New rules of patient engagement: how to meet the evolving demands of the modern healthcare consumer
Aug 19, 2021 - Reading time 8-10 minutes
New technologies and digital platforms are reshaping the way people buy, sell and consume [1]. With the world increasingly at their fingertips, people expect to have choice, convenience and control over every element of their daily lives.

In the wake of the COVID-19 pandemic, we’re seeing the same shift in patients’ expectations for healthcare experiences. For example:
The question is: Will these new preferences for patient engagement endure in a post-COVID-19 world, or are they temporary products of circumstance?
And if these preferences are set to endure, which patient-engagement solutions will satisfy them while also ensuring efficient care delivery across the health continuum?
Six principles for patient engagement with the modern healthcare consumer
We’ve examined these new demands for patient engagement and distilled them into six distinct categories. You can think of them as six qualities that every interaction with the modern healthcare consumer should have in order to enable a positive patient experience, and efficient care delivery:
1. Convenient – welcoming patients through digital front doors
We’ve seen that patients now value convenience more than ever – particularly in the context of everyday care such as picking up prescriptions. But why? One reason may be due to how the public currently perceives healthcare – in a recent report of over 3,409 Americans [6], 66% of adults reported that healthcare contributed to a significant source of stress in their lives. Another reason may just be the convenient experiences we’re used to having in other industries. For example – eCommerce gives us the opportunity to order goods straight to our front doors, at designated time slots. Ride-hailing apps like Uber mean transportation can meet us wherever we are, whenever we need it. Online-banking apps let us manage our finances and plan for the future from the comfort of our own homes. With so many elements of our daily lives now tailored to our preferences and managed at the touch of a button, it makes sense that patients are expecting the same level of convenience from healthcare services. One way healthcare providers are meeting this expectation is through online appointment-scheduling tools. These allow patients to easily select a calendar slot that fits their busy schedules, while helping healthcare providers support staff and location availability.

A great benefit of online appointment-scheduling tools is that they can be followed up with other digital patient engagement initiatives, such as disease-awareness and support programs, or pre- and post-procedural patient surveys. These engagement initiatives can also help to reduce the chances that patients don’t show for appointments – a costly challenge across many departments. In radiology, for example, no-show rates can be as high as 7%, causing preventable delays in diagnosis and treatment, workflow disruptions, and financial losses of up to $1 million. Healthcare providers are also maximizing convenience through the use of patient portals. These allow patients to securely access, manage and share their own imaging records without dedicated training or support, all while reducing the need to return in-person to pick up results. Patient portals also give referring physicians the power to review and compare full imaging records, to promote higher clinical confidence during patient consults.
2. Personalized – tailored to the needs and preferences of every patient
60% percent of consumers don’t think the communications received from healthcare institutions are relevant to them [7]. 84% of consumers want healthcare providers to offer personalized web portals [8]. Clearly, personalization is front of mind for today’s patient population – as it is for today’s healthcare providers. But delivering a truly personalized healthcare experience is challenging – especially when the experience itself is so compartmentalized, including everything from provider communications to treatment itself. One potential enabler of more personalized provider communications is artificial intelligence (AI). By tracking and analyzing user behaviors and collecting feedback over digital platforms (following patients’ consent), algorithms could learn about patients’ preferences for things like interaction cadences and communication styles, then use those insights to deliver better experiences. For example - an algorithm might learn that a particular patient shows up for appointments more often when they get a digital reminder 48 hours in advance as opposed to a phone call 24 hours beforehand, or that they’re more responsive when communications are in a friendly, casual tone of voice as opposed to a formal one. Learning about patient preferences in this way can also free patients from having to spend time explaining their likes and dislikes to healthcare providers, or conducting manual data entry – an added bonus for convenience

Providers are also embracing patient-provider mapping to deliver a more personalized healthcare experience. This is where clinics, hospitals and GPs connect to become a digital ecosystem that can trigger a search for an appropriate specialist or care team, based on the individual patient’s needs. The specialist (or team) will then have an overview of the patient’s health journey, plus the power to connect them with experts who can guide them in taking better control of their health. All the data is stored in one secure, virtual location – from where it can then be shared with any member of the patient’s care team, following the patient’s consent. Even products like toothbrushes are providing opportunities for personalized patient engagement (and, ultimately, care). For example, many are now paired with AI-powered apps, giving providers a chance to offer real-time guidance and personalized recommendations for improving brushing habits – habits that affect not just oral health, but overall health.
3. Accessible – quality care no matter who patients are, or where they live
According to the World Bank and World Health Organization (WHO), half the world lacks access to quality care [9]. Without drastic action, the WHO estimates that 5 billion people will be unable to access healthcare by 2030 [10]. Even in the most developed countries, people face barriers to care, such as high healthcare costs and imbalances in supply and demand. Of course, accessibility is a vast and complex issue that healthcare providers are tackling in many ways. But to give one example of how providers are innovating to maximize access, a promising area is teledentistry – which gives people all over the world a chance to be seen, consulted with and treated before problems get worse – even in remote locations. Advances are also being made in provider-to-provider telehealth. One example of this is in image acquisition, where expert specialists can remotely guide less experienced peers from anywhere, while the peers themselves stay close to the patients. Just like with teledentistry, this can mean patients don’t have to travel for miles in order to receive specialist care. Another innovation that we recently helped to develop at Philips in order to improve access to care is the Virtual Care Station: a pod-based telehealth environment that delivers virtual-care services in convenient neighborhood locations like retail premises and town halls. Once inside, patients sit in a private room and have a virtual chat with their healthcare provider supported by a high-quality camera, lighting, and speakers.

Of course, an important factor in maximizing accessibility in healthcare, which may seem like a step back in time, is to focus on maintaining and improving traditional communication methods. In a world where healthcare providers are racing to deliver services that can be accessed at the tap of a smartphone, it’s key that methods of patient engagement such as telephoning and sending letters don’t get neglected – or worse, abandoned. Even in developed countries, there are infrastructure barriers that often make these the only viable lines of communication, such as a lack of broadband services. Finally, a key aspect of accessibility that will be front of mind for healthcare providers going forward is accounting for differing levels of healthcare literacy when devising new patient-engagement solutions. For example, providers may want to share in-depth resources and support programs via patient portals in order to help more engaged or healthcare-literate patients take greater control over their healthcare – while chatbots and basic reminders for things like appointments and prescriptions may be more appropriate for patients who just want a basic breakdown of their condition, or clear instructions on how to medicate.
4. Participatory – keeping patients informed and engaged every step of the way
There have been many positive developments in recent years when it comes to ensuring patients are actively participating in their healthcare journeys – particularly in the field of research. For example, between 2019 and 2020, over 80% of research papers were reviewed by patients, and 85% of commissioned educational articles were co-produced with patients and patient advocates [11]. In a patient-engagement context specifically, there are a few ways providers are creating opportunities for patients to participate more in their care. One promising area is in pre-surgery health coaching – an initiative designed to help get patients in optimal condition before they have elective surgery, in order to shorten hospital length of stay and prevent avoidable readmissions. Digital twins will be a key innovation here in the years to come – this is a rapidly emerging field that will give patients the chance to see exactly what will happen to them prior to (or following) surgery, by witnessing a virtual representation of the process that’s based on a digital replica of themselves, plus the objects and systems involved in their care. We’re also seeing an increase in the number of healthcare providers embracing patient-reported outcomes. These allow patients to be monitored from home, but with the ability to share outcomes – such as physical symptoms and wellbeing indicators – directly with their hospital via digital channels. It’s an approach that could be transformative in areas like cancer care, where prolonged time spent in clinical settings or away from loved ones can mean additional stress and discomfort.

5. Connected – healthcare anytime, anywhere
Ever since the emergence of COVID-19, we’ve seen healthcare providers turn to telehealth to bridge distances in times of physical separation. But in a post-COVID-19 world, where certain telehealth demands will no longer be driven by necessity, it’s hard to predict which use cases will endure. One strong candidate is home-based monitoring, enabled by wearable bio-sensors. This will help ensure that providers stay up to date on their patients’ conditions, and that they can make fast decisions with confidence about whether certain patients need to be seen or be hospitalized. It’ll also give patients the chance to stay in more comfortable, lower-cost settings, while making it easier for resources (such as beds) to be allocated according to risk.
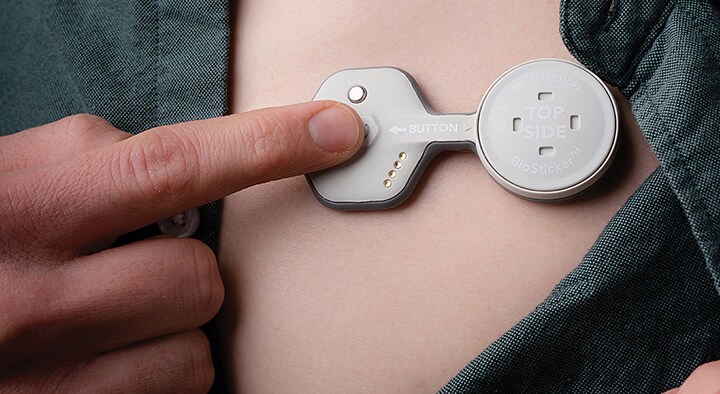
Another strong use case for connected care is remote fetal monitoring – this is where, using a wireless pad and disposable electrode patches placed on a woman’s abdomen, caregivers can monitor vital signs of both mother and baby remotely to reduce unnecessary physical interactions. The expecting moms won’t even need to take the patches on and off – they can wear them in the shower, or even while they’re asleep.
6. Preventative – enabling a brighter future for every patient
Right now, the global wellness market is estimated to be worth more than $1.5 trillion, with annual growth of 5-10% [12]. And in a recent study of 7,500 consumers across six countries, 79% of respondents said they believe wellness is important, with 42% considering it a top priority [13]. All of this indicates that now more than ever, people are invested in a more holistic view of health, prioritizing wellness in order to avoid health complications later in life.

We see oral healthcare as one aspect of health where a preventative approach can make a significant difference to long-term outcomes – not just to a person’s oral health, but also to their general health. In West Virginia, U.S. for example, we recently helped expectant and new mothers adopt good oral care habits by supporting the Helping Appalachian Parents and Infants (HAPI) Project. The results speak for themselves: women in the perinatal care program who reported brushing twice daily with a Philips Sonicare toothbrush had improved birth outcomes compared with those who brushed less than twice a day.
Lasting change for patient engagement
COVID-19 has no doubt catalyzed the dramatic shift in what patients expect from today’s healthcare providers, and how they prefer to engage. But while the endurance of some of the shifts in other industries are still in question, such as contactless hospitality and digital events, these new demands for patient engagement were already emerging long before the COVID-19 pandemic hit. As such, it’s likely that healthcare providers will be keeping all six patient-engagement principles front of mind going forward, as each one looks set to endure in its own right.
1. The Deloitte Consumer Review: Digital Predictions 2018, Deloitte, 2018 2. 2020 State of Telemedicine Report, Doximity, 2020 3. COVID-19: Digital Health Trends and Opportunities for 2021, Orcha, 2021 4. The Growing Value of Digital Health, IQVIA Institute, 2017 5. 2019 Healthcare Consumer Trends Report, NRC Health, 2018 6. Stress in America: A Mental Health Crisis, American Psychological Association, 2020 7. Connected Healthcare Consumer Report, Salesforce, 2020 8. Tracking Universal Health Coverage: 2017 Global Monitoring Report, World Health Organization, 2017 9. Primary Health Care on the Road to Universal Health Coverage, World Health Organization, 2019 11. Healthcare Decision Making Should Be Democratized, BMJ, 2021 12. Feeling Good: The Future of the $1.5 Trillion Wellness Market, McKinsey, 2021








