Imagine a future in which all healthcare professionals that are involved in the care for a patient have easy access to the same holistic view of that patient – whether it’s in a high-tech hospital room where the patient is about to undergo a life-saving operation, or during a video consult with a patient who calls for advice based on the latest health readings from her home therapy device. As we saw in my previous article, it is the Internet of Things (IoT) that will help turn this vision into a reality. Digital platforms, ubiquitous connectivity and AI will work in concert to support health and well-being, with integrated care ecosystems organized around people’s needs. How is this connected future already taking shape today, and where will it lead us tomorrow? In this article, we will explore a wider range of IoT applications in healthcare – many already available today, others farther on the horizon. All have the potential to deliver on the Quadruple Aim of creating better health outcomes at lower cost, while improving patient and staff experience.
1. From location-dependent to location-independent care
With IoT-enabled solutions, many aspects of care are no longer bound to one location. Instead of patients having to go to a designated room in the hospital, a doctor’s office, or another place where certain medical technology is available, we can now take that technology to the patient.
With IoT-enabled solutions, many aspects of care are no longer bound to one location - we can now take technology to the patient.
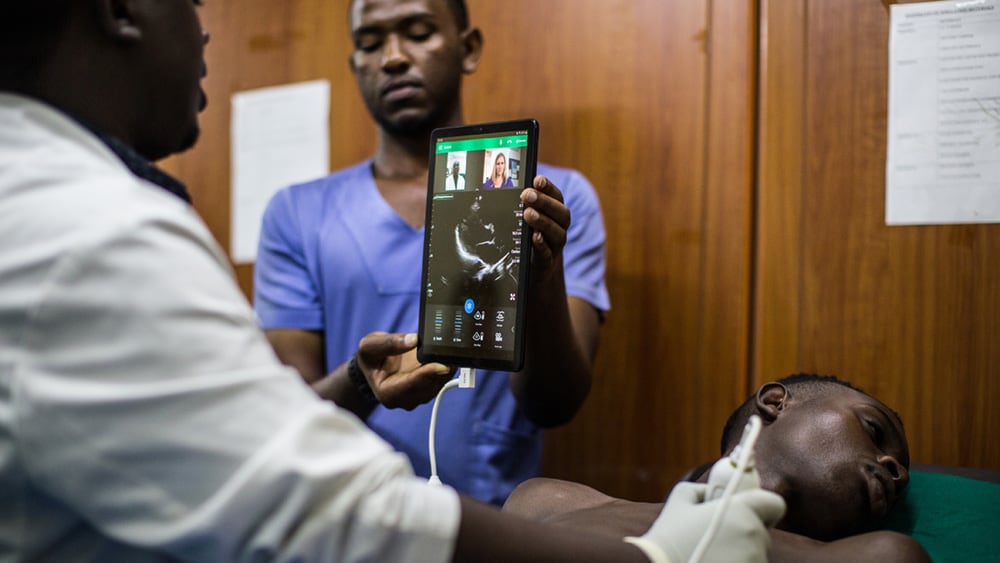
An example of how medical diagnosis is becoming location-independent is Philips Lumify; a handheld, mobile ultrasound system that brings high-quality ultrasound to the point of care. With Lumify, cardiologists at the Haga Teaching Hospital in the Netherlands can now do a quick inspection of the heart in first aid or intensive care, without having to bring in a heavy ultrasound device from the echo room.

But the use of portable ultrasound is not confined to the hospital. Mobile medical teams flying medevac helicopters can take echo images for initial diagnosis and treatment on the spot of an accident. They can even live-stream images directly to the hospital so that hospital staff knows what to expect when the patient is flown in, and can prepare accordingly. Live-streaming also holds promise for remote training to support caregivers in underserved regions of the world. In Rwanda, for example, a mentoring program connects a team of European and US-based ultrasound experts with local caregivers to improve emergency medicine. I expect more initiatives like this in the future, with connected technology increasing access to care where it’s needed the most.
2. From episodic and reactive care to continuous and proactive care
This second IoT-enabled trend follows closely from the first one, but takes it one step further. Coupled with advances in AI and predictive analytics, the IoT allows care not only to become location-independent – but also more continuous, proactive, and preventative; helping caregivers to act pre-emptively when and where it is needed. Patient monitoring is a case in point. Intermittent bedside checks of a patient’s vital signs – such as heart rate and breathing rate – only provide a snapshot in time. Via a wearable biosensor, caregivers can now also monitor the patient’s vital signs between spot checks. Data are fed into a smart algorithm that can inform caregivers on the patient’s condition and send a notification when an intervention is needed, helping them to deliver timely care.
Coupled with advances in AI and predictive analytics, the IoT allows care to become more continuous, proactive, and preventative; helping caregivers to act pre-emptively when and where it is needed.
In today’s ultra-connected world, patients can even be monitored from a remote location – sometimes as far as 10,000 miles away! Thanks to connected technology, clinicians in Perth, Australia, are now able to provide remote nighttime critical care support to patients in the U.S. city of Atlanta during daytime hours in Perth. Supported by algorithms that detect early warning signs, remote experts can communicate with bedside caregivers via a live video link and advise on the best course of treatment. This eICU model helps to reduce the burden of traditional night shift work, and can help to address a shortage of intensivists. In previously published studies, eICU programs have also been shown to reduce ICU mortality by 20% [1], generate care savings of nearly $1,500 per patient across a 60-day post-ICU episode [2], and reduce ICU length of stay by 30% [3]. Fantastic results, which point to the power of continuous and proactive patient monitoring across settings.

3. From hospital- to home-based patient monitoring models
As the IoT enables ongoing health monitoring through wearable technology and personal health records, healthcare professionals now also have much better means to keep track of a patient’s health outside the hospital – both prior to and after a medical intervention. This can help to get patients in optimal condition, shorten hospital length of stay, and prevent avoidable readmissions. Patients can recover safely in the comfort of their home, rather than having to stay in an expensive hospital bed. In line with this philosophy, forward-thinking hospitals such as Rijnstate in the Netherlands are exploring new, virtual models of care. For example, patients who undergo stomach reduction or bowel surgery currently have to stay in the hospital for a few days after their operation. Through pre-surgery health coaching, and with remote monitoring as a safety net after hospital discharge, these patients may be able to return home earlier. Such virtual care models will require close collaboration within a wider network of care, including home caregivers and primary care physicians.
IoT-enabled solutions enable healthcare professionals to keep track of a patient’s health outside the hospital.
In the U.S., reimbursement changes and an increased emphasis on value-based care are an extra impetus for hospitals to rethink the way they bridge the transition from acute to post-acute care for patients with chronic disease such as COPD. Many patients with COPD suffer through repeated hospital readmissions. In 2015, the Centers for Medicare & Medicaid Services began penalizing hospitals for readmissions within 30 days. Through ongoing health monitoring and education after hospital discharge, a pilot program in Alabama managed to reduce acute 30-day COPD readmissions rates by 80% within just three fiscal quarters. Cost reductions: approximately $1.3 million.

4. From one-way to two-way information flows
The rise of home monitoring programs points to another shift brought about by the IoT: whereas in the past it was often the healthcare professional who collected and controlled healthcare information on behalf of the patient, today the patient can take a more active role in collecting and sharing information on their health and well-being – creating a two-way communication flow across care networks.
Today the patient can take a more active role in collecting and sharing information on their health and well-being.
For example, via a smartphone-based platform we announced earlier this year, aging seniors can form and activate a care circle of trusted family, friends, and caregivers, thereby offering visibility into their health status. This simplifies the complexities of coordinating care, as the full care circle has access to the same information – including notifications from a personal alert system worn by the senior person. The alert system, which is already used today and works via a button on a wristband or pendant, allows seniors to easily communicate with a trained care specialist to call for help when needed, 24/7, or after automatic detection of a fall.
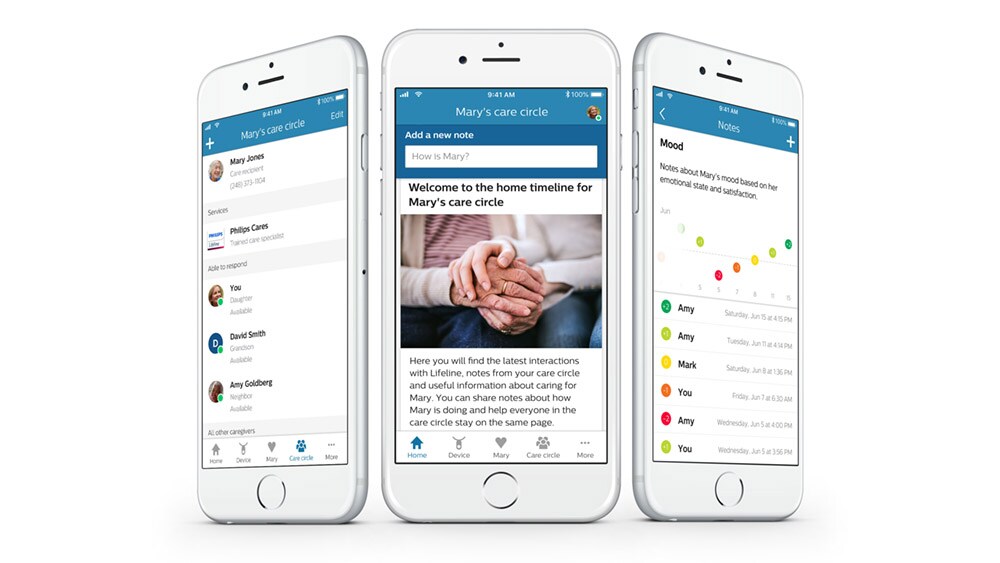
At the same time, we can help professional caregivers deliver predictive care for at-risk seniors in their homes, combining fall detection sensors with other data sources to prevent avoidable hospital readmissions. With further advances in the IoT and advanced data analytics, we will gain more and more insight into emerging health risks – allowing for timely intervention. Of course, appropriate security and privacy controls are essential as more and more health information is shared.
5. From ad-hoc to continuous operational improvement
So far we have focused on how the IoT can support patients and healthcare providers by making care more connected across settings. But the impact of the IoT goes far beyond that. As medical systems and devices become increasingly interconnected and remotely accessible, we can also collect and analyze data from them to optimize their utilization and uptime. Not just when something goes wrong – but ongoing, to ensure that systems and devices are used in the most effective and efficient way to deliver on operational and financial performance goals.
As medical systems and devices become increasingly interconnected and remotely accessible, we can collect and analyze data from them to optimize their utilization and uptime.
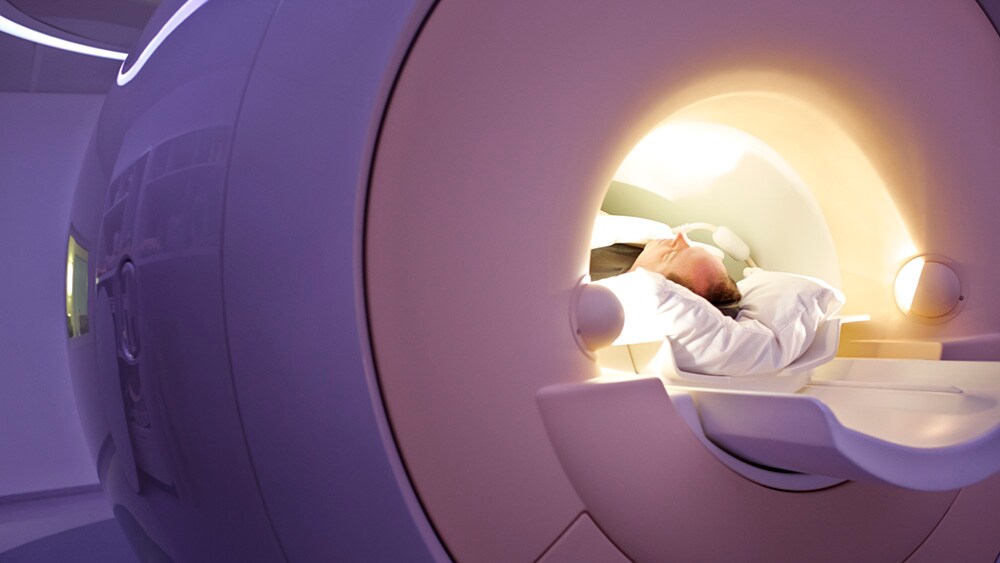
For example, by remotely monitoring and analyzing the technical log files of a CT or MR scanner (with the customer’s consent), we can potentially identify a maintenance need before it occurs. Just as you want to give a patient on the ICU appropriate care before she may suffer a stroke, you want to replace a component of a CT or MR scanner in time to ensure the scanner keeps functioning without hiccups. This can prevent avoidable downtime and delays, which are a nuisance for physicians and patients alike.
Based on the trove of data created by IoT-enabled systems and devices, hospital managers can also start optimizing workflows. What if you could schedule every procedure at the best possible moment to cut back on waiting times? What if you could easily track every piece of medical equipment throughout the hospital in real-time? And what if you could unravel long-term trends in where and when that equipment is needed the most? Answers to these questions would help to get the most out of limited resources – a need that will only become more pressing as the demand for care continues to surge over the next few decades. This is where healthcare can take inspiration from how the IoT is already streamlining operations in other industries, most notably manufacturing.
The future of healthcare is connected
Taken together, these examples show how profoundly healthcare is set to change as a result of ubiquitous connectivity, sensors that are shrinking in size, and AI that helps to make sense of growing data sets. Once disparate fields, these capabilities are now converging in the Internet of Things; connecting people, data, and technology for better care and better health. I am excited for what is next! References [2] Emory Healthcare achieves USD 4.6 million in savings over 15 months leveraging Philips eICU platform
Share on social media
Topics
Author

Henk van Houten
Former Chief Technology Officer at Royal Philips from 2016 to 2022













