With costs of cardiovascular (CV) care rising to unsustainable levels, there is a strong need to transform CV health systems. Physicians, healthcare administrators and the industry need to join forces – in a so-called TRIAD Model – to reinvent cardiovascular care with a frontier mindset, exploring new payment and risk-sharing models, leading to better outcomes and improved patient and staff experiences, at lower cost.
In 1856, Rudolf von Koelliker and Heinrich Müller were the first to discover that the heart generated electricity. The pioneering spirit of these two physiologists, working together towards a truly incredible breakthrough, paved the way for what we now know as one of the cornerstones of cardiovascular medicine: electrocardiography. I sensed that frontier mentality earlier this summer at a cardiology meeting I had the pleasure of attending with my colleague Bert van Meurs, our Chief Business Leader of Image Guided Therapy. The event was the 7thCardiovascular Service Line Business Round Table meeting, which took place at the Heart & Vascular Hospital of Hackensack University Medical Center, New Jersey. Since 2016, Philips has organized these meetings around the TRIAD Model, which aims to bring together the physician, healthcare administrative and industry leadership responsible for cardiovascular services. During a particularly lively panel session Tim Attebery, CEO of the American College of Cardiology (ACC), gave a thought-provoking and challenging keynote lecture entitled “Step up, engage and lead”, about the need to transform today’s cardiovascular care systems with a frontier mindset.

From left to right: Bert van Meurs, Chief Business Leader Philips Image Guided Therapy; Jan Kimpen, Chief Medical Officer, Royal Philips; and Tim Attebery, CEO of the American College of Cardiology (ACC)
Why do things need to change? Cardiovascular disease takes a heavy toll not just on the health of populations - in the 2019 Future Health Index (FHI) report, 34% of individuals across the 15 countries surveyed said they have cardiac-related health issues -; it contributes to the burden and cost of national healthcare expenditures throughout the world. In 2016, for example, cardiovascular diseases cost a staggering $555 billion to the US economy – 15% of overall healthcare spending – and these costs are projected to reach $1.1 trillion by 2035 . Also bear in mind that 30% of these costs are so-called ‘avoidable’ costs, attributed to waste and inefficiencies in healthcare. We’re making progress. The crucial transition from fee-for-volume to value-based healthcare is underway. And as I discussed in a blog earlier this year, the demand for efficient and connected cardiovascular care is growing strongly. Against the backdrop of the rise of chronic diseases and population aging, this presents new challenges and opportunities for healthcare providers who need to keep their operational costs in check while providing the highest quality care. However, according to Attebery, we need to do more. Today’s cardiovascular care organizations are not coordinated, managed, operated or led in a way that is needed to take on the challenges ahead.
We need radical change, not just tweaking. Industry partners and suppliers need to play an active role by taking a share in the risk for improved outcomes.
There is growing awareness that things have to be changed radically, and not just tweaked. We need new ways of thinking and operating in order to bring a value-based care system to fruition. What are these new ways of thinking and operating? In his inspiring keynote, Attebery argued that industry partners and suppliers need to play an active role in the cardiovascular care transformation – through strategic and financial support, but also by taking a share in the risk for improved outcomes. Indeed, he said that there are three basic ways to increase the value of healthcare: decrease the price, improve the outcomes, or take more risk. With value-based care, generated value is defined as outcomes over cost. But, as Attebery rightly explained in his keynote, we tend to forget that risk can contribute to value as well. At a time when the healthcare industry is changing rapidly, health systems are exposed to new risks and an unknown future. Just doing nothing in the hope of avoiding exposure is in itself risky because others will simply change around us. We do not know with certainty what the outcomes of capital investments will be, nor do we know how patients will respond to the changing healthcare environment. But uncertainty is exactly where investment, innovation and success are born. Adding risk is adding value. If this is this case, how can healthcare system stakeholders work together to transform cardiovascular care systems, while generating more value by taking on more risk? This is exactly where the TRIAD Model comes in. It’s based on the premise that different groups tackle problems differently and can learn from one another and progress if they are brought together in a dynamic joint leadership team under shared accountability. The model forms the central theme of our Cardiovascular Service Line Business Round Table meetings. We invite physicians, healthcare administrators and the industry to join forces to reinvent cardiovascular care through collaboration, joint design of systems and services, and a joint offering, which also takes into account sharing risk. This means payments based on risk, and tied to the value generated and captured.
It’s a new way of approaching business for us. But we know that innovation cannot happen without uncertainty.
It’s a new way of approaching business for us, and one we’re still exploring. But we strongly believe that healthcare providers, health insurance providers, government payers and the healthcare industry have a major, shared role to play in a culture of continuous improvement, expanding value-based care from pilot projects into an operational model that can be quickly scaled up. And with our track record of more than 128 years of innovation, we know that innovation cannot happen without uncertainty, and that failure can be one of the greatest lessons. Given the unmet potential and pressing need to make healthcare more sustainable, we know we must seek out and explore innovative payments that share the risk and align incentives across care pathways and providers together with our TRIAD partners. One of the ways we’re starting to do that is by selling more end-to-end solutions in partnerships with our customers, increasingly using shared-risk payment models that relate very much to the new reimbursement models that Tim Attebery talked about. Examples of such initiatives include our pioneering risk-sharing agreements with two medical centers based in the southeastern region of the US: Ballad Health’s Holston Valley Medical Center for coronary procedures, and our more recent agreement with Atrium Health’s Sanger Heart & Vascular Institute.
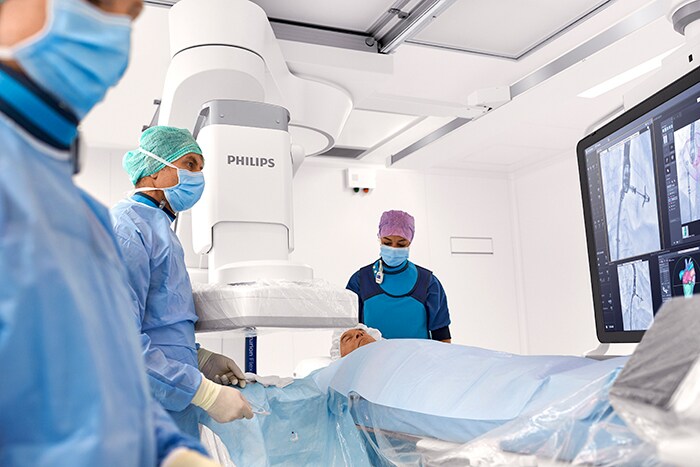
Azurion with FlexArm sets a new standard for patient imaging and positioning flexibility for image-guided procedures.
In November 2018, we took a bold step of advancing value-based care together with Sanger Heart by signing a risk-sharing agreement that links Philips’ advanced imaging technology capabilities to the achievement or avoidance of critical outcomes for patients with peripheral vascular (PV) disease. Led by the Philips Image Guided Therapy Devices business, this is the industry’s first risk-sharing agreement in the US for PV-specific procedures. Ultimately, we want to improve care with better patient outcomes, improved patient experience, improved staff satisfaction, and a lower cost of care. Doing so through the widespread adoption of value-based care requires openness, trust and strong collaboration and partnerships between all healthcare stakeholder groups. And there are good reasons to be optimistic: I see so much positive energy, engagement, and motivation to change the future of cardiovascular care in the members of the TRIAD partnership. Just like the physiologists von Koelliker and Müller, it feels like we’re on the brink of a fantastic leap forward. And it’s with their same pioneering mentality that I also feel we’re ready to meet the challenges ahead of us. [1] American Heart Association, ‘Cardiovascular disease: A costly burden for America – Projections through to 2035’
Share on social media
Topics
Author

Jan Kimpen
Chief Medical Officer, Royal Philips Before joining Philips in 2016, Jan Kimpen, Professor of Pediatrics, was CEO of the University Medical Center in Utrecht. He leads the global clinical team of Philips, focusing on advocacy, customer partnerships, clinical research and medical consulting, and is responsible for the annual publication of the Philips Future Health Index. He is a strategic advisor for commercial and clinical strategy, market reimbursement, R&D roadmaps and partnerships and M&A, and provides thought leadership on relevant clinical and medical topics. Jan participates in the WEF Global Future Council on Healthcare, the American Heart Association alliance and the Board of Sanara Ventures in Israel. Jan is president of COCIR, the European trade union for imaging, healthcare informatics and radiotherapy.
Follow me on












