Let me tell you about a patient of mine from my days as a pediatrician. Let’s call her Sophia. Her journey was typical of pediatric patients that have been dealt a bad hand and live with chronic or severe diseases. It was also typical in that care for patients like her can be dramatically improved today through value-based care in pediatrics. At an early age, Sophia was diagnosed with cystic fibrosis, a condition that she will have to manage for her entire life. I saw her pinball from one medical silo to the next – from primary care to specialist, to another specialist to yet another specialist. Because she was too young to drive, her family had to bring her to each appointment. Because she did not understand what was happening, she cried through medical procedures that were designed for emotionally mature adults. Back and forth she went, from home to hospital, year after year. She managed to deal with her chronic and non-curable disease throughout childhood, but the experience was stressful, time-consuming, and costly for her and her family. Her care chipped away at the childhood that every child deserves, chronically ill or not. This kind of experience is taxing for the entire family. Author Jacquelien Noordhoek vividly describes this struggle in her book, “Life with Lucas: A Child Growing up with CF,” about her son’s battle with the disease. Jacquelien has been an inspiring role model for me ever since I met her more than 15 years ago, and she still is today through her work as CEO of the Dutch Cystic Fibrosis Foundation (NCFS) and President of CF Europe, a federation of national Cystic Fibrosis associations.
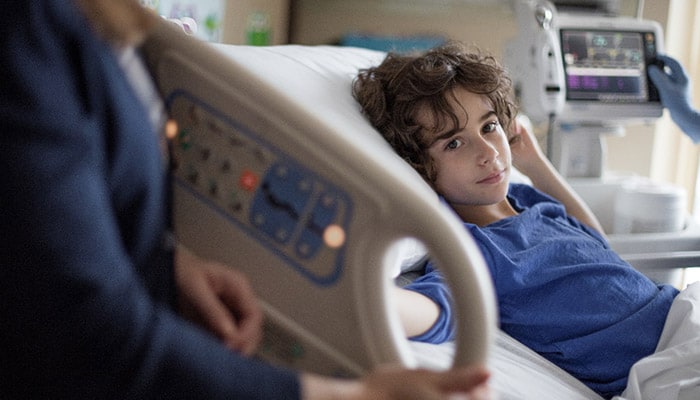
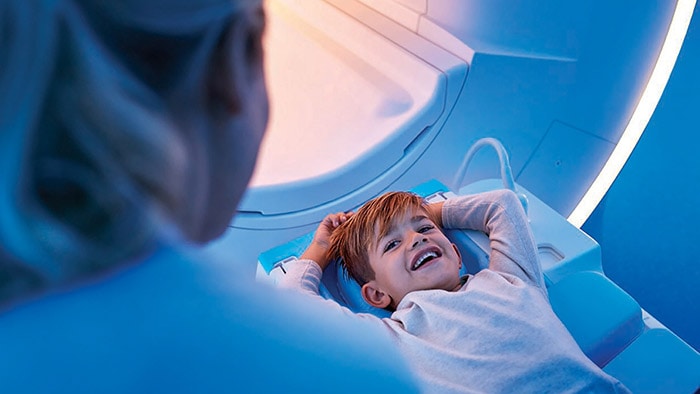
After decades of practicing pediatric medicine, I know there’s a better way to serve young patients like Sophia. It’s called value-based care, and if you’re reading this blog then there’s a good chance you are already familiar with this term. You’ve probably also heard arguments about why it won’t work in pediatric care. But I’m here to tell you that it will: I saw this work first-hand when I was leading a pediatric department more than 10 years ago, and I’ll outline what I believe to be an important step to achieve it. At Philips, we believe in value-based care as a delivery framework to improve health outcomes at lower cost. It focuses on what stakeholders in the healthcare system—patients, healthcare staff, care providers and others—value, and then allocates resources according to the health outcomes delivered by the system. We make value-based care principles actionable by translating value-based care into the Quadruple Aim – better health outcomes, improved patient experience, improved staff experience, and lower cost of care. Achieving any one of these in pediatrics depends on essential building blocks, such as clearly defined outcomes and measurement standards, in combination with digital, connected solutions that build on health informatics and artificial intelligence. Critics of value-based care in pediatrics say that the patient population is just too small, the health conditions too chronic or severe, the spectrum of diseases too broad and the current protocols too entrenched. Why bother with a new model? The reason is simple; for your children, my children, everyone’s children —that’s why. We must restructure care to focus on what’s best for the long-term benefit of children because they still have their entire lives ahead of them. By breaking down silos in care, focusing on outcomes, and transforming reimbursement models, we can achieve the Quadruple Aim of value-based care. Let me paint a picture of what value-based care could have looked like for Sophia. From the time of Sophia’s diagnosis, a team of caregivers—from primary care to disease specialists—works together as a unit to provide care over the long term. Instead of operating as many separate doctors who are paid a fee for each service, the team is reimbursed based on performance and outcomes over a longer period of time. Digital connected care technology allows pediatricians to work together as a fully integrated team. They can share information and work together to address and coordinate care, which improves the patient’s experience and saves money at the same time. Sophia is now able to use telehealth solutions to connect her, her family and her caregivers for online consultations and care coordination. This dramatically reduces the number of trips to the hospital and the time burden associated with that travel. What do you think Sophia would prefer? Sitting in hospital waiting rooms or playing tag out on the street with her friends? Doctors can monitor Sophia’s treatment outcomes remotely, and, in some cases, even provide additional treatment in the comfort of her home. By using dedicated, intelligent software on their smartphones, Sophia’s family can stay informed about her day-to-day health. Such an ecosystem of connected care solutions helps us to achieve the Quadruple Aim—it creates a better experience for both the patient and healthcare providers, and saves money over the long term. But it’s not about using technology for its own sake—it’s about using technology to improve outcomes and the experience of the patient, their families and all other stakeholders in the health system, including payers, providers, and insurers, at lower cost. In other words, complete health systems working together to achieve the Quadruple Aim. I cannot say this too often: children are not simply small adults—they think and behave in a different way, have different emotional needs, and therefore require a totally different care approach than adults, with medical procedures tailored to their specific needs. An example I truly love is our Ambient Experience solution that uses unique sounds and visuals to help children relax during an imaging procedure, reducing the expense associated with the need for repeated scans.

Once Sophia turns 16, 18 or 21 (depending on the system), she transfers seamlessly to adult care due to improved data transfer practices. The transfer is based on smart analytics from data repositories such as the Electronic Health Record, but also from personal devices for continuous or semi-continuous monitoring, pharmacy records, laboratory data, family practitioner notes and other sources. Although all of these exist today, they are not interoperable, not based on outcome measurements, and certainly not built into a longitudinal health record, which would empower Sophia and her parents to participate actively in the day-to-day care. It would also allow them to be much better informed when the time comes to make difficult decisions with her care team, such as choosing the best moment for invasive therapies, such as a lung transplant. It’s also important to note that pooling data (with the consent of patients) from multiple patients with cystic fibrosis would make it possible for artificial intelligence to work towards real personalized therapy, including selection of the patients who will benefit from experimental or expensive drugs. Through all these steps, you’ll notice that it’s the child and his or her family whose well-being is the highest priority. That’s the real drive for value-based care in pediatrics, and the first step on this journey is simple: do whatever you must to put children first. Living as a child with a chronic or severe medical condition is hard enough. It’s long overdue that we implement value-based care in pediatrics so that these children and their families have an easier time getting the care they deserve, with as little disturbance to their day to day lives as possible.
Share on social media
Topics
Author

Jan Kimpen
Chief Medical Officer, Royal Philips Before joining Philips in 2016, Jan Kimpen, Professor of Pediatrics, was CEO of the University Medical Center in Utrecht. He leads the global clinical team of Philips, focusing on advocacy, customer partnerships, clinical research and medical consulting, and is responsible for the annual publication of the Philips Future Health Index. He is a strategic advisor for commercial and clinical strategy, market reimbursement, R&D roadmaps and partnerships and M&A, and provides thought leadership on relevant clinical and medical topics. Jan participates in the WEF Global Future Council on Healthcare, the American Heart Association alliance and the Board of Sanara Ventures in Israel. Jan is president of COCIR, the European trade union for imaging, healthcare informatics and radiotherapy.
Follow me on