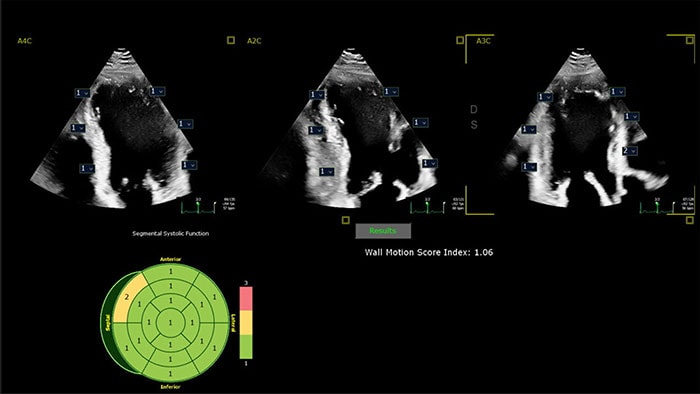
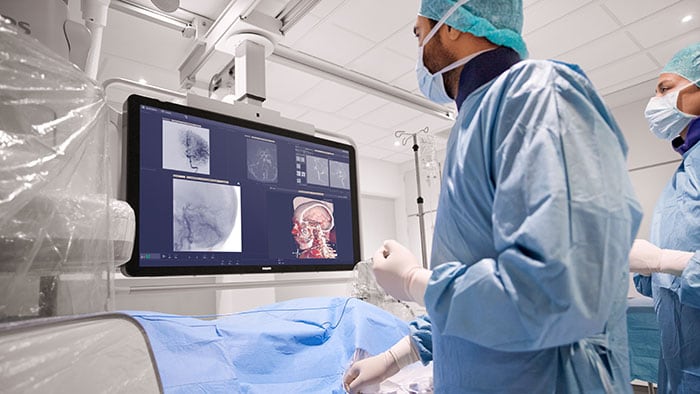
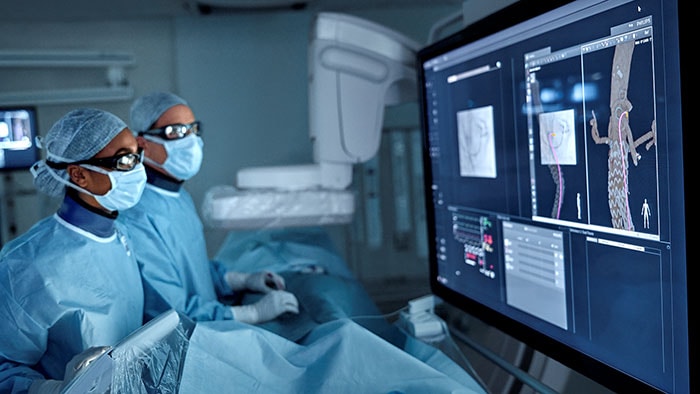
The growth of image-guided therapy procedures in the hospital has transformed the patient experience and enabled a wave of procedural innovation in cardiovascular care and beyond. Procedures that would have required major surgery a generation ago can today be carried out with just a small incision, often no larger than a pencil point, resulting in faster recovery times and more efficient care.
As image-guided therapy has grown to become a common part of many hospitals, procedures – particularly coronary and peripheral vascular procedures to restore blood flow around the heart and in the legs to help save lives and limbs – have become routine. Over the past decade, providers in some U.S. states have taken the lead in a new frontier: to take minimally invasive procedures outside of the hospital and bring them closer to patients’ communities. This movement has helped reduce costs, improve access to care, decrease waiting times, lower the risk of healthcare-associated (nosocomial) infections and improve the patient experience, while freeing hospitals to focus on more complex cases.
The first generation of facilities, primarily treating patients suffering from peripheral vascular disease, are called office-based labs. More recently, they have been complemented by the rise of ambulatory surgery centers, which can carry out a broader range of procedures including low-risk percutaneous coronary interventions (PCIs). The two models are also increasingly combined, with a facility operating as an office-based lab on some days and as an ambulatory surgery center on others.
General and Vascular surgeon Dr. Jim Melton, D.O., co-founded one such facility in Oklahoma City, Oklahoma, U.S. “Patient outcomes and patient satisfaction are the main drivers behind our success. Ambulatory surgery centers are a setting where you can pay more attention to your patients. You have pretty much one-on-one nursing. And you also typically have lower infection rates than hospitals, simply because it’s a smaller, more dedicated space.”
Patient outcomes and patient satisfaction are the main drivers behind our success.
Dr. Jim Melton D.O.
Co-founder of the CardioVascular Health Clinic in Oklahoma, U.S.
“Our patients can require treatment for a range of conditions including peripheral artery disease, varicose veins, coronary artery disease, heart disease, enlarged male prostate, patent foramen ovales (a hole between two upper chambers of the heart), coronary artery disease, uterine fibroids and end-stage renal management,” Dr. Melton continued.
Lindsay Pack, General Manager for Procedural Solutions at Philips, recently saw the direct benefits of one such facility when a family member told her of the pain she was suffering due to ulcers on her toes that would not heal. “Due to my field of work it was immediately apparent to me that her problem might be more than skin deep. Even though it was the holiday season, I was able to quickly connect her with a facility in her area that used state-of-the art equipment to perform a revascularization procedure, restoring blood flow and saving her leg. Today her ulcers have healed and she’s up and walking. The atmosphere in the outpatient setting was so reassuring, and she was more comfortable and confident than during previous experiences she’d had in a hospital environment.”
Another benefit of carrying out minimally invasive procedures in ambulatory surgery centers and office-based labs in the U.S. is cost. Health insurance policies often require patients to cover a significant amount of treatment costs out of pocket. “It’s not uncommon in the U.S. for health insurance policies to have a $5,000 deductible. If a patient goes to a large hospital for something like a left heart catheterization, for which the hospital charges way over $5,000, they would have to pay that full amount. We can do it for far less than that figure, which is a huge benefit financially to the patient,” Dr. Melton said.
Adding resilience to the healthcare ecosystem
With many hospitals suspending elective care during the COVID-19 pandemic, office-based labs and ambulatory surgery centers have in some cases been valuable in providing continuity for elective care. “We’ve seen a dramatic increase in demand during the pandemic as many patients don’t want to go to the hospital,” Dr. Melton said.
The additional resilience that office-based labs and ambulatory surgery centers add to the total healthcare ecosystem will continue to be an asset in addressing the backlog of patient care resulting from the pandemic, and any future constraints, efficiently and cost-effectively. That is particularly the case when earlier diagnosis and treatment of conditions such as peripheral arterial disease (PAD), can significantly improve patient outcomes [1].
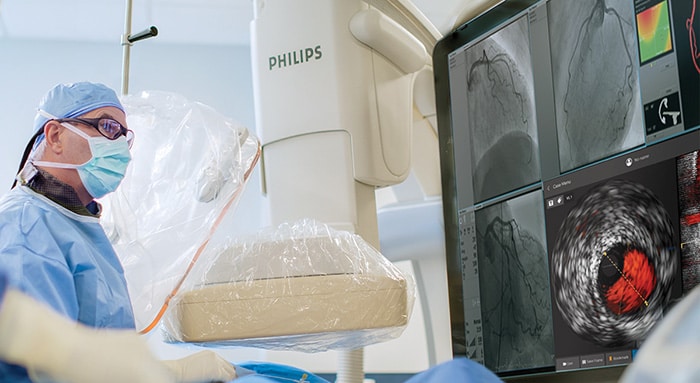
Increasing support and efficiency to lower costs
“The overhead costs for ambulatory surgery centers, which can be physician-owned, part of a larger network in a joint venture with a hospital, or part of a hospital, can be substantially lower, so even though they receive a lower level of reimbursement, they can use that money more efficiently to treat patients,” Pack said. In addition, as ambulatory surgery centers don’t treat emergency cases, they can also avoid challenges with scheduling, planning their workflow more efficiently.
The overhead costs for ambulatory surgery centers can be substantially lower, so even though they receive a lower level of reimbursement, they can use that money more efficiently to treat patients.
Lindsay Pack
General Manager for Procedural Solutions at Philips
An important enabler for innovation in the space are regulatory bodies, with the Centers for Medicare & Medicaid Services (CMS) playing a key role in the U.S., where it is responsible for setting reimbursement rates for procedures both in the hospital and other care settings. Over the past decade, CMS has set a trend by approving coverage for a greater number of procedures in out-of-hospital settings, most recently adding low-risk PCI for ambulatory surgery centers in 2020, and drug eluting stents and coronary atherectomy (a common procedure to open a blocked artery around the heart) in 2021.
Philips is also engaging with state legislatures to lower the barriers to entry for prospective ambulatory surgery centers. “While some states such as Oklahoma, Texas, Arizona and Florida have a thriving network of ambulatory surgery centers, others are playing catch-up. State regulations can be unclear and sometimes restrictive in terms of which cardiac procedures are possible in the ambulatory surgery center. State Department of Health guidelines, laws, and ‘certificate of need’ requirements can make the research and application process complex. Most physicians seek help from experienced consultants to navigate the rules and regulations of a given state,” Pack said.
The specific details of reimbursement can also have a significant impact on patient care. “In general, we now have codes (the CMS payment structure) where ambulatory surgery centers can apply for reimbursement for coronary procedures. But it’s still limited to a bundled payment, and often doesn't call out the specific clinical tools physicians use in the hospital to better diagnose and treat their patients. For example, based on research we know that PCI procedures using our iFR physiologic guidance technology can improve outcomes and reduce angina for patients more effectively than treatment guided by angiography alone, but not having a specific reimbursement code for the use of this technique makes it less likely it will be used. We’ve come a long way but there are more opportunities for the future,” Pack continued.
Changing the landscape of healthcare
Looking further into the future, Dr. Melton sees an important role for ambulatory surgery centers across the U.S. “I firmly believe that ambulatory surgery centers are the future for cardiovascular and vascular care, and definitely encourage hospitals to join forces with physicians and build such a facility beside every hospital to take care of their patients.”
I firmly believe that ambulatory surgery centers are the future for cardiovascular and vascular care.
Dr. Jim Melton, D.O.
As to whether more procedures will migrate to the ambulatory surgery center, Dr. Melton is optimistic: “As far as procedures coming down the road, I think Transcarotid Artery Revascularization (TCAR) and Endovascular Aneurysm Repair (EVAR) will eventually head to the outpatient space. And we are already planning to carry out embolization for oncology patients.”
In the U.S., office-based labs and ambulatory surgery centers are quickly becoming an integrated part of the health provider landscape, providing an environment for low-risk, high-volume procedures and enabling hospitals to focus on high-risk, high-reimbursement patients who need the complex treatment that only they can provide. “We know that lack of access to care drives poorer outcomes, so providing more opportunities for care, reducing waiting times, and getting more complex and more urgent cases into the hospital faster really is a win-win situation, making office-based labs and ambulatory surgery centers a model that could work in many other parts of the world,” said Pack.
Providing more opportunities for care, reducing waiting times, and getting more complex and more urgent cases into the hospital faster is a win-win situation.
Lindsay Pack
Philips supports office-based labs and ambulatory surgery centers as a complimentary site-of-service to hospitals, helping physicians provide quality care in the U.S. through its packaged office-based labs and ambulatory surgery center solution, SymphonySuite, and globally through its integrated portfolio, Philips is bringing image-guided therapy closer to patients worldwide.
With thanks to Dr. Jim Melton, D.O., co-founder of the CardioVascular Health Clinic in Oklahoma, U.S.
[1] In the U.S., 50% of patients who receive a non-traumatic lower limb amputation die within five years. Methodist Debakey Cardiovasc J. 2012 Oct-Dec; 8(4): 10–14.
Share on social media
Topics
Contact

Mark Groves
Philips Global Press Office Tel.: +31 631 639 916
You are about to visit a Philips global content page
Continue
Fabienne van der Feer
Philips Image Guided Therapy Tel: + 31 622 698 001
You are about to visit a Philips global content page
Continue
Dr. Jim Melton D.O., co-founder of the CardioVascular Health Clinic in Oklahoma, U.S.

Lindsay Pack, General Manager for Procedural Solutions at Philips