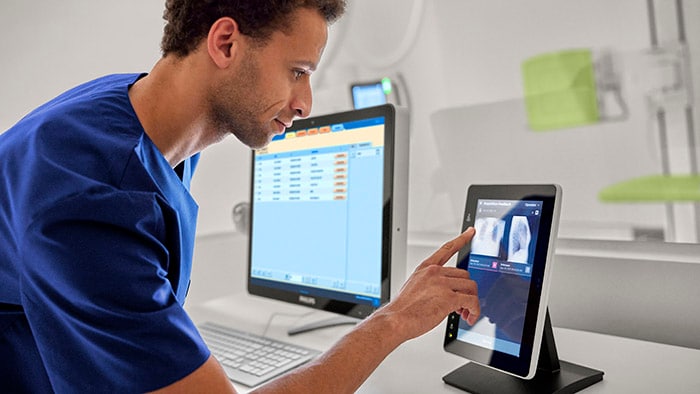
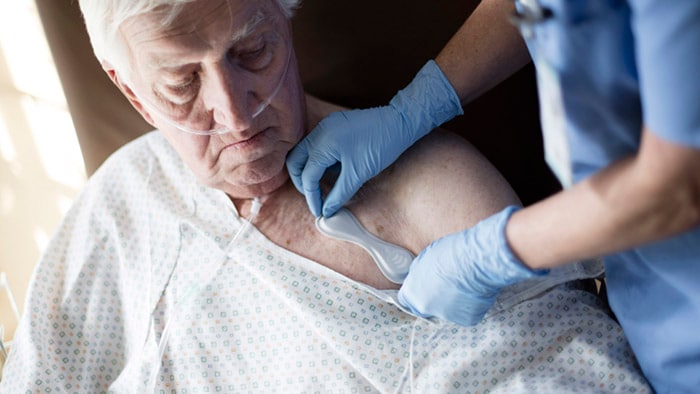
At Philips, we’ve long championed a commitment to oral-systemic health, education and innovation. As such, I was pleased to see the resolution centered around oral healthcare approved at the WHO’s World Health Assembly last month, which was based on the theme: Ending this pandemic, preventing the next: building together a healthier, safer and fairer world. After years of research into the connection between oral and overall health, the WHO elevated the conversation to a global level, proposing a much-needed reorientation of oral healthcare to bridge the gap between dentistry and medicine [1].
Access to prevention, early diagnosis and treatment of oral diseases are far from universal and sadly remains unattainable for millions. As we build our next normal together, this resolution has huge potential to address the vast disparities in oral healthcare around the world and, ultimately, help vulnerable populations to thrive.
Many dental practitioners describe the mouth as ‘the gateway to the body’ because it offers clues about our overall health, with strong links tying oral diseases to other health problems. From diabetes and heart conditions to Alzheimer’s and neo-natal health, it’s now widely acknowledged that oral healthcare is an important aspect of disease prevention [2][3][4]. It’s great to see this confirmed with official support from the WHO for a more holistic approach to healthcare.
Within the resolution, the WHO underscores the importance of good oral health to overall health and well-being and prompts member states to accelerate action on oral health to promote disease prevention. With 3.5 billion people suffering from oral diseases worldwide, there’s an urgent need to better integrate oral health into national policies to ensure more timely and inclusive care [5]. This is such an exciting step forward, moving away from the traditional curative approach and puts our society more firmly on the path to prioritizing preventative care.
Harnessing technology to promote preventative care
Good oral care goes beyond keeping your mouth healthy, as gum disease has been linked to neo-natal and adverse pregnancy outcomes [6]. In West Virginia, U.S., we help expectant and new mothers adopt good oral care habits by supporting the Helping Appalachian Parents and Infants (HAPI) Project. The results speak for themselves: women in the perinatal care program who reported brushing twice daily with a Philips Sonicare toothbrush had improved birth outcomes than those who brushed less than twice a day [7].
With patients missing dental appointments during stay-at-home periods this past year, the pandemic highlighted the value of consistent home oral hygiene routines. The increasing use of AI-enabled, personal devices can help people adopt healthier brushing behaviors. For example, our newest power toothbrush, the Philips Sonicare 9900 Prestige, is accompanied with an AI-powered smartphone app, which gives real-time guidance and personalized recommendations to improve users brushing habits. While AI and connected devices are not new to consumer tech, the health tech industry has more recently started to embrace this trend. With greater adoption of this technology in our health devices, we can empower people with their health data and build a greater understanding of what that data means for their long-term wellness. By equipping people with these insights, they’re able to make lifestyle changes with long-lasting health benefits.
We’re at a pivotal point in medical knowledge, technology and data science innovation over the past year, advancing consumer care in a truly impactful way. It’s now our shared responsibility to bridge the gap between oral and systemic health and help bring medical and dental professionals together so they can deliver more effective care.
Deeptha Khanna
Chief Business Leader Personal Health
Oral healthcare shouldn’t be an afterthought
We’re at a pivotal point in medical knowledge, technology and data science innovation over the past year, advancing consumer care in a truly impactful way. It’s now our shared responsibility to bridge the gap between oral and systemic health and help bring medical and dental professionals together so they can deliver more effective care.
Due to the pandemic, we’ve seen teledentistry play an increasing role in connecting people directly with their dental professionals. Of course, we know that digital health is not a replacement for essential in-person appointments, but greater adoption (and health insurance coverage) of teledentistry and remote monitoring is a key step in expanding access to care and improving long-term health outcomes.
There’s also work to be done in the payer/provider ecosystem. We still treat care of the mouth differently compared to other types of medical care. For example, why is oral healthcare in many countries an add-on package to health insurance, rather than part of the overall coverage? Good dental care is part of good medical care and oral health coverage should be more of a priority on national healthcare agendas and less of an afterthought.
We know that many dentists take blood pressure and other vital readings at regular check-ups, but this data is generally not linked to the systems of general practitioners. With visits twice a year, many people have a closer relationship with their dentist than their doctor – and this makes dental professionals well-positioned to detect systemic health conditions earlier.
Today, we have a tremendous opportunity to forge closer connections between dental professionals and the rest of the healthcare system. What if people could share their dental and health records with healthcare and oral care professionals via the same data ecosystem? A patient could be supported by their doctor and their dentist in the management of their diabetes. And this collaboration would benefit more than just dentist and GPs. By including care providers across the entire health continuum from prevention to healthy living, we could promote better overall patient outcomes as a result.
To bring to life the recommendations from the WHO’s resolution, there’s work to be done to fully integrate oral care into universal health. Digital and technological innovation is a major factor in this, and we at Philips are fully committed to driving this forward to shape the future of healthcare.
[1] World Health Organization (2021, January) Oral Health EB148.R1
https://apps.who.int/gb/ebwha/pdf_files/EB148/B148_R1-en.pdf
[2] Effects of periodontal disease on glycemic control, complications, and incidence of diabetes mellitus (2020, May) https://onlinelibrary.wiley.com/doi/abs/10.1111/prd.12271
[3] Periodontitis and cardiovascular diseases: Consensus report (2020, February) https://onlinelibrary.wiley.com/doi/full/10.1111/jcpe.13189
[4] Periodontal diseases and adverse pregnancy outcomes (2018, August)
https://obgyn.onlinelibrary.wiley.com/doi/abs/10.1111/jog.13782
[5] Global, regional, and national incidence, prevalence, and years lived with disability for 354 diseases and injuries for 195 countries and territories, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017 (2018, November)
https://pubmed.ncbi.nlm.nih.gov/30496104/
[6] Periodontal disease and adverse pregnancy outcomes (2020, May)
https://onlinelibrary.wiley.com/doi/abs/10.1111/prd.12294
[7] Personal Oral Infection Control, Low Birthweight, and Preterm Births in Appalachia West Virginia: A Cross-Sectional Study (2018, August)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6106793
Share on social media
Topics
Author
Deeptha Khanna
Chief Business Leader Personal Health Deeptha Khanna is Executive Vice President and Chief Business Leader Personal Health, and a member of the Royal Philips Executive Committee. The Personal Health businesses of Oral Healthcare, Mother and Child Care and Personal Care (Male Grooming and Beauty) play an important role in the health continuum delivering integrated, connected and personalized solutions that support healthier lifestyles and those living with chronic disease.
Follow me on