In five years from now, will we look back on the pandemic as the catalyst behind a new era of innovation and collaboration? Will we look at 2020 as the turning point on our path to achieving universal health coverage (UHC)? I believe we will. The opportunity is ours for the taking. But we have to take it – the world is watching. That’s why I want to call on those of us fighting to ensure people everywhere can access the health services they need. We must build on the momentum created by the pandemic and get the message out, beyond our networks, that billions of people have little or no access to health services. We must strengthen partnerships forged in the last year and capture the innovative spirit we’ve once again discovered, so we can get on track to achieving UHC by 2030, with speed. And we must ensure we don’t let things slide back to the way they were before the pandemic. Here’s how we can make a start.
Giving a voice to the crisis
Pre-pandemic, the WHO and the World Bank reported that up to 3.5 billion people – half the world’s population – lacked access to basic health services. While we can’t yet say by how much the pandemic has increased these already shocking numbers, we know it has further strained many communities in both developed and developing nations. For example, while countries have prioritized care for those who have contracted coronavirus and need treatment, pregnant mothers, people living with diabetes, cancer patients, heart disease patients and many others have struggled to access care, further putting the quest for UHC in crisis. That’s why, as we scramble to come out of the pandemic, we need to build health systems that are resilient to future shocks, while also strengthening our commitments to achieving UHC.
There’s no better time than now to make the case for achieving UHC. We can start by calling out the true nature of the challenge we’re up against.
We believe digital and technological innovation along the health continuum is key to expanding access to care and achieving UHC. In fact, I am convinced UHC can only be achieved through digital innovation.
Jan-Willem Scheijgrond
Global Head of Government and Public Affairs, Philips
Sharing the commitments we make
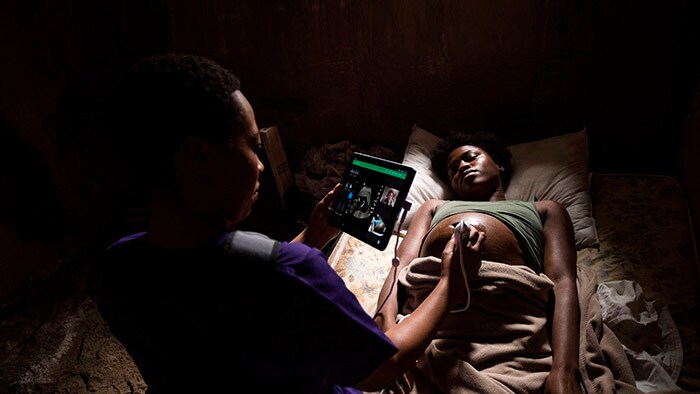
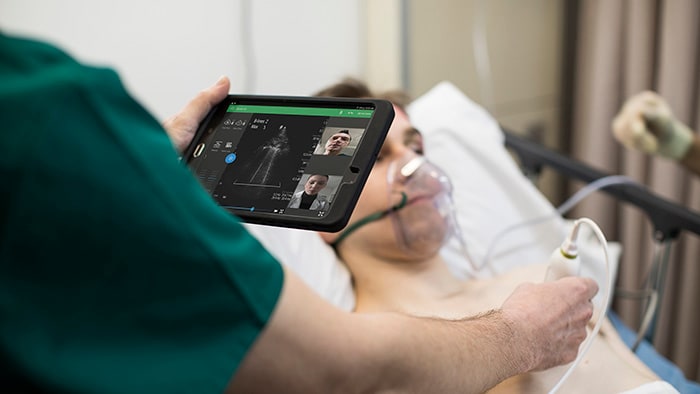
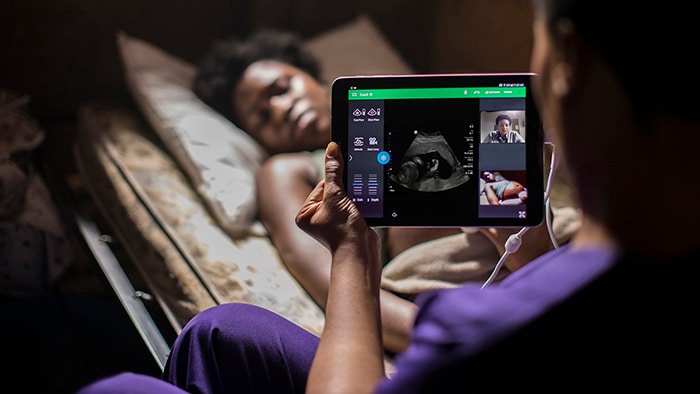
Next, we need to talk about these commitments, sharing how we are all working to expand access to care for all, no matter the size or scale of these commitments. At Philips, we aim to improve the lives of 2.5 billion people a year by 2030, including 400 million in underserved communities. To help expand access to care for these underserved communities, we have committed to driving digital and technological innovation along the health continuum, developing new business models and financing solutions, and building strong partnerships within an ecosystem of collaboration. Driving digital and technological innovation along the health continuum We believe digital and technological innovation along the health continuum is key to expanding access to care and achieving UHC. In fact, I am convinced UHC can only be achieved through digital innovation. One example of this is our eICU program, a transformational critical care tele-ICU program. It enables a co-located team of intensivists and critical-care nurses to remotely monitor patients in the ICU regardless of patient location. Intensivists and nurses based in a telehealth eICU hub are supported by high-definition cameras, telemetry, predictive analytics, data visualization and advanced reporting capabilities in order to support their colleagues on the front line. Such solutions enable more patients to receive high-quality care, closer to home, even in remote locations. Developing new business models and financing solutions For locally relevant innovations to take off and scale, we recognize the need for new business models that bring together donors and impact investors, governments, NGOs and the private sector. For example, Philips has joined forces with Makueni County government, Amref Health Africa and the Dutch development bank FMO in the Partnership for Primary Care Makueni. Kicking off in July 2018 with a one-year feasibility study in Makueni County, the aim of the partnership is to strengthen primary care by building a financially sustainable model that improves access to high-quality care. The project has improved care delivery significantly. The partnership is now developing a public-private partnership that can be financially sustainable thanks to a delicate balance between capital investments, capitation fees, insurance payments, technical assistance grants and performance-related payments.

Building strong partnerships within an ecosystem of collaboration Lastly, we believe that a committed ecosystem of strong collaborators is key to addressing the complex challenges in expanding access to care. That’s why we’re helping to, among other things, build the Digital Connected Care Coalition (DCCC). Co-initiated by Dalberg, PharmAccess Group and Philips, with 20-plus members, the DCCC was created at the end of 2019 to accelerate the digital transformation of healthcare and support the journey towards achieving universal health coverage across low- and middle-income countries (LMICs). To adequately address the complex nature of healthcare transformation, the DCCC brings together a comprehensive and cross-disciplinary membership base that forms a networking-and-action platform to support more efficient partnerships across sectors and reduce fragmentation. It anchors its design in the WHO principles for digital health and the WHO/ITU framework for e-health. These are just some of the ways we at Philips have committed to fighting for UHC. By sharing these stories, I hope I inspire you to continue sharing what you’re doing – the commitments, the results, the experiences, good and bad.
Taking the opportunity before us
For more on how I feel about what makes for successful partnerships on the path to UHC, read my last blog post.
Let’s continue to give a voice to the challenge of our lives, for all lives, building on this newfound momentum we have, on our innovative spirit, and on the strong partnerships we’ve forged. And let’s visualize what UHC could look like, especially for those who can’t imagine it. Only then can we hope to have made that massive step forward in five years’ time, on the road to UHC for all in 2030!
Share on social media
Topics
Author

Jan-Willem Scheijgrond
Global Head of Government and Public Affairs Jan-Willem leads the global network of government and public affairs professionals at Philips. He heads up partnerships with international partners such as the United Nations and the World Health Organization.
Follow me on