How can we innovate for more equitable cardiovascular care?
Mar 31, 2022 - Reading time 5-7 minutes
Surviving heart disease shouldn’t depend on who you are or where you live, but too often it does. As the leading cause of deaths globally, an estimated 17.9 million people die each year from cardiovascular diseases [1]. Sadly, more than three quarters of these deaths occur in low-and middle-income countries where people often lack access to effective and equitable healthcare services [2]. Without accessible care, early detections that could help avoid premature deaths often happen too late in the course of the disease. How can we design technologies to combat these health disparities and better ensure people everywhere can access the vital care they need [3]?
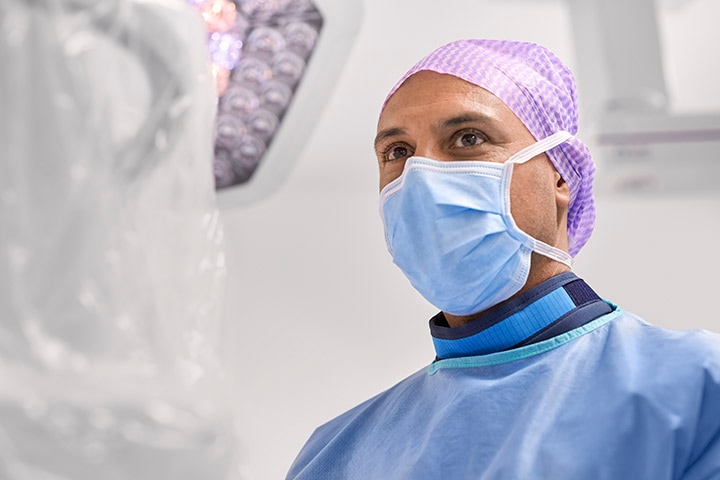
Innovative technologies that make cardiovascular care more accessible
Without a doubt, emerging technologies offer countless possibilities to make healthcare more accessible. Fast-tracked by the pandemic, the shift in delivery from the hospital to the home is making healthcare broadly more available. Specialized care once only available at metropolitan hospitals can now be accessed closer to where people live through a combination of virtual specialist support and technologies – such as ECG, ultrasound and advanced imaging – that enable earlier diagnoses and treatment for conditions like heart disease. Tele-ultrasound technologies, like Collaboration Live, bring critical expertise closer to patients by giving healthcare providers expanded access to secure, real-time guidance and decision support in many areas, including echocardiography.
Primary care facilities and local clinics in many parts of the world can function as diagnostic centers and remote hospitals thanks to virtual care technologies. Especially for people in remote or rural areas, options like Local diagnostic hubs (UK), Virtual Care Stations (US), and technology-equipped container structures (Brazil) offer new ways to access diagnosis and treatment of cardiac conditions. In the future, emerging health innovations could bring cutting-edge mobile healthcare to wherever people are.
Inclusive innovation means putting people at the center of the process
Unfortunately, the digital transformation of healthcare alone will not guarantee equitable health outcomes. New technologies with the power to expand access to diagnosis and disease treatment in certain situations also have the potential to widen gaps in access, affordability, and equitability [4]. This is especially true in places where digital infrastructure is inadequate or where solutions aren’t affordable or culturally relevant. In order to meet healthcare demands in an equitable, sustainable way, those involved in developing new technologies need to fully understand existing needs on the ground and how a solution will be used in practice. Listening to diverse customer and patient voices, balancing stakeholder interests, and working collaboratively with local partners and communities can generate better outcomes and help avoid abandoned equipment and inaccessible or ineffective digital solutions [5].

This people-centric approach calls for ‘radical empathy’ and perseverance, addressing sometimes uncomfortable biases and understanding the range of factors that contribute to health disparities. It then combines these contextual insights with creative thinking to innovate more equitable, responsible, and socially viable solutions.
Seeing the opportunities often requires a change of perspective. While most social determinants of health – like a person’s geographic location or socioeconomic status– are outside the control of a health technology company, there are ways in the design process to recognize and address complex societal challenges. A health technology company may not be able to single-handedly solve a region’s transportation infrastructure challenges, for example, but it can design cardiovascular solutions that better enable access to care for people who can’t easily get to a hospital.
Co-creating affordable, accessible cardiovascular care solutions
Health technology companies can also act as catalysts, drawing together diverse stakeholders to collaborate and bring to life pioneering solutions. Triggered by the very real problem of people in underserved communities dying unnecessarily from cardiovascular disease, a small but dedicated team within Philips set out with a group of volunteers to gather insights and ideate around the shared purpose of bringing critical cardiac care to underserved communities in Africa. Recognizing that people suffering from heart disease often don’t realize it until too late – a reason for such high mortality rates – the team identified early diagnosis as an essential piece of the puzzle. But access to early and affordable diagnoses at primary care clinics is rarely available in underserved communities, which means people wait until they are suffering symptoms and go straight to tertiary health facilities.
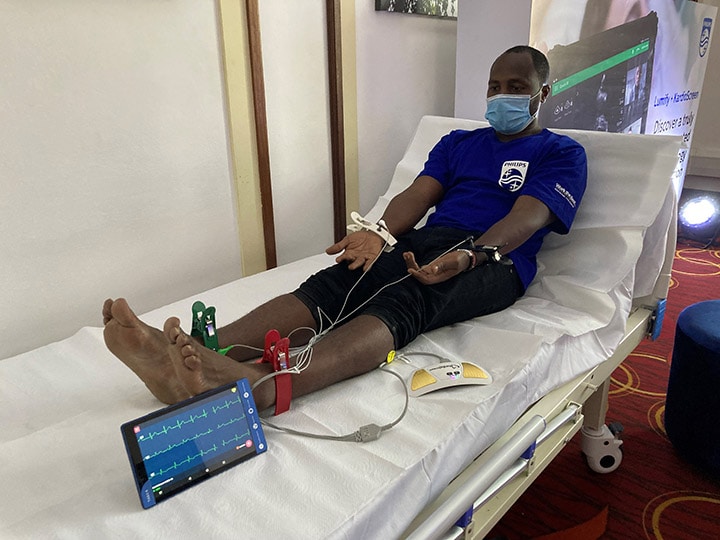
However, pairing a mobile tele-ECG device with Philips Lumify ultrasound offers primary care providers integrated cardiovascular screening and diagnostic capability that can help address the problem. Beyond early detection at the primary care level, this innovative telehealth-based care model can also help provide more effective triage, remotely and at a low cost. Once patients are identified as high-risk, tele-cardiac referral can be used to help get them the right care, including lifesaving cath lab procedures. In addition, by offering use-based payment options, smaller providers, like clinics, can more easily afford to purchase the technology. What began as an internal Philips research project grew into a collaboration that includes Philips Foundation, an external health technology partner, and stakeholders in medically underserved communities. Though still in the early phases, this scalable initiative embodies the kind of equitable care outcome that can come from a people-centered innovation process. In India, another multi-stakeholder collaboration aimed at addressing the growing burden of cardiovascular diseases has resulted in the installation of 1,000 state-of-the-art cath labs at major sites across the country. Not only do these labs help expand India’s capacity to treat a range of cardiovascular diseases with minimally invasive image-guided therapy procedures, but they also lay the groundwork for additional cath lab expansions to help reach the country’s most remote locations.
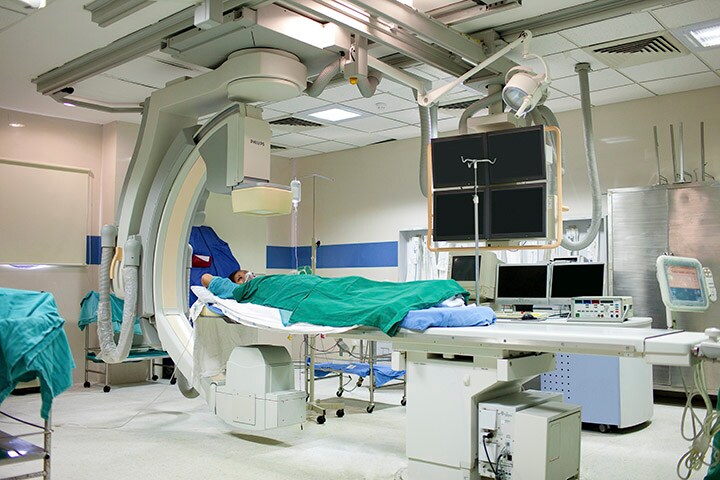
Similarly, office-based labs and ambulatory surgery centers in the United States offer closer-to-home access to potentially life-saving minimally invasive procedures to treat conditions like coronary artery disease. Rising to this challenge, the Philips Experience Design team in partnership with the IFRC (International Federation of Red Cross and Red Crescent Societies), Global First Aid Reference Centre (GFARC) and Philips Foundation, co-created an accessible, image-rich training that can be used to teach life-saving CPR/CPRD skills. Customizable to different regions and available in eight languages, the training kit is now being used in many parts of the world, including underserved regions in Africa.
But technology isn’t always the answer. Sometimes the most applicable solution is a less technically complex one. The CPRD training kit represents a case in point. Cardio Pulmonary Resuscitation and Defibrillation (CPR/CPRD) is an extremely impactful response to sudden cardiac arrest, but in low- and middle-income countries where heart attack is a major cause of death, these life-saving skills aren’t as widespread as they could be.

Designed with easy-to-understand visuals, the CPRD training kit training doesn’t require pre-existing health knowledge or a specific education level. While it may seem surprisingly nontechnical, this people-centric innovation not only embodies what is possible, but also what is preferable [6].
People-centered approach to help ensure health innovations benefit everyone
Designing health technologies that increase access to care and support larger health equity goals – like strengthening global health systems and reaching universal health coverage by 2030 – requires being consciously inclusive throughout the innovation process, designing toward a common goal, and co-creating solutions that are sustainable, equitable and scalable. There’s no one-size-fits-all. Every community has unique factors to consider and designing healthcare solutions is different depending on where you are and what you need. To solve complex problems and deliver more meaningful outcomes means engaging in a truly collaborative, people-first approach. [1] World Health Organization. https://www.who.int/health-topics/cardiovascular-diseases/
[2] World Health Organization. 11 Jun 2021. https://www.who.int/news-room/fact-sheets/detail/cardiovascular-diseases-(cvds)
[3] World Health Organization. 13 Dec 2017. https://www.who.int/news/item/13-12-2017-world-bank-and-who-half-the-world-lacks-access-to-essential-health-services-100-million-still-pushed-into-extreme-poverty-because-of-health-expenses
[4] Eiselé J. “How digital equality could boost heart health.” World Economic Forum. 29 Sep 2021. https://www.weforum.org/agenda/2021/09/how-digital-equality-can-boost-heart-health/
[5] Fonga H, Harrisa E. “Technology, innovation and health equity.” World Health Organization. 2015. https://www.who.int/bulletin/volumes/93/7/15-155952.pdf
[6] Rees M, Torres D P. “Morality, Foresight, and Human Flourishing: An Introduction to Existential Risks.” Pitchstone Publishing. 2017.









