Seven key success factors for digital transformation in healthcare
Apr 13, 2022 - Reading time 7-9 minutes
A surge of innovations is driving digital transformation in healthcare, with 81% of healthcare executives saying that digital transformation in their organization has accelerated in the wake of the COVID-19 pandemic [1]. However, technology is only part of the equation. For digital transformation in healthcare to move from isolated pockets of innovation to an integrated enterprise effort, it needs to address people, processes, and other factors as well as data and technology. Here are seven critical success factors that can make or break digital transformation in healthcare.

1. Designing digital health solutions for better human experiences
At its heart, digital transformation in healthcare is really about people, not technology. With digital health solutions, we can take the friction out of care experiences. That means healthcare professionals get to focus on what they do best, without getting bogged down in complexity and inefficiencies that are contributing to alarming rates of burnout. And it means consumers and patients get to take an active role in their health and wellbeing, with easy to use and intuitive tools that help them stay healthy and prevent disease to take the pressure off healthcare systems.
But as we know from the early days of electronic medical records, digital technology can also become a source of frustration if detracts from the patient-provider relationship. As one doctor lamented in the Scientific American: “we physicians entered the profession to connect with and help patients – not to stare at a screen.” [2] Similarly, patients may be reluctant to adopt digital health technology if it creates more hassle than convenience. Or their interest in using the technology may wane over time if it doesn’t add enough value, as we have seen with some first-generation fitness and health tracking wearables [3].
To ensure that digital transformation in healthcare is embraced by patients and healthcare professionals alike, it needs to be rooted in human-centered design. Co-creation sessions with patients and healthcare professionals can help to uncover their needs and pain points, and tools such as experience flows can help to understand the practical and emotional context in which digital technology is used. Equipped with such insights, we can develop solutions that truly improves people’s lives – whether it is through augmenting the skills of physicians to help them manage ever-increasing workloads, or by empowering patients and care providers to better manage chronic disease at home.

2. Bringing everyone on board through effective change management
As the scope of digital solutions expands – often impacting multiple stakeholders across departments – change management becomes increasingly critical to successful and sustained transformation.
For example, as healthcare providers seek to better orchestrate patient transitions from one care setting to the next, new digital innovations using predictive analytics can help to forecast and manage patient flow. This allows healthcare providers to manage patient transitions more effectively, and rapidly adapt to fluctuating patient demand.
But in tandem with the adoption of such technologies, senior leaders will also need to agree with clinical care teams on enterprise-wide KPIs that reflect patient flow across departments. This may represent a big cultural shift from previous, more siloed ways of working. In addition, implications for frontline staff need to be well thought through. Predictive insights should support physicians and nurses in their daily decisions and integrate into their workflows, without adding to existing information overload.
Only by involving all stakeholders from the start will such large-scale digital transformation in healthcare live up to its full potential.

3. Training staff to help them get the most out of digital technology
As digital transformation in healthcare takes hold, new skills will also be required to get the most out of burgeoning technologies such as AI, IoT, and virtual care. The Philips Future Health Index 2021 report revealed that 32% of healthcare leaders consider lack of training to fully utilize digital health technology a barrier to its adoption in their hospital or healthcare facility.
To keep pace with digital transformation in healthcare, national health systems must prioritize the latest developments in AI, data science, and digital health in their education curricula.
In addition, on-the-job training and guidance can help healthcare professionals raise their skill levels. One way of doing is through real-time video collaboration, which enables remote education and on-demand support. For example, in minimally invasive image-guided therapy, virtual collaboration lets interventional physicians look over their peer’s shoulder via webcams mounted on the ceiling of the interventional room.
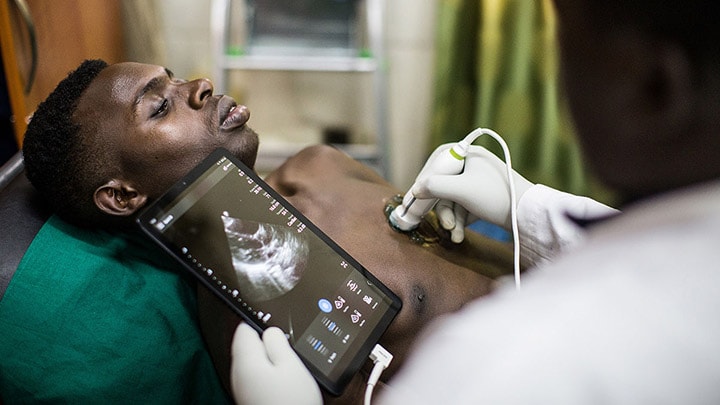
Similarly, hub-and-spoke models supported by virtual collaboration can help to make expert knowledge more widely available throughout a health network – with experienced specialists in a central hub remotely guiding their less experienced peers in satellite locations. Such models are already showing their value in radiology and ultrasound, where specialized staff may be in short supply, particularly in remote regions.

4. Taking an inclusive approach that leaves no patient behind
While the pandemic has demonstrated how digital transformation in healthcare can make a real difference to patients and providers alike, it has also shone a harsh light on long-standing disparities in access to quality care. To prevent a growing digital divide, digital transformation in healthcare should take an inclusive approach that promotes access to care for all – no matter where patients live.
Virtual collaboration between care providers is part of the answer because it can help to make specialist knowledge more widely available. Expanding telehealth options for patients can also lower the barrier to access. But given the fact that people in remote areas and low-income regions often lack access to robust internet, we need to be mindful that an increased reliance on digital technology can actually exacerbate existing health inequities. Differences in digital literacy can further compound this issue.
That means virtual innovations need to be accompanied by new physical access points – for example, in the form of virtual care stations that allow patients to connect with care providers through convenient neighborhood locations. In addition, digital patient engagement initiatives should cater for the needs and preferences of different patient groups. And when trying to reach underserved communities, healthcare leaders should work closely with local partners and stakeholders to understand how they can best serve patients and design solutions accordingly.
5. Adopting cloud-based platforms for data access anytime, anywhere
Data is the lifeblood of digital transformation in healthcare. But today, it is often locked away in different systems and devices that don’t speak to each other. The result is a patchwork of point solutions. In our Future Health Index 2021 report, healthcare leaders cited difficulties with data management (44%) and lack of interoperability and data standards (37%) as the biggest barriers to adoption of digital health technology in their hospital or healthcare facility.
As healthcare becomes increasingly distributed, extending from the hospital into the home and local communities, having an end-to-end data strategy that spans the entire patient journey will become even more important. What’s needed for digital transformation in healthcare are digital platforms that enable the fast and secure exchange of data across settings, offering a comprehensive view of the patient wherever they are being diagnosed, treated, or monitored.
During the COVID-19 pandemic, healthcare providers have experienced firsthand how cloud-based solutions provide flexibility, scalability, and speed – both in adopting new innovations and in adjusting resources to meet fluctuating demand. In 2022, 66% of healthcare executives expect to move their technology infrastructures to the cloud – a number that is set to rise to 96% two years from now [4].
At Philips, we’re enabling this transition with Philips HealthSuite: an open, secure, cloud-based platform that collects, compiles, and analyzes clinical and other data from a wide range of devices and sources. Through a combination of AI and deep clinical knowledge, we can then translate those data into insights at scale that support healthcare professionals at the point of care.

6. Building digital trust by safeguarding data privacy and security
Because health data is among the most sensitive personal information, trust is paramount for digital transformation in healthcare. When asked what would keep consumers from using digital devices for healthcare, 41% ranked “concerns about my privacy or data security” as the number one barrier [5]. Similarly, for healthcare CIOs tasked with keeping patient data safe across a growing plethora of channels and devices, data security is as big a concern as ever [6].
More than ever, cybersecurity requires a systematic approach that considers where and how devices are used. At Philips, we take an end-to-end ‘Security Designed in’ mindset that puts security considerations front and center all the way from product design and development to testing and deployment – backed by robust policies and procedures for monitoring, effective updates, and where necessary, incident response management.
Similarly, we are committed to responsible data stewardship through ‘privacy by design’. This approach aims to embed privacy and data protection controls throughout the entire data lifecycle, from the early design stage to deployment, collection, use and ultimate data disposition and disposal. By being transparent about how we deal with personal data, we can help foster the trust needed for further digital transformation in healthcare.

7. Joining forces through strategic partnerships and ecosystem collaboration
As digital transformation in healthcare picks up speed, healthcare leaders recognize the need to forge long-term strategic partnerships with healthcare informatics companies that can help develop and implement a roadmap to digital maturity. According to our Future Health Index 2021 report, 41% of them believe their hospital or healthcare facility needs to prioritize strategic partnerships to successfully implement digital health technologies.
But no single partner will be able to “do it all”. Healthcare is too complex for that. Instead, the future of digital healthcare will be built in collaborative ecosystems, with solutions from multiple vendors working in concert on open and interoperable platforms.
For example, in radiology, this can take the form of software marketplaces. With the rise of AI, there’s a plethora of apps coming from start-ups and universities. However, hospitals may find it hard to put these apps to use if they lack a common underlying platform that is integrated with their workflow at the point of care. A curated software marketplace allows radiologists to download validated apps from third-party developers via one common platform – without having to worry about point-to-point integrations. It will then be the role of healthcare solution providers like Philips to ensure that such apps run seamlessly on the consoles and mobile devices used by hospital staff.
By combining the strengths of technologies from different vendors, in a way that is easy to access and implement for healthcare providers, we can further accelerate innovation and deliver on the full promise of digital transformation in healthcare.
Download our position paper on digital transformation in healthcare
Discover what the future of digital health will look like – and what is needed to turn this vision into a reality.
Further reading on digital transformation in healthcare
References
[1] https://www.accenture.com/us-en/insights/health/accenture-digital-health-technology-vision-2021
[2] https://blogs.scientificamerican.com/observations/electronic-health-records-and-doctor-burnout/
[3] https://www.gartner.com/en/newsroom/press-releases/2016-12-07-gartner-survey-shows-wearable-devices-need-to-be-more-useful
[4] https://www.accenture.com/us-en/insights/health/accenture-digital-health-technology-vision-2021
[5] https://www.beckershospitalreview.com/healthcareinformation-technology/healthcare-cios-in-2020-3-keypriorities-how-the-role-is-evolving.html
[6] https://www.healthcareitnews.com/news/apac/examining-cybersecurity-our-medical-health-devices

