Whenever you read about the Internet of Things (IoT), the focus is usually on the ‘things’ that are being connected. A home thermostat that you can control remotely via a smartphone app. Cars that exchange data for real-time traffic regulation. Robots that navigate through fulfillment warehouses to pick up the product you just ordered online. Connected technologies with built-in sensors and smart algorithms are making life easier, safer, and more convenient. And we are just in the early days of the IoT. Gartner projects that the IoT will expand from 14 billion things today to 25 billion things by 2021 – with 5G and AI enabling ultra-fast and intelligent connectivity.
Whenever you read about the Internet of Things, the focus is usually on the ‘things’ that are being connected. But in healthcare, the focus should really be on people, not things.
Yet for all its potential, the term ‘Internet of Things’ is also a bit of a misnomer. By putting the emphasis squarely on technology, the term doesn’t capture what a connected future is really about – which is to serve people. Ultimately, the adoption and impact of any IoT-enabled solution depends on how well it meets and adapts to human needs and aspirations. Nowhere is this more important than in healthcare. The IoT is set to transform how healthcare providers operate and how people manage their health. By intelligently integrating data from different systems and devices, in and outside the hospital, the IoT can give a much more complete, dynamic, and actionable overview of people’s health than what is available today. Both patients and healthcare providers will benefit. But for the IoT to deliver on this promise, I will argue that we must take a thoroughly human-centric approach – with people being the focus rather than things. As we will see, the strength of this approach is already visible from first examples today.

Through a network of connected devices that collect, exchange and analyze data, the Internet of Things can help people take control of their own health, and make healthcare more integrated, personalized, and effective.
Connecting care across settings
Why is the IoT such a transformative concept? Patients have always interacted with a multitude of medical ‘things’ throughout their health journey; from a stethoscope to a blood pressure monitor, from an insulin pump to a CT scanner. Yet traditionally, what was lacking was the means to easily connect the data from all these disparate sources across settings and over time – resulting in disjointed, episodic, and largely reactive care. That is all changing now – with the IoT serving as the connective tissue. Medical devices are getting smaller, smarter, and more portable, with ubiquitous connectivity enabling real-time data exchange. Wearable biosensors allow for more continuous health monitoring, safeguarding the transition between acute and post-acute care. And with home monitoring systems and portable health devices, healthcare no longer needs to be confined to the hospital or the doctor’s office – people can take an active part in it alongside professionals.
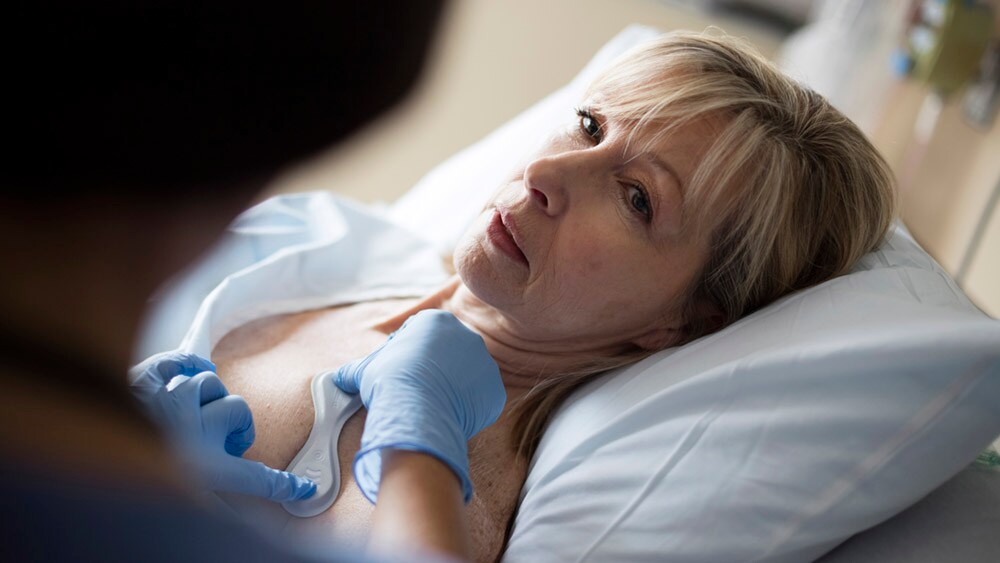
Wearable biosensors allow for more continuous health monitoring between spot checks, irrespective of patient location.
However, merely hoarding individual health data from every possible source will do little to support patients or healthcare professionals. In fact, it would merely add to the information overload that healthcare professionals are already facing today. Worse yet: it could leave patients with many unanswered questions and unnecessary worries about their health. As we move into the future, I believe it is critical we learn from the shortcomings of Electronic Medical Records (EMRs). While they have value, EMRs have always been more about recording data and supporting billing, rather than engaging and guiding healthcare professionals with actionable insights, or facilitating an informed dialogue between patient and care provider. As one doctor lamented in the Scientific American: “we physicians entered the profession to connect with and help patients – not to stare at a screen”. We also need to be mindful that, in the consumer domain, not all fitness and health trackers have proved sticky enough for sustained use. Abandonment rates of up to 30% have been reported. Clearly, connecting ‘things’ for continuous data collection is not a panacea in itself.
Technology should support the relationship between a patient and a healthcare professional, rather than get in their way.
That is why it is so important to put patients and healthcare professionals at the center of the IoT. Technology should support their relationship rather than get in the way. Data needs to be analyzed and presented in a way that filters the signal from the noise, helping people to act on the information that matters, based on an understanding of what they are trying to achieve in a certain context. This can be achieved by taking what I call a systems of engagement approach. A system of engagement aggregates data from disparate sources and moments in time, and gleans relevant insights from them based on AI or advanced data analytics combined with available medical knowledge. These insights are then presented to people in a personalized and contextualized way, via easy-to-use and intuitive apps. Let’s now consider what this looks like in practice, by turning our attention to one of the world’s most prevalent chronic diseases.
Helping patients adhere to their therapy
Nearly one billion people worldwide suffer from obstructive sleep apnea (OSA), a chronic disorder that causes their breathing to repeatedly stop and start during sleep. OSA can be treated through therapy known as Continuous Positive Airway Pressure (CPAP). A CPAP system uses a mask to send a constant flow of airway pressure to the throat to keep the airway open during sleep. To be maximally effective, the CPAP system must be used every night. As with many chronic diseases, however, therapy adherence is low. At Philips we have developed an ecosystem of connected solutions to support both patients and healthcare professionals in managing this debilitating condition. Patients can wirelessly connect their CPAP system to an app called DreamMapper, which provides personalized therapy guidance. The app analyzes therapy use, mask fit, and apnea hypopnea index (AHI) readings (the number of pauses in breathing per hour of sleep) to help users set and achieve personal goals.

Patients with obstructive sleep apnea can monitor their therapy and get personalized advice via a mobile app when needed.
For example, if the patient starts to struggle with therapy adherence by dropping below two hours of use each day for several days, then the app will attempt to work out why by asking questions. Depending on the patient’s answers, the app will give tailored advice. This could be something simple such as, “we notice you’re having issues with mask fit”, together with a suggestion to watch a video on how to fit the mask correctly. At the same time, professional sleep therapists are able to access their patient data remotely through a cloud-based platform. Automated alerts help them direct their attention toward the patients who most need their attention at any given moment. One study demonstrated that 58% more people stuck to their therapy every night when they used the app [1]. The study also showed a 283% higher success rate for users struggling with adherence to sleep therapy [2].
Connecting smart devices, mobile apps, and clinical data can help people take control over their own health – while providing healthcare professionals with actionable insights that allow them to provide support when needed.
These results illustrate how connecting smart devices, mobile apps, and clinical data can help people take control over their own health – while providing healthcare professionals with actionable insights that allow them to provide support when needed. Enabled by secure, cloud-based connectivity, with appropriate privacy controls. It captures the essence of what the IoT in healthcare is about. But this is merely one of many examples of how the IoT can support patients and healthcare providers alike. In my next article, I will explore a wider range of IoT applications that are changing the face of healthcare. All by putting people – not things – first. References [1] 19% of DreamMapper users used their therapy 100% of the nights over 90-days versus 12% for the Standard Care users, a relative increase of 58.33%. In a retrospective review conducted by Philips Respironics of the EncoreAnywhere database (white paper) that compared DreamMapper patients (n=71,157) to users who did not use it (n=56,711) over a period of 90 days. [2] 46% of DreamMapper patients went on to achieve adequate adherence within 90 days versus 12% for the Standard Care group, a relative increase of 283.33%. In a retrospective review conducted by Philips Respironics of the EncoreAnywhere database (white paper) of struggling patients (n=24,176)
Share on social media
Topics
Author

Henk van Houten
Former Chief Technology Officer at Royal Philips from 2016 to 2022













