Taking healthcare everywhere – three key themes from the 2023 Future Health Index
Apr 19, 2023 | 8 minute read
Amid increasingly strained resources, healthcare systems are forced to rethink how and where they deliver patient care. This year’s Future Health Index – the largest global survey of its kind – shows how healthcare leaders and younger healthcare professionals are aligned in their vision to innovate care delivery models with digital technologies that meet patients where they are.

Fast-tracked by the pandemic, the past three years have given us a glimpse of the future of healthcare delivery: one that extends beyond the hospital into the home and the community, with digital technology connecting care across settings. There is no going back now. Staff shortages and financial pressures compel healthcare organizations to deliver care in smarter and more efficient ways. Patients are also demanding it. Digital transformation continues to accelerate every aspect of our lives, from how we buy to how we work and learn. As a result, our best and most convenient experience anywhere is now what we expect everywhere – including in healthcare.
How can new care delivery models, which integrate in-person and virtual care within and beyond hospital walls, offer a path forward? With this year’s Future Health Index research, we set out to answer that question. Now in its eighth year, the global survey asked healthcare leaders and younger healthcare professionals (aged 40 or under) in 14 countries how they envision the role of new care delivery models. Their answers are revealing, showing remarkable agreement between healthcare leaders of today and tomorrow. Here are three key themes that emerged from the survey findings – which you can read more about in the full Future Health Index 2023 report.
1. Tackling workforce shortages with digital innovation
I hear the same cry for help in every healthcare organization I get to interact with: how can we continue to provide high-quality and timely care when the highly-skilled professionals who are needed to deliver that care are in increasingly short supply?
This year’s Future Health Index shows how more than half of healthcare leaders globally (56%) are either using or planning to use digital health technologies to reduce the impact of workforce shortages. Top of their list are digital health technology solutions that connect with out-of-hospital settings (selected by 43% of healthcare leaders), closely followed by cloud-based technology to support access to information from any location (42%) and critical decision support technology such as AI and predictive analytics (39%)

We are seeing many examples of that in action today. Hub-and-spoke models such as radiology operations command centers and tele-ICUs allow healthcare organizations to extend their expertise, with specialists in a central location offering remote guidance and assistance to their peers in peripheral sites. No longer is specialty care delivery bound to a physical location. Through technology, we can make it available everywhere.
Healthcare leaders recognize that workflow automation and AI are also critical in alleviating the pressure on their workforce constraints. Now that the availability of qualified staff has become a significant rate limiting factor in healthcare, we need to embed expertise into technology to make specialty skills more widely available. Take a complex imaging modality such as MR: selecting the right protocol for an exam takes a significant level of expertise. Smart algorithms can lend a helping hand, by learning from each hospital’s protocol preferences to automatically suggest the most suitable protocol for any given exam and patient anatomy. That’s how we can scale human expertise with machine learning to empower staff.
Younger healthcare professionals welcome the increased investments in digital technologies. In fact, our survey findings show they are asking for it. Being at the forefront of AI in healthcare is their top consideration in choosing where to work (selected by 49% of younger healthcare professionals), followed by being at the forefront of connected care delivery (44%). These responses suggest that digital innovation can also be a powerful tool in attracting and retaining talent as healthcare leaders are increasingly competing with other sectors for scarce professionals.
Interestingly, when asked what would make them feel most empowered to improve patient care, younger healthcare professionals cited, amongst others, better training on new technologies (38%) – illustrating the need for continuous education to help them get the most out of digital innovation. They would also like more opportunities to have their voice heard (39%). This underscores the importance of designing and optimizing ways of working with and not just for staff, as I outlined in my previous post on the cultural aspects of digital transformation.
Yes, digital technology can help relieve the burden on overstretched healthcare professionals – but only if we involve them from the start to ensure it serves their needs and workflows.
2. Bringing healthcare closer to the patient
Last year, the Future Health Index revealed that healthcare leaders viewed extending patient care delivery beyond the hospital as their highest priority, after staff satisfaction and retention. This year, we see that trend continue.
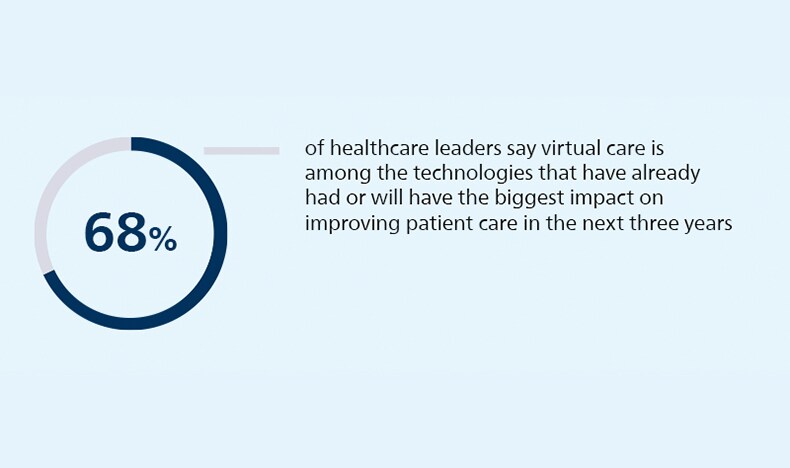
Following its explosive uptake during the pandemic, virtual care is turning into a mainstay of medicine. 68% of healthcare leaders say it is among the technologies that have already had or will have the biggest impact on improving patient care in the next three years. This is reflected in how they are allocating their budgets: 54% of them are investing heavily in virtual care today, up from 47% a year ago.
That’s with good reason. Comprehensive, condition-specific virtual care management is showing compelling results. In recent clinical studies, it has been shown to help ease pressure on hospital staff by reducing emergency department visits up to 38%, as well as lowering the cost of care by as much as USD 3,086 annual claims per patient through better management of chronic disease [1,2] – all while giving patients more control of their own health in the comfort of their home. It’s a win-win-win for healthcare professionals, patients, and payers.
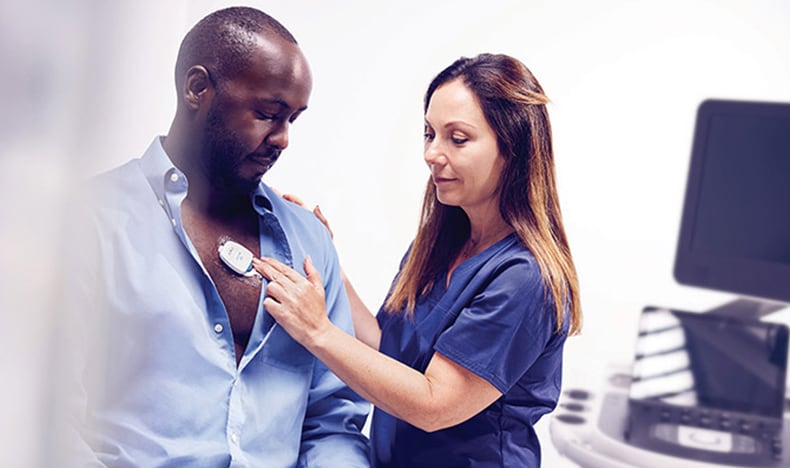
What I am equally excited about is the potential of new digital technologies to support remote diagnostics. For example, with a connected mobile patch worn on a cardiac patient’s chest, physicians can now diagnose and manage heart rhythm disturbances across care settings, from the hospital to the home, based on near-real-time data insights. One study showed how this kind of ‘anytime anywhere’ visibility of a patient’s health can increase detection of atrial fibrillation and generate up to USD 4 million in cost savings [3].
Yet it’s not just virtual care that is helping to bring care closer to patients. When asked more broadly which services healthcare leaders aren’t currently providing but plan to start providing in the next three years, they also called out walk-in centers, surgery centers, and out-of-hospital emergency care (all three cited by 36% of leaders as expansion areas). Younger healthcare professionals also envision a further proliferation of ambulatory and community-based care settings. What we are seeing is a diversification of entry points in healthcare. For patients, that means having greater choice, convenience, and access. Or, as I like to say, we are moving to a future of “your care, your way.”
3. Partnering across the healthcare ecosystem
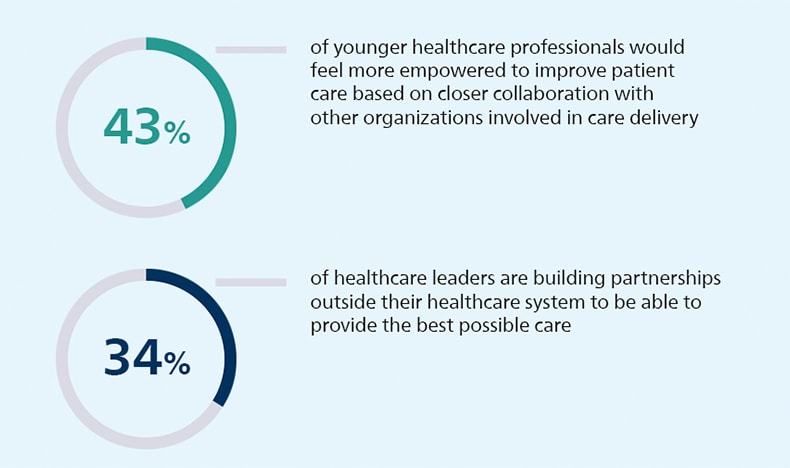
Not only do healthcare leaders and younger healthcare professionals have a similar vision for the future, they both also recognize they can’t get there alone. Even more so than in previous years, partnerships and ecosystem collaboration emerged as a key theme in this year’s Future Health Index research. As payers are pushing for high-quality care delivered in cost-effective ways, more than one-third of healthcare leaders (34%) are building partnerships outside their healthcare system to ensure that new ways of delivering care improve patient outcomes. No longer do they think of their hospital or health system in isolation. Wider ecosystem collaboration is the new norm. Younger healthcare professionals share the same desire to team up with other healthcare organizations. In fact, when asked what would empower them most in improving patient care, closer collaboration with other organizations involved in care delivery was their top choice from the options offered, selected by 43% of them.
That collaboration is taking different forms:
To realize their vision of delivering integrated care across settings, healthcare leaders and younger healthcare professionals realize they need to liberate data and make it available when and where it is needed. That’s why they also see an important role for partnering with health technology companies and data/IT providers. More specifically, when asked which factors will determine the success of new care delivery models, healthcare leaders and younger healthcare professionals were united in calling out interoperability across systems and platforms (28% across both groups combined) and timely and smart data sharing (27%). Or as one CIO recently told me: “When a pilot is flying a plane, all relevant data is gathered for them in one digital display, irrespective of who manufactured the underlying instruments. It should be the same in healthcare.” And he is right: interoperability and data liquidity is what we should be aiming for with all informatics solutions. That’s how we can enable data to flow without friction to generate actionable insights at the point of care. In recent years, healthcare providers have come to recognize the sector’s responsibility in reducing its sizeable carbon footprint. In fact, I am seeing firsthand how it is becoming a key consideration for hospitals in establishing strategic partnerships with companies like Philips. A new eco-conscious generation of talent is also asking for it. More than one-third of younger healthcare professionals (35%) consider it important that a hospital has strong sustainability practices in place. However, our survey findings reveal there are several barriers holding healthcare leaders back in implementing environmental sustainability initiatives – including a lack of clear standards and agreed metrics for measuring success. Again, that is where providers are looking to collaborate with peers and third parties. They also want to share best practices and measure progress against clear targets. Taken together, these findings paint a future where healthcare is delivered in more connected, convenient, and sustainable ways across care settings, enabled by digital technology and collaboration. I invite you to explore the survey findings in more detail and reflect on what they mean for your organization. Where will you take healthcare next? I hope you find inspiration from current and future healthcare leaders in the full Future Health Index 2023 report!
Going forward, clinical, and economic evidence of the benefits of new care delivery models will be essential in driving further adoption by payers and providers. Limited-scope pilots conducted with partners can help generate that evidence, showing how digital innovations can improve patient health outcomes as well as the patient and staff experience. Similarly, being able to measure progress on environmental sustainability goals will help propel green initiatives in healthcare.
Sources [1] Magee MF, Baker KM, Fernandez SJ, et al. Redesigning ambulatory care management for uncontrolled type 2 diabetes: a prospective cohort study of the impact of a Boot Camp model on outcomes. BMJ Open Diabetes Res Care. 2019;7(1):e000731. Published 2019 Nov 13. doi:10.1136/bmjdrc-2019-000731. [2] A Diabetes Care Management Program for uncontrolled type 2 diabetes in a predominantly African American population amortized over the study cohort due to reduced risk of all factors hospitalization after 90 days compared to usual care.
Share this page with your network








