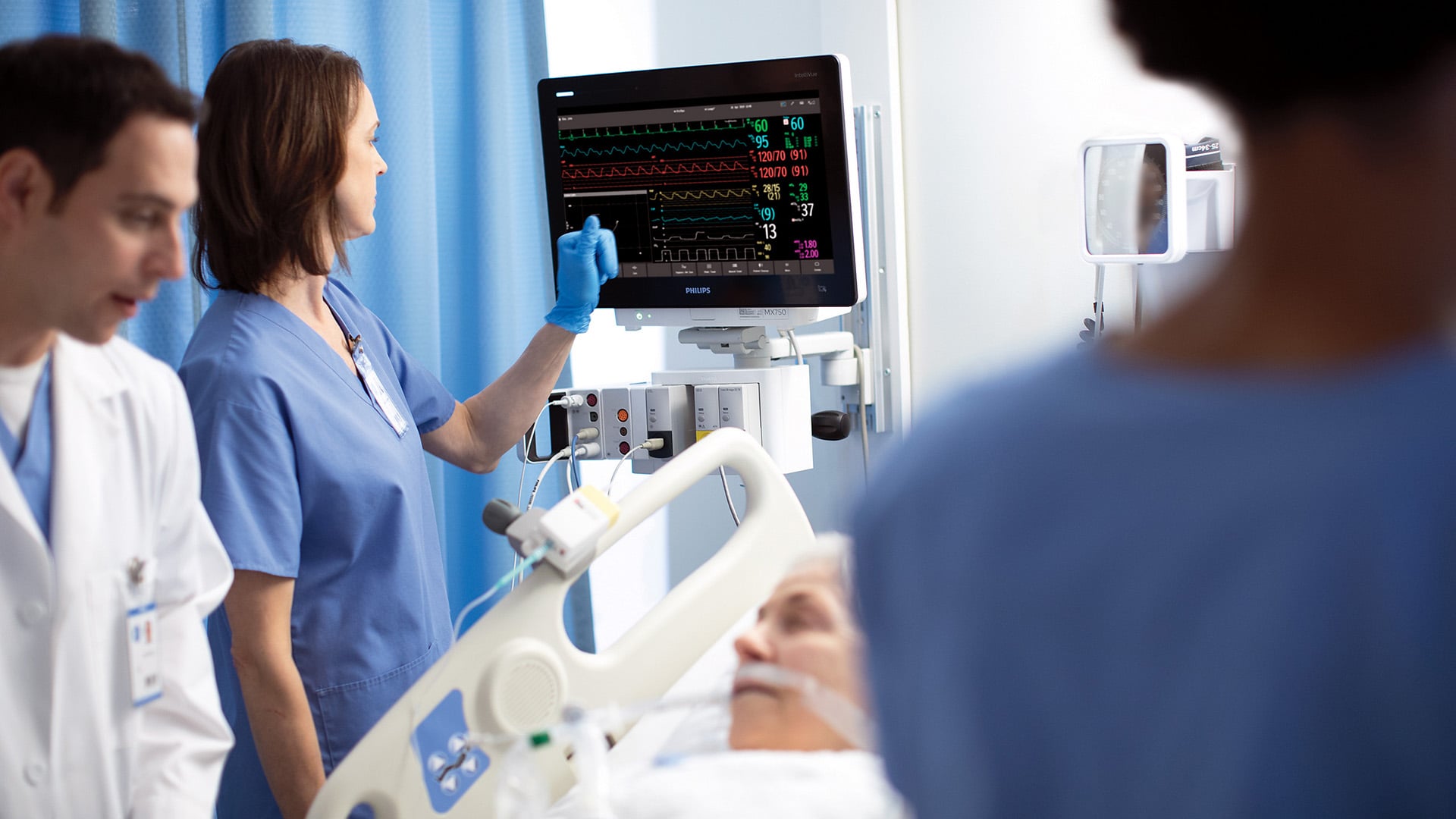
In critical care services where patients are sedated and intubated, it is often said that data speaks for the patient, because the patient cannot speak for themselves. But when that data is spread across many different devices, monitors, and systems on an ICU floor, it can be hard to know what the data is telling you. It was one of the biggest challenges my colleagues and I faced in my early days as a physician, and data fragmentation continues to be one of the biggest headaches for critical care providers today. To make an informed decision about a patient, you need a complete picture of the patient’s health history and their current condition. Plus, in a critical care setting, you don’t just want to know what happened in the past hour. You want to know what’s happening right now. Only part of a patient’s data is captured in the EMR, and typically not at the frequency that is needed to detect rapid changes in a patient’s condition. Those changes can sometimes occur within seconds, rather than minutes or hours. You need to be able to aggregate both low- and high-frequency data from a variety of devices such as ventilators, infusion pumps, and vital signs monitors – often from different vendors – to create a fine-grained patient story that enables you to act swiftly in the critical moments that matter. That’s why, at Philips, we have created an open patient monitoring ecosystem, where data flows freely across devices and systems from different vendors – coming together in a single, standardized view that can be accessed from anywhere in the hospital, whether it’s at the central station or on a mobile interface. Care teams no longer have to inspect separate monitors and devices one at a time to put a patient story together. Instead, all relevant data is available to them in one place. This kind of medical device integration and vendor-neutral interoperability is already helping healthcare organizations to improve clinical efficiency and data accuracy, while at the same time freeing up nurses for more patient-centered care.

2. Turning data into insights for advanced clinical surveillance
Bringing disparate patient data together doesn’t on its own tell a meaningful story. The bigger challenge and opportunity is to turn abstract waveforms and streams of numbers into actionable insights that help you understand what to do next. It’s about synthesizing the past and the present to predict the future. Without this, having more data only adds to the cognitive load for caregivers, making clinical interpretation even harder – especially for more junior nurses or physicians, like in my own early days. Separating signal from noise is a huge challenge for critical care providers today. An estimated 80% to 95% of alarms coming from monitors and devices are clinically irrelevant, causing unnecessary stress and distractions that can lead to alarm fatigue [5]. At the same time, it can be easy for care providers to overlook clinically meaningful information, such as a patient’s deteriorating condition – especially if the signs are subtle and only visible when viewed in relation to each other. For example, an elevated heart rate alone may not be reason for concern. It could simply be due to natural variability. But if a patient’s heart rate is trending up while their respiratory rate is also going up and blood pressure is dropping, that could be a sign of impending sepsis or another serious complication that calls for rapid intervention to avoid adverse patient outcomes. These are the early warning signs you don’t want to miss. This is where smart rules can make a difference compared to traditional alerts. Smart rules analyze data points in relation to each other to identify clinically meaningful patterns, rather than triggering alarms based on single parameters. That’s how we can provide care teams with actionable alerts of emerging events, while simultaneously reducing non-actionable notifications. It gives them more confidence that they are acting on the right signals, without overlooking significant changes in the patient’s condition. It also creates a better healing environment for patients and their families, saving them unnecessary anxiety from constant beeps that have no clinical significance. Everyone benefits. Today, these smart rules are based on a combination of clinical expertise and evidence-based protocols, developed in close collaboration with clinicians. With further advances in AI, we can expect to see increasingly sophisticated algorithms that help care providers predict and prevent adverse patient events before they occur. Over time, these algorithms will be able to offer increasingly personalized recommendations, comparing a patient’s data with thousands of similar patients to help care teams decide on the best course of action for each patient, based on their unique and ever-evolving story. It’s another reason why taking an open ecosystem approach is so important. Once we set data free in a secure way, via open and scalable platforms that third-party algorithm developers can integrate with, the possibilities for clinically relevant AI development become limitless.

3. Offering virtual support at the bedside
Equipped with advanced analytics and AI that help detect the onset of emergent conditions, we can also scale the expertise of scarce critical care providers more effectively – using in-house virtual care. This enables them to keep a watch on larger numbers of patients, while offering remote guidance and support to less experienced colleagues. Having such a second pair of eyes can give care teams at the bedside the confidence they need to act decisively when it matters. Especially in remote or rural areas, it can be a powerful way of addressing staff shortages while also raising the standard of care. Virtual care models such as e-ICU programs have been shown to reduce both mortality rates and the length of stay for a patient [6]. I recently sat behind an e-ICU station myself, and was struck by how it offered a cockpit-like experience, with simple color codes helping to prioritize which patients to attend to first based on their anticipated trajectory. As someone who grew up watching Star Trek, I was always captivated by the highly technologically advanced ‘sickbay’ depicted in the iconic science-fiction series. Not only could doctors get a single view of the patient’s medical history with the snap of a finger, but they could also consult a smart virtual assistant for real-time support with diagnosis and treatment. It was precisely the sort of support I wish I had during my first year of clinical practice, when I was constantly second-guessing myself. Some say the future shown in Star Trek is still far away. But I say we are steadily moving in that direction with advancements in technology. Virtualization makes it possible to provide high-quality care to patients regardless of their location. Advanced analytics and predictive insights can help care teams act more proactively. As we continue to advance in this direction, we will be able to provide better care to more patients in a way that is not only more efficient, but also personalized to each patient’s unique story as it unfolds in the moment. That’s a prediction I’m willing to make. To learn more about how Philips is partnering with healthcare providers to help them create a live digital view into each patient story, join us at the upcoming HIMSS 2024 conference in Orlando, Florida. You can also follow @PhilipsLiveFrom for updates from #HIMSS24.
Sources [1] Vincent, J.L., et al. Ten areas for ICU clinicians to be aware of to help retain nurses in the ICU. Crit Care 26, 310 (2022).
[2] https://www.chiefhealthcareexecutive.com/view/rural-hospitals-struggle-to-find-workers-and-not-just-doctors
[3] Akinosoglou, K., et al. The impact of age on intensive care. Ageing Res Rev. 2023 Feb;84:101832.
[4] Based on Philips historical data collected at customer sites using Data Warehouse Connect.
[5] Lewandowska, K., Weisbrot, M., Cieloszyk, A., et al. Impact of Alarm Fatigue on the work of Nurses in an Intensive Care Environment - A Systematic Review, Int J Environ Res Public Health. 2020;17(22):8409.
[6] Lilly, C.M., et al. A Multi-center Study of ICU Telemedicine Reengineering of Adult Critical Care. CHEST. 2014 Mar; 145(3): 500-7.
Share this page with your network