By Robert Metzke
Chief of Staff Innovation & Strategy and Head of Sustainability, Philips
With the increasing scarcity of critical raw materials and growing waste mountains, a transition towards circular economic models is the only way forward. At Philips, we believe that digitalization is becoming a major catalyst for more efficient use of resources and a faster shift towards sustainable models of healthcare, including wider access to care. Let me outline how I see this happening, discuss some implications, and invite you to join forces.
The need for change
In healthcare, the combined burden of growing and aging populations and the rising incidence of chronic diseases has created a pressing need for models of care delivery that are truly sustainable. And this at the very time when we need to tackle climate change and the huge global increase in our environmental footprint, with consumption currently running at around 1.7 times the resource capacity of the planet[1]. Acutely aware that public health and a healthy environment go hand in hand, healthcare providers and professionals are increasingly looking for clinical solutions and services that also help them embed sustainable practices in their day-to-day operations. Requests for Proposals (RFPs), for example, today often contain a substantial sustainability component.
Circular economy supporting sustainable healthcare
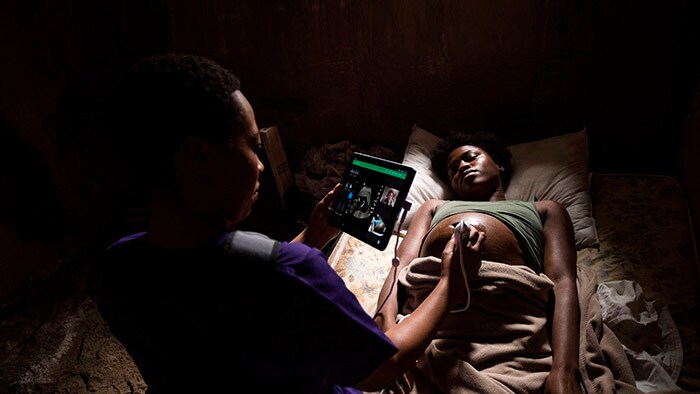
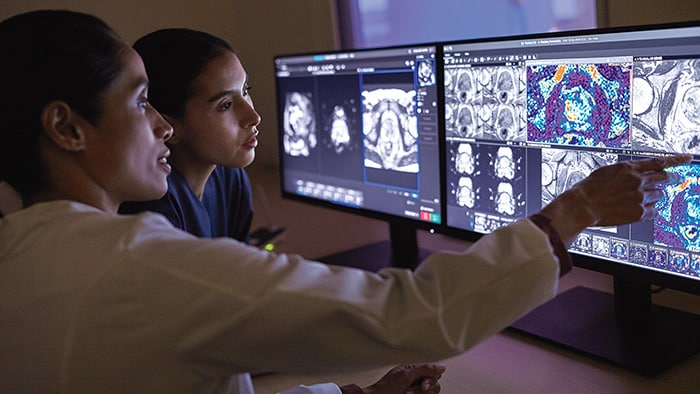
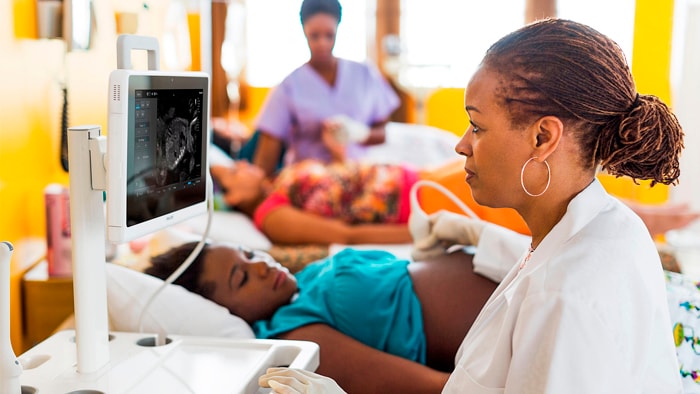
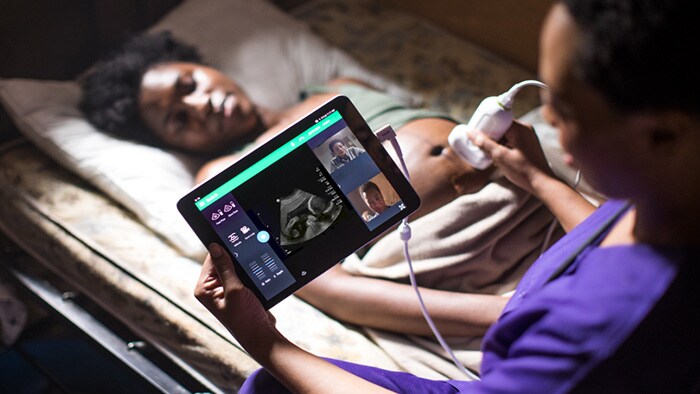
Circular, service-oriented models are central to reducing waste and carbon emissions, and so making healthcare more sustainable. This is why, at Philips, we have started to fundamentally redesign our business models. With the new periodic, usage- and outcome-based business models, we are moving from selling the physical product or system to offering its use as a service. For radiology or oncology departments, for example, it’s no longer about getting a scanner – it’s about getting the right imaging and analytics needed to support precision diagnosis and personalized treatment. And by designing scalable solutions that are easier to implement, install, maintain and use, our customers have access to the high-impact technologies they need – with a much smaller environmental footprint and without the risks and cash impact of big upfront investments in infrastructure and systems. Our Philips Lumify portable ultrasound service is a good example. Under this flexible subscription service, users can have access to transducers, an app and online ecosystem. The subscription service reduces upfront costs and improves patient access to innovative care, for example in remote areas. Models like this have the added benefit of supporting multiple re-use and recycling, thus contributing to the sustainable use of resources.
Digital technology can be a key driver of the transition to resource-efficient value creation.
Robert Metzke
Philips Global Head of Sustainability
Beyond hardware
At the same time, we are working to maximize the lifetime value of our products and systems by extending their technical and economic life – through takeback and refurbishment, and parts recovery. And we are reducing our use of virgin materials by increasing use of recycled materials. But, while many people understandably associate ‘circular’ with closing the loop on hardware like this, it does not tell the whole story. The true promise of circular lies in decoupling value creation/retention from resource consumption. Or to put it in practical terms: How can we deliver a better service or intended outcome, with less drain on material resources? At Philips, we believe that the answer, or at least part of the answer, lies in digitalization. Digital technology can be a key driver of the transition to resource-efficient value creation, tapping an amazing potential that goes way beyond the role of a mere ‘enabler’.
The transformative power of connected digital technology
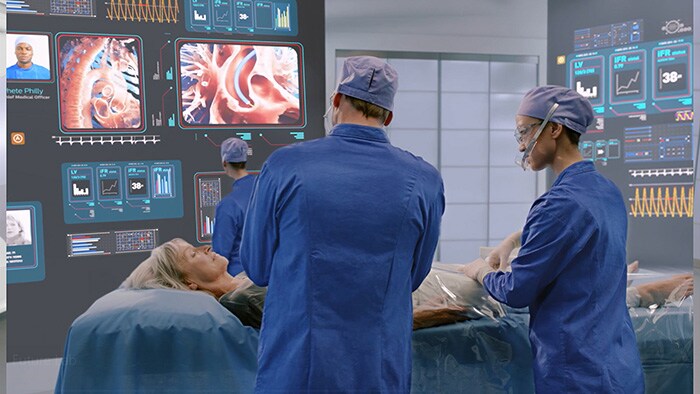
Fueled by the COVID-19 crisis, we are now seeing a massive step-up in adoption of digital technology, as consumers (keen on health living and prevention) and health systems (keen to reduce the stress on capacity) turn to innovative technology to help them address their challenges. In the past few months alone, we have seen a proliferation of triaging apps, amplified sharing of data across healthcare providers, track-and-trace of COVID patients, a sharp increase in telehealth activities such as remote monitoring and video consultations. And the list goes on. Unfortunately, with personal health data currently scattered over many apps, devices and platforms in multiple places and formats, the value of that data for patients, clinicians and caregivers is often still limited. As the most recent Circularity Gap report highlights, the need for global collaboration to collect and share data is one of the main drivers for closing the circularity gap. By integrating and combining data in a meaningful way, we can create smarter, connected health solutions. Applying clinical decision algorithms and predictive analytics, we can use data to deliver personalized, actionable insights. These can then be used, for example, to help motivate healthy behavior through digital coaching, to support healthcare professionals in making clinical decisions, or to alert medical teams to potential problems – all potentially life-changing applications. Of course, If developed with patient needs in mind, digital technologies will have a major role to play in extending access to care, e.g. by enabling many underserved communities to ‘leapfrog’ the gap in provision of primary services.
Digital driving resource efficiency
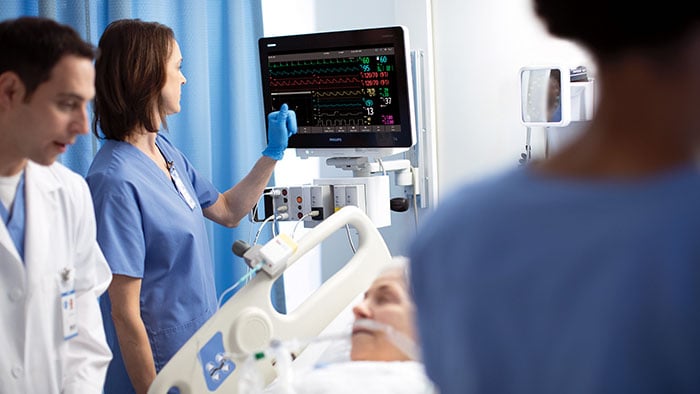
Besides having such a positive direct impact on the delivery of care, digitalization can also enable more efficient use of scarce resources, both human and material. For example, supporting telehealth and the shift of care from resource-intensive clinical settings to networked lower-cost settings and the home. Connectivity and digital infrastructure can have a major effect in reducing our environmental footprint, by enabling ‘dematerialization’ and optimized use of resources. By 2025, it is expected there will be 41.6 billion connected devices, or ‘things’, generating 79.4 zettabytes (ZB) of data. Research[2] indicates that the resource savings unlocked by digital information and communication technology outweigh the increase in the footprint caused by the deployment of that technology. In the area of connectivity, software enables the integration of interfaces to exchange data between different data platforms. In healthcare, this can help prevent multiple diagnoses and reduce IT processing time. It also enables remote interactions between caregivers and patients, and among caregivers. This could potentially reduce the need for physical healthcare facilities, thereby lowering consumption of materials and energy, as well as travel. Last but not least, digital technology enables the use of generic hardware (e.g. tablets) for computation and/or the user interface, which means less need to produce dedicated devices. Here too, our Lumify portable ultrasound service is a case in point. Likewise, in the area of digital infrastructure – with local virtual servers potentially integrated and optimized and stored in the cloud – the resource-efficient role of software should not be underestimated. Software allows us to create virtual resources to manage workloads. This means fewer local servers are needed, and power consumption can be reduced thanks to better CPU utilization. It also enables cloud computing, involving the use of remote internet servers. This is a positive development, as centralized data centers use hardware more efficiently, which means less CPU capacity in use. Indeed, 84% less power is used when customers use large-scale cloud providers instead of on-premises infrastructure[3]. And the increased efficiency enabled by software also extends the lifetime utilization of hardware. Philips PerformanceBridge is one example of how digitalization can support better and more resource-efficient care delivery. This web-based, real-time data platform aggregates data from multiple sources and integrates with the hospital’s image viewer, so that staff get the data they need with context. Operational data is clearly presented, so staff can readily identify outliers and potential improvement opportunities, also when it comes to material/energy usage.
Join us on our journey
While the potential of circular business models and digitalization of care is clear, we can only fulfill that potential by working together with care providers, practitioners, other technology companies, and knowledge partners. I therefore invite you to join the discussion on how to best leverage the trend of digitalization to accelerate the adoption of sustainable practices such as circular economy. Eager to build upon our initial learnings, we would be delighted to hear from parties interested in exploring this further with us. [1] Global Footprint Network (2019) [2] Accenture #SMARTer2030. (2015). ICT Solutions for 21st Century Challenges
Share on social media
Topics
Author

Robert Metzke
Philips Global Head of Sustainability Mr. Metzke leads Philips’ activities in Sustainability where he drives the company’s strategy towards innovative, sustainable business models and embedding sustainable and circular ways of working across Philips. In particular, Robert and his team are leading all activities with regards to Philips' environmental responsibility, with a focus on climate action, circular economy and expanding access to healthcare in underserved communities, as part of Philips overall purpose to improve people's health and well-being. Before joining Philips, Mr. Metzke worked at McKinsey & Company as a consultant where he gained 5 years of experience in strategy and innovation in the high-tech, healthcare and public sectors. Mr. Metzke has a background in journalism, science publishing (Science/ AAAS) and academic research (physics). He is married, has three children and lives in the Netherlands.
Follow me on