If there’s one industry that is (or at least should be) highly personal, it’s healthcare. When it comes down to it, we each have different preferences: as patients, we might like to analyze our medical data and discuss facts and figures with our doctor, or be more emotionally inclined and prefer a softer touch. The same goes for clinicians: some may choose video over phone consultations, or prefer to specialize in treating a very specific condition. Imagine a healthcare system that can match each patient with their perfect GP, specialist, or even hospital based on acuity, capability, availability, location and even personality type. Sound far-fetched? It might be closer than you think. This concept may be alien to most of the healthcare industry, but it’s very familiar to consumers. Multi-player gaming services can match you with other people based on your age, skills and when you want to play; Amazon’s service AWS IQ matches business customers looking for technology partners; while the likes of Netflix and dating apps learn about your preferences to match you with the best movie or partner based on your past choices and personal profile. They’re all services that get smarter over time, as the artificial intelligence (AI) learns more, improving recommendations for each individual. Back to healthcare, and now that we’re seeing a cultural shift toward more acceptance of virtual care, innovators across the industry are taking some cues from these matchmaking services. Their aim? To personalize and improve the experiences of patients and health professionals, while getting better health outcomes.
We need a system that is better equipped to match patient needs and available resources
Opportunities to reduce waste in the system
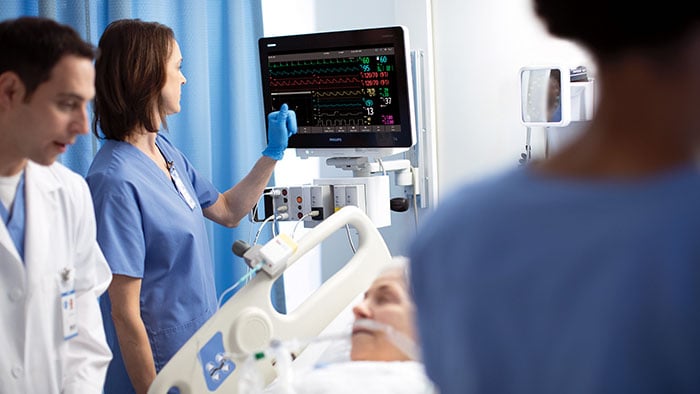
Let’s start with why we need something like this in the first place. In October, I did a full health assessment. The result indicated I had very high blood pressure and possibly an arrhythmia. I downloaded the health report via WhatsApp and then uploaded it into the system of my GP, who ordered a visit to a cardiology clinic, where I did another round of blood tests, another ECG and an ultrasound. The high blood pressure was possibly the result of hereditary kidney issue, and my GP ordered another ultrasound of my kidneys and liver and blood tests at the local hospital. I was told I could see an internist six weeks later in January, in person at the hospital – even though the appointment could quite easily have happened virtually, which would have saved us both time and the healthcare system extra expense. I had to retake some tests and then the internist told me that in order to change my medication, they would notify the pharmacy – by fax. Four months went by and many redundant tests were taken with multiple trips to providers. Extrapolate my experience to millions of patients and you’ve got a huge amount of waste in a healthcare system that can scarcely afford it. That’s especially true these days, when many elective procedures are backed up because of the pandemic. In the US alone, that amounts to millions of patients [1] which is something that I know healthcare leaders are worried will take years to clear.
What if we could create a multi-player healthcare ecosystem that matches patients with the right GP, specialist, payer, or hospital – with AI in the background suggesting the best fit at that moment in time?
The multi-player healthcare matchmaker
We need a system that is better equipped to match patients’ human and clinical needs with available resources in a network, not just physical settings. This has the potential to clear the backlog much faster, but also improve patient and doctor experiences and provide more timely access to quality care that many people still lack. These patient-centric ecosystems could match patients with qualified and available GPs, specialists, hospitals, and behavioral health services – with AI in the background suggesting the best fit for them at that moment in time, given their broader health context. Imagine it: If the clinics, hospital and my GP had been connected into a digital ecosystem like this, it could have potentially triggered a search for an internist anywhere in my country who could take my case as soon as possible, based on one visit to a health hub to conduct a single set of tests, all within one day. That internist would have an overview of my health journey – and see that kidney disease runs in my family – and I could be connected to experts to guide me towards better control of my health. All my data would be stored in one secure, virtual place and shared with any member of my care team, based on my consent. For the hospital network, the ecosystem would enable supply-demand matching and care orchestration. And with the recent rise in community health hubs that offer day surgery and standard diagnostics, this kind of system could help a care team to conduct a procedure faster and guide the patient before and after, which might improve everyone’s experiences, and potentially improve outcomes too.
Bringing it to life through cross-industry collaboration
While I’m painting a picture here of my ideal future vision, teams within Philips have already started working on many of these elements. We’ve recently joined forces with the University of California San Francisco (UCSF) to develop technology that will enable a modern, more streamlined experience for patients, who will be guided through their health journey. This will set a new standard for healthcare delivery. UCSF will use Philips HealthSuite to aggregate and analyze patient data and coordinate the development of technologies that use advanced analytics to enable personalization and make it easier for patients to select providers, access their health information and receive virtual care at home, while also easing the burden on care providers with automated workflows and real-time decision support. One of the aims of the collaboration is to empower UCSF with orchestration tools to bring this vision to life across their network of hospitals, community clinics and outpatient centers, as well as virtual care. Indeed, this ecosystem could play a strong community health role, including educating and supporting patients in their broader health behaviors.
Payers could benefit too
We’ve talked about patients, doctors and hospitals, but a matchmaking ecosystem would benefit the payer too. By taking a longitudinal, proactive view of the patient, it could help payers to take a population health management approach based on the cohorts and care pathways that represent the largest cost in the system: obesity, cardiovascular care, diabetes, pulmonary, cancer and mental health care. This could then enable providers to transition to value-based care, driving better health outcomes at lower cost and putting the right incentives in the system. Meanwhile, in today’s system, we are still heavily reliant on amazing human effort to touch every single part of a person’s care journey. Think of the difference it would make if we could automate referrals, medical documentation and payments – three things which are largely still created by hand, or incompatible systems (and sometimes sent by fax).
Making it more personal
What else could this matchmaking service offer? I see an even deeper personalization capabilities being included in ecosystems like this in the future. Let’s take the example of weight-loss surgery, which can be very successful over the long term, but relies on the patient being engaged in their own care through lifestyle changes. Without this, around a quarter of patients regain significant amounts of weight [2]. The role of the patient’s support network is crucial, but the hospital rarely has any insight into whether the patient is sticking to their treatment in their daily lives. Now imagine that the ecosystem could not only support that patient at home, but also match them with a care team that fits their needs-profile. Are they the type of person who responds better to the bare facts, or do they prefer to understand more about why they need a certain treatment? Do they work better with a specialist who can support their mental health needs, and equally, is there a specialist who can provide that? In my case, you probably know by now that I’m a data person. I like tracking how my health data changes over time, and then discussing the options with my specialists. So, I am ready for a tool that gives me a better visualization and understanding of how I can manage my own health through personalized, evidence-based information and then helps me stick to any plan I have co-created with my GP. This includes both health behaviors – like eating, drinking, exercise, sleep and mindfulness – as well as clinical behaviors, such as adhering to medication and keeping track of vitals, like blood pressure and heart rate.

An ecosystem for an ecosystem
When you think about it, our health is in itself a complex system that’s made up of millions of interconnected elements. Even if we consider the cause to be being overweight, or having cardiovascular disease, or kidney disease, our health is more far more nuanced than that. One person can be overweight and have sleep apnea, and be at risk for developing cardiovascular problems in the future, and also trying to get pregnant. An ecosystem that brings together the different facets of healthcare could enable a more proactive approach to their holistic health. And for providers, knowing earlier on that, for example, their cardiac patients are also at risk for sleep apnea might mean that they can introduce them to sleep therapy and potentially avoid typically higher costs and interventions further downstream.
“I take the view that if something is likely to benefit so many people, then there must be a way to make it happen.”
The industry is more open to it than ever
I spoke recently with the CEO of a major hospital, who reflected on how much has changed this year. “I never worked with video conferencing tools before, now it is the only thing I do,” he said. “We never did virtual care, now I’m exchanging data and protocols with peers. It means that we have to rethink how health systems work and how we work with patients. There’s simply no way we’re going to do it alone.” Working together to create patient-centric ecosystems like this is one major step forward. And another is bringing in fresh ideas and new people. Some of you may have already seen that I will be stepping down as Chief Innovation & Strategy Officer for Philips on July 1st. I will be handing over to Shez Partovi MD, who is someone I find truly inspiring and who I know will lead Philips to the next stage of patient-centered innovation. Meanwhile, I will continue to work with the company on high-impact programs and I look forward to seeing where our journey takes us next towards this vision. As someone with an innovative mindset, while I know there will always be challenges in upgrading a system that’s as complex as healthcare, I also take the view that if it is likely to benefit so many people, then there must be a way to make it happen. So long as we stay single-mindedly focused on our goal of better outcomes, lower costs, and better patient and staff experiences. You often hear people talk about situations that are a “win-win”. This would be a quadruple win. And not a fax machine in sight.
Share on social media
Topics
Author

Jeroen Tas
Chief Innovation & Strategy Officer Jeroen is an experienced global executive and entrepreneur with a track record of leading innovation in the healthcare, information technology and financial services industries. Leading the company’s global Innovation & Strategy organization, he’s responsible for creating a pipeline of innovative business propositions that address emerging customer needs and enable a high-growth, profitable health continuum strategy.
Follow me on