When Apollo 13 was launched on an April morning in 1970, no one foresaw that astronauts James Lovell, John Swigert, and Fred Haise would soon be fighting for survival as one of their oxygen tanks exploded two days into the mission. Swigert’s now-famous phrase “Houston, we’ve had a problem here” would set in motion a feverish rescue operation to bring the astronauts home safely. As the world held its breath, the NASA flight control team in Houston faced its biggest challenge yet. How do you resolve technical malfunctions from 200,000 miles away? Key to the rescue operation was that NASA kept a mirrored system of the Apollo 13 on earth – a physical model of the spacecraft and its components. This allowed engineers on the ground to model and test possible solutions, simulating the conditions on board of Apollo 13. When the amount of carbon dioxide in Apollo 13’s lunar module rose to life-threatening levels, NASA engineers created an improvised air purifier and instructed the astronauts how to build it with materials available in the spacecraft.[1] At the same time, astronauts on earth ran simulations at Houston and Kennedy Space Center to test procedures for getting the ill-fated crew of Apollo 13 back to earth alive – which they eventually succeeded in, four days after the accident.[2] Of course, technology has come a long way since 1970. Analogue models have been replaced by digital models, enabling NASA to monitor and modify systems in real time with ever more precision.[3] But the underlying notion is still the same: a model of a physical object – a ‘twin’, so to say – enables you to monitor its status, diagnose issues and test solutions remotely.
A model of a physical object – a ‘twin’ – enables you to monitor its status, diagnose issues and test solutions remotely.
What if we apply the same concept to healthcare equipment, where healthcare providers and patients depend on the well-functioning of an X-ray machine or MRI scanner?
The digital twin: a virtual representation of a device
The term ‘digital twin’ was first coined in product lifecycle management in 2003, when digital representations of physical products were still in their infancy.[4] With the advance of computing power and the Internet of Things, digital twins are now gaining traction across industries, including healthcare. They were recently named one of the top ten strategic technology trends in 2018 by Gartner.[5] So what exactly is a digital twin? It is a dynamic virtual representation of a device, which is continuously fed with data from embedded sensors and software (see figure below). This gives an accurate real-time status of the physical device.
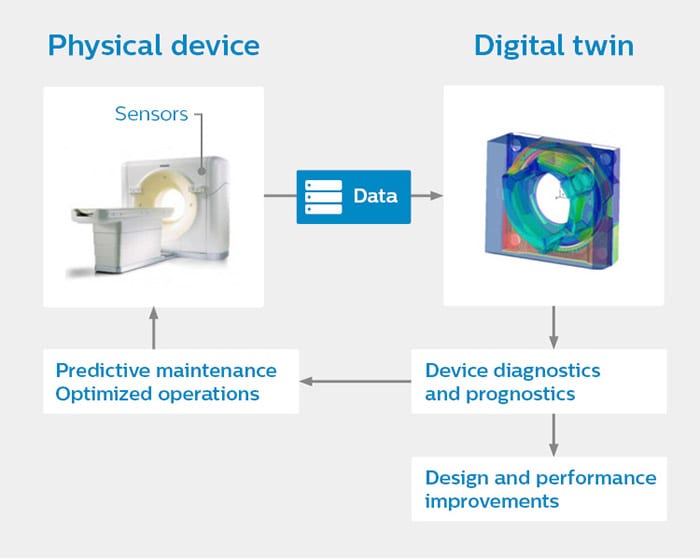
When you add in the power of computational technologies such as artificial intelligence (AI), you can even identify potential problems before they arise, allowing for timely repair or replacement of critical components. For example, smart analysis of data transmitted from sensors in a jet engine during flight can provide 15 to 30 days’ advance notice of potential failures.[3] It is not hard to see how healthcare operations could benefit from the same kind of prognostics.
Identify maintenance needs before they arise
Examination cancellations and unforeseen workflow disruptions are critical issues for both hospitals and patients. Imaging equipment should be ready and operational when they need it. System failures can cause unplanned downtime that is costly and adds to patient waiting times and discomfort, with a potential negative impact on clinical outcomes as well. It is impossible to eliminate the need for maintenance, however. For example, just like you might need to replace the fan belt in your car or the chain on your bicycle after a while, certain components of an MRI scanner degrade over time through regular use. The challenge, then, is to identify potential problems before they occur, so you can schedule maintenance at a time when the equipment is not in use (for example, at night). This is where the concept of the digital twin comes in. Every day, a typical MRI scanner produces an average of 800,000 log messages, which reflect how the system is working technically. Through what we call proactive remote monitoring services at Philips, we can track and analyze these log messages for early warning signs of impending technical issues – following the same philosophy that NASA uses to monitor the status of its space vehicles. (To be clear: these analyses are conducted on technical data only, obtained in agreement with customers; not on the clinical data a hospital collects with the scanner.)
The challenge is to identify potential problems before they occur, so you can schedule maintenance at a time when the equipment is not in use.
Proactive remote monitoring allows us to rectify impending issues from afar, and schedule maintenance by a service engineer when necessary. Because we analyze system data in advance, the engineer knows exactly what kind of maintenance is needed, and which spare component to bring to the hospital. If you are the user of a product, preventative maintenance can feel counterintuitive at first. “Why fix what isn’t broken?” you may think. For those of us who drive a car, we are used to taking it into the garage for a regular check-up. However, nowadays, cars signal electronically when it is time to go to the garage for maintenance. This saves time and money, while it prevents your car from unexpectedly breaking down while you are driving. Similarly, because continuity of care is so vital for healthcare providers and patients, there is significant value in being able to identify potential technical issues in medical systems and devices, and to solve them before they occur.
How proactive remote monitoring works – and why it needs more than AI
So how do we identify potential issues before they manifest themselves? The models we use in our remote monitoring services do not constitute a full digital twin yet. But the underlying principle is the same: through sensors in a physical device, we relay data for remote analysis. When we started developing these services within Philips, we collated technical data from over 15,000 MRI, CT and interventional X-ray systems – analyzing billions of data points. After curating the data, using machine learning (AI) and other analytical methods, we were in fact able to identify patterns that foreshadow specific impending issues. There is more to it than smart number crunching, though. A digital twin of a device consists of four components, as you can see in the figure below.
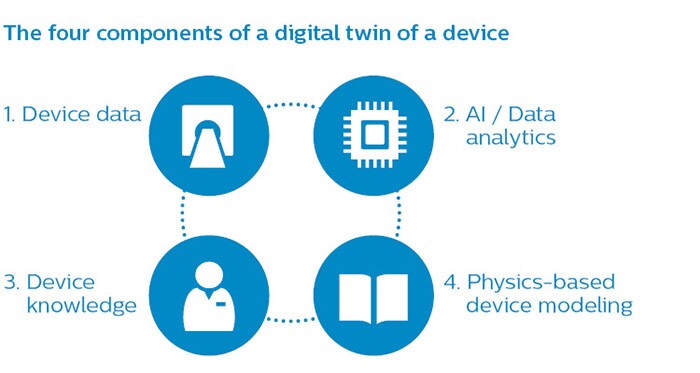
To predict when a device needs maintenance, you need data from that device (component 1) and you need AI and data analytics (component 2) to identify relevant signals in the data. However, to make sense of the data that a device emits, you also need intimate knowledge of that device (component 3). AI can help detect patterns in data, but it cannot tell whether these patterns are practically meaningful. You need human knowledge and understanding of the underlying technology for that. It is hard to find a needle in a haystack, but it is even harder if you don’t know what a needle looks like! AI augments human capabilities, but doesn’t replace them ̶ which is why, at Philips, we prefer to speak of adaptive intelligence. Adaptive intelligence is best conceived of as a helpful, smart assistant, with human knowledge and judgment remaining crucially important. History serves as a reminder here: it was human ingenuity that helped to bring the crew of Apollo 13 home – not technology alone. When developing predictive models it is therefore important to pair data scientists with engineers with deep domain knowledge. They understand how a device was designed and how it operates. This is exactly how we work at Philips.
When developing predictive models it is important to pair data scientists with engineers who understand how a device was designed and how it operates.
There is one more component to the digital twin, and that is physics-based modelling (component 4). Back in 1970, mission control at NASA used physics-based modelling to calculate the optimal angle for re-entry of Apollo 13 into the earth’s atmosphere. Similarly, we can deduce from the laws of physics when a component of a medical device will wear out or overheat – we don’t need AI or machine learning for that. It is a combination of the four components of a digital twin that allows us to generate useful predictions about medical equipment – helping hospitals to achieve uninterrupted workflows.
Accelerating innovation through virtual simulations
Digital twins of devices are not merely useful once a device has been put to use. Because digital twins are already built up during product development, they also enable rapid prototyping of new or improved technology. NASA, for example, uses digital twins in the development of vehicles that endure more extreme conditions.[6] In Formula One, teams create digital twins of their cars, which allows them to rapidly design, test and manufacture improved car parts for the next race.[3] At Philips, we take a similar approach when it comes to designing medical equipment for hospitals or personal health devices. For example, we conducted simulations in the development of a portable oxygen generator for patients with breathing problems. By using digital prototypes, we were able to perform tests that would have taken months and several iterations if we had to build physical prototypes first. Of course the physical product still had to be validated rigorously, but we saved precious development time so we could serve patients quicker with the final product, designing it right the first time.
By running simulations on virtual prototypes of the device, we were able to perform tests that would have taken months and several iterations if we had to build physical prototypes first.
A digital version of you?
If digital twins offer so many opportunities for keeping physical systems and devices “healthy”, could we apply the same concept to human beings? Could a digital version of you – your digital twin – support healthcare providers with diagnosis and treatment? And could it help you manage your own health? It may sound like science fiction, but it is an analogy worth exploring. In fact, it is already materializing and proving useful on a small scale. More on that in my next article!
References
[1] Apollo 13: celebrating the unsung heroes of mission control (2017). https://www.theguardian.com/science/2017/apr/16/apollo-13-mission-control-unsung-heroes-jim-lovell-interview [2] The ill-fated space odyssey of Apollo 13 (2004). https://er.jsc.nasa.gov/seh/pg13.htm [3] Millions of things will soon have digital twins (2017). https://www.economist.com/business/2017/07/13/millions-of-things-will-soon-have-digital-twins [4] Digital twin: manufacturing excellence through virtual factory replication (2014). http://innovate.fit.edu/plm/documents/doc_mgr/912/1411.0-Digital_Twin_White_Paper_Dr_Grieves.pdf [5] Top 10 strategic technology trends for 2018 (2017). https://www.gartner.com/smarterwithgartner/gartner-top-10-strategic-technology-trends-for-2018/ [6] Digital twins in health care: ethical implications of an emerging engineering paradigm (2018). https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5816748/
Share on social media
Topics
Author

Henk van Houten
Former Chief Technology Officer at Royal Philips from 2016 to 2022













