As the coronavirus disease (COVID-19) continues to spread, we have made this a top priority for all of us at Philips. Our global resources have been mobilized to continue to fulfill the critical and increased customer needs of healthcare providers and the patients they are taking care of, while ensuring the health and safety of our employees and ensuring business continuity. Employees around the world are stepping up to support healthcare providers and their patients with our broad portfolio of products, services and solutions that can help address the preparedness, response and recovery needs of an infectious respiratory disease such as COVID-19. In addition to diagnostic imaging systems and services and telehealth solutions, the impact of our respiratory care solutions in supporting health systems and care providers is critical in the current situation. For a broader view of what Philips is doing holistically to aid during this pandemic, our CEO Frans Van Houten recently shared his perspective on our key areas of focus. The COVID-19 pandemic is a challenging situation where healthcare workers must not only determine the best course of treatment, but also ensure that the virus is not being spread. There are a range of clinical solutions available for managing patients in respiratory failure, and one way we are supporting providers during this crisis is by trying to optimize the non-invasive ventilation (NIV) therapy. We have outlined some recommendations below, in the hope that these could be of help for anyone treating COVID-19 patients. These recommendations are not meant to replace existing World Health Organization (WHO), national guidelines or established hospital protocols, and of course, decisions regarding any specific treatment must be made by the healthcare provider and the patient based on specific clinical conditions and available resources.
Key Considerations When Using NIV Therapy for COVID-19 Patients
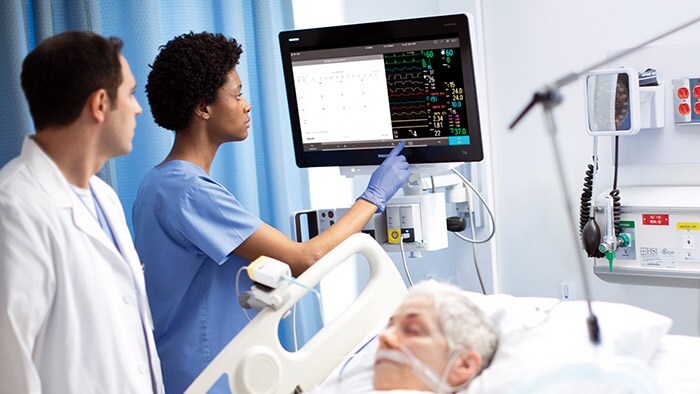
Non-invasive ventilation (NIV) therapy provides both oxygenation and ventilation support and can enable providers to tailor ventilation pressures and flows to match the patient’s breathing patterns. For healthcare providers considering NIV therapy for their COVID-19 patients, it is important to follow the general principles for managing acute hypoxemic respiratory failure when using this therapy. While NIV won’t be an option for every patient with COVID-19 depending on the severity of their symptoms, it has the potential to help many patients in respiratory distress, while ensuring that invasive ventilation options are available for the critically ill. Just as important, COVID-19 is extremely contagious and is being transmitted quickly. It’s vitally important to adhere to infection control measures as outlined by hospital or health department policies to avoid transmission of COVID-19 during therapy. Recommendations from the WHO and the Centers for Disease Control and Prevention (CDC) include using negative pressure isolation rooms for patients, and gloves, gowns and masks for caregivers [1-2].
Adapting Care & Precautions for Different Therapies
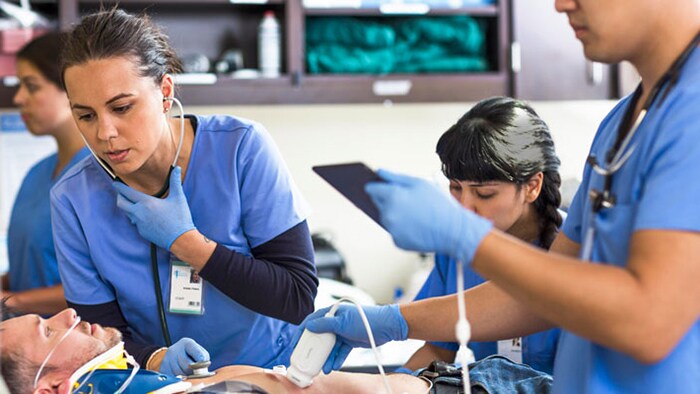
Understanding which ventilation technique is appropriate for each patient can help improve patient care and assist clinical teams for success. There are different ways to support COVID-19 patients with NIV therapy and depending on the route of the best course of treatment, each comes with different considerations. Below are the most common NIV therapies, with recommendations on how the transmission risk can be reduced: Of course, vigilance is required to ensure timely endotracheal intubation and positive pressure ventilation if a patient’s clinical status deteriorates. If a patient develops acute respiratory failure with documented or suspected COVID-19 infection fails trials of noninvasive respiratory, they may require endotracheal intubation and positive pressure mechanical ventilation [3-4, 6]. Some ventilator models can be used for both non-invasive ventilation and invasive ventilation, shifting modes as the clinical need changes with the patient. Our mission to improve lives is more relevant now than ever. We are working vigilantly to support healthcare providers around the world and provide them with clinical guidance relating to the use of our professional healthcare products and solutions and any other information that may be helpful during this crisis, like the information in this article. Our gratitude goes out to everyone who is fighting against COVID-19 and who are trying to do what they can to help patients. Stay safe and healthy. [1] World Health Organization (WHO). Infection prevention and control during health care when novel coronavirus (nCoV) infection is suspected: Interim guidance. https://apps.who.int/iris/rest/bitstreams/1266296/retrieve [2] Interim Clinical Guidance for Management of Patients with Confirmed Coronavirus Disease (COVID-19). Centers for Disease Control. https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-guidance-management-patients.html [3] Josh Farkas. COVID-19. Internet Book of Critical Care (IBCC), https://emcrit.org/ibcc/covid19/#noninvasive_respiratory_support, March 2, 2020. [4] David S. Hui, Benny K. Chow, Thomas Lo, et al. Exhaled air dispersion during high-flow nasal cannula therapy versus CPAP via different masks. Eur Respir J. https://erj.ersjournals.com/content/53/4/1802339.long, 2019; 53: 1802339 [https://doi.org/10.1183/13993003.02339-2018]. [5] (https://www.usa.philips.com/healthcare/product/HCNOCTN113/respironics-niv-filter-circuit/overview) [6] Basem M. Alraddadi, Ismael Qushmaq, et al. Noninvasive ventilation in critically ill patients with the Middle East respiratory syndrome. Influenza Other Respir Viruses. https://onlinelibrary.wiley.com/doi/epdf/10.1111/irv.12635, 2019; 13:382–390.
o Provide masks to be worn over the nasal cannula to reduce the potential for airborne virus transmission.
o Ensure timely endotracheal intubation and positive pressure mechanical ventilation if the patient’s clinical status deteriorates [3-4].
o Use a well-fitted oro-nasal mask (or helmet, if available). Avoid use of nasal masks and/or nasal pillows, if possible.
o Employ a dual-limb ventilator with filters placed at the ventilator outlets.
o Using an appropriate and compatible expiratory port filter for single-limb non-invasive ventilators will reduce the risk of virus spread in the open patient room [5].

Share on social media
Topics
Author

Jan Kimpen
Chief Medical Officer, Royal Philips Before joining Philips in 2016, Jan Kimpen, Professor of Pediatrics, was CEO of the University Medical Center in Utrecht. He leads the global clinical team of Philips, focusing on advocacy, customer partnerships, clinical research and medical consulting, and is responsible for the annual publication of the Philips Future Health Index. He is a strategic advisor for commercial and clinical strategy, market reimbursement, R&D roadmaps and partnerships and M&A, and provides thought leadership on relevant clinical and medical topics. Jan participates in the WEF Global Future Council on Healthcare, the American Heart Association alliance and the Board of Sanara Ventures in Israel. Jan is president of COCIR, the European trade union for imaging, healthcare informatics and radiotherapy.
Follow me on

Huiling Zhang
Head of Medical Office, Connected Care, Royal Philips Huiling Zhang, MD, MPH, MBA, is a Physician executive with over 20 years of experience in healthcare management.
Follow me on