Show me the evidence: how real-world data is advancing image-guided therapy and patient health outcomes
Mar 23, 2023 | 5 minute read
Image-guided therapies have driven a quiet revolution in healthcare. Patients can now be treated with ever more precision in minimally invasive ways, which typically result in faster recovery and improved health outcomes. But for innovations in image-guided therapy to be adopted more widely in clinical practice, they need a strong data-driven evidence base. This is where the use of real-world data is increasingly complementing traditional clinical trials to advance new, evidence-based interventional treatments.
Evidence-based medicine has always been the cornerstone of good clinical practice. And with the continued rise of value-based care, it is only becoming more important. That’s because reimbursement is now increasingly being tied to appropriate use criteria for interventional treatments as well as patient outcomes. Fortunately, in the age of big data, we have access to more information than ever before to evaluate the effectiveness of new treatments. That means patients get to benefit from faster adoption of potentially life-saving innovations that have shown to be effective in real-world application.
Complementing randomized controlled trials with real-world data
Historically, randomized controlled trials have been the gold standard for assessing the safety and efficacy of new health technologies, generating robust evidence in a highly controlled fashion. While such trials will continue to play a critical role in our efforts to innovate procedures in image-guided therapy, a common question on the mind of payors, physicians, and regulatory reviewers is to what extent the results of these protocol-driven trials generalize to real-world application.
To help answer that question, we can now tap into a wealth of real-world data collected in routine clinical practice. This includes data sources such as electronic medical records, disease registries, insurance claims, as well as patient-generated data generated through wearables.
With the use of this real-world data, we are able to evaluate the safety and effectiveness of technologies much more quickly and in a much larger number of patients – providing valuable insights that would have taken many more years to collect if we had to rely on clinical trials alone.
Shortening the path to evidence
During the COVID-19 pandemic, we have all witnessed the importance of speed in clinical development. Global randomized controlled trials, complemented with early analysis of real-world data, propelled the application of medical advances in drug and vaccine development, often in record time.
Some of the same lessons can now be applied to the development and authorization of medical devices. In fact, regulatory bodies have already shown commitment to incorporating real-world evidence in its evaluation of medical devices.
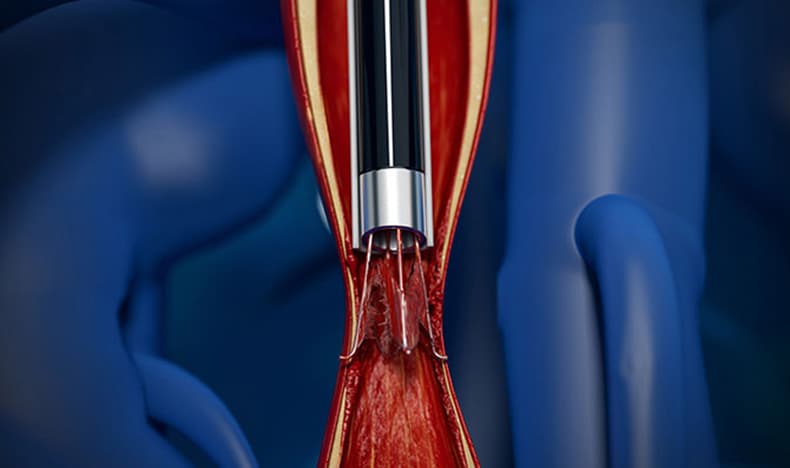
For example, late 2021, Philips received market authorization for its CavaClear laser-based device, using real-world evidence to demonstrate safety and effectiveness of the device in clinical practice [1]. The device can support the removal of indwelling inferior vena cava (IVC) filters in patients who otherwise would have limited options.
Driving adoption in clinical practice
Following market introduction of new technologies, I also see a vital role for real-world evidence to help shape practice guidelines by professional medical societies and reimbursement policies from payers.
A case in point is the use of intravascular ultrasound (IVUS), which allows physicians to visualize the inside of vessels to determine what is restricting blood flow in the vessels supplying the heart (in coronary interventions) or to the legs (in peripheral interventions). IVUS is an imaging technology that has been studied extensively in coronary applications, where it continues to demonstrate improved patient outcomes [2]. However, in peripheral interventions, lack of clarity on the appropriate use of IVUS and lack of patient outcome data has led to inconsistent adoption and yearly reimbursement cuts in the US.
That could very well change based on the latest real-world evidence and expert consensus for non-coronary use of IVUS. In the largest-ever real-world analysis of lower-extremity peripheral vascular interventions, using data from over 700,000 patients, a study conducted by the Smith Center for Outcomes Research showed a 32% associated reduction in major adverse limb events, such as amputations [3]. What’s more, an international team of over 40 clinical experts led by Dr. Eric Secemsky, MD, established the first-ever global, cross-specialty expert consensus on the appropriate use of IVUS in peripheral vascular interventions [4].
Having such compelling clinical evidence and expert endorsement for the use of IVUS in peripheral vascular interventions promises to establish a new standard of care, which could improve health outcomes for patients worldwide and drive reimbursement for physicians to promote wider adoption.
At this year’s Annual Scientific Session & Expo of the American College of Cardiology/World Congress of Cardiology, we saw further examples of how high-quality real-world evidence studies can help demonstrate improved patient outcomes from innovations in image-guided therapy.
Accelerating the pace of evidence generation
As healthcare increasingly extends from the hospital to the home, we will only see more opportunities for evidence generation based on real-world data. With the rise of wearable health technology, clinical studies have already begun to include patient-generated data, for example to accelerate the diagnosis of atrial fibrillation based on continuous ECG monitoring. Large-scale data can now be collected in a matter of weeks, speeding up the pace of evidence-based innovation.
Wearables also enable home-based patient monitoring following treatment, generating additional data over time. Coupled with advances in analytical capabilities such as AI, this will offer interventional physicians a richer long-term understanding of the effectiveness of their interventions, helping them decide on the most appropriate treatments for their patients. All in a highly evidence-based way.
Another potential benefit of the use of real-world data is that it could generate insights that are more representative of the population at large, compared to clinical trials in a subset of the population. Lack of diversity and inclusion has been a common concern with clinical trials. Expanding our analyses to broader and more diverse data sets could go a long way toward promoting equitable care for all.
Overcoming challenges together
To unlock these opportunities, there are still several challenges we need to overcome as a sector.
First, further harmonization in regulation around data access and data privacy will be critical to scale the use of real-world data in an effective and responsible way. With AI offering unprecedented opportunities to analyze large amounts of data retrospectively, it is particularly important that we safeguard individual patient privacy while at the same time enabling innovation for the common good.
Second, through our work on IVUS, we have learned the value of close collaboration between different stakeholders – including physicians, medical societies, payors, and health technology providers such as Philips. In partnership, we can identify where more real-world clinical evidence is needed, and how we can generate it in ways that meet the high standards of medical research and professional societies. No stakeholder can go at it alone. Our recently signed five-year partnership with the Smith Center for Outcomes Research is a testament to this belief. It will make full use of the CMS Virtual Research Data Center program to generate high-quality real-world evidence for emerging interventional treatments.
Together, we can continue to advance evidence-based practices in image-guided therapy to innovate interventional procedures and raise the standard of care for patients worldwide.
Sources [2] Hong S, Zhang J, Mintz G, et al. Improved 3-Year Cardiac Survival After IVUS–Guided Long DES Implantation. J Am Coll Cardiol Intv. 2022 Jan, 15 (2) 208–216.
Share this page with your network