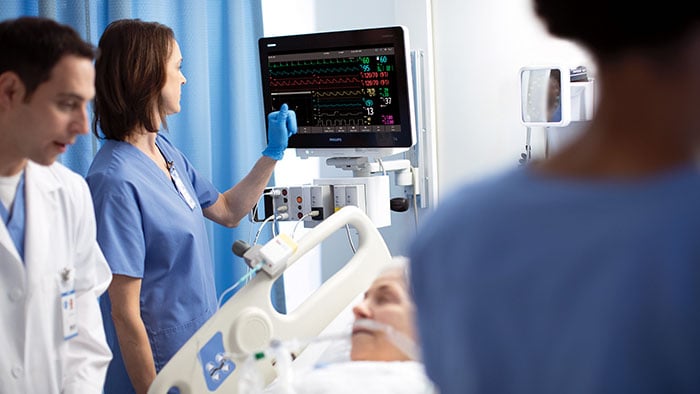
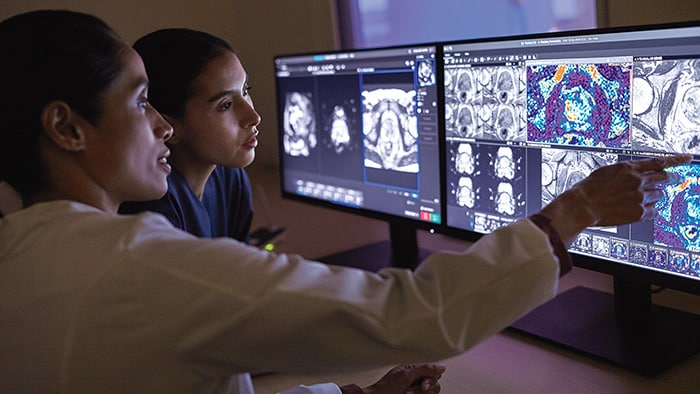
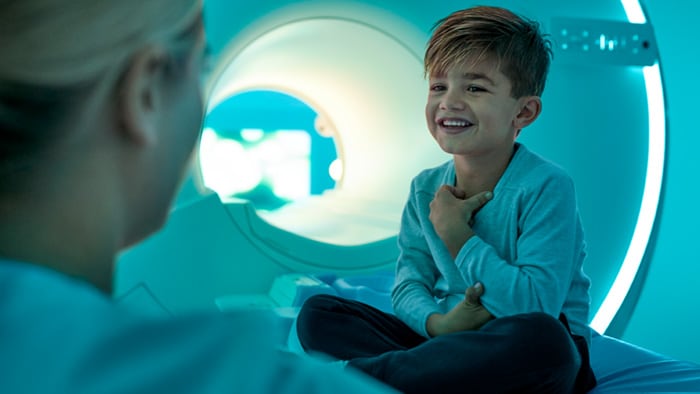
“The hospital room of the future will be the bedroom,” cardiologist Eric Topol wrote in 2015, foretelling a world in which monitoring of vital signs and other relevant physiological metrics would shift from the hospital to the home for all but the most acutely ill patients [1]. Five years later, this prediction seems ever more prescient – in ways that few of us could have imagined just a few months ago. In the face of COVID-19, many healthcare providers turned to remote patient monitoring and virtual visits to continue caring for vulnerable patients while minimizing risk of virus transmission and reducing the strain on scarce hospital resources. It has given a new and urgent impetus to implement digital health solutions at scale, with telehealth projected to grow by 64% in the U.S. this year alone. Sooner or later, the threat from COVID-19 will go away. But the need to rethink where and how we deliver healthcare won’t. What the pandemic is bringing to the fore is how our homes are destined to play a central role in the healthcare system of the future. Rather than having patients travel to see healthcare providers, can we bring healthcare to their doorsteps?
Rather than having patients travel to see healthcare providers, can we bring healthcare to their doorsteps?
It’s a shift that many people would welcome. Consumer interest in remote and virtual health services is seeing an uplift following COVID-19, accentuating the need for increased access and convenience of care. With banking, retail, and other industries already offering 24/7 digital access to their services for many years, healthcare will have to follow suit to meet the expectations of today’s consumer. There is an urgent economic need for change, too. The reality is that today’s hospital-centric model of care is financially unsustainable as demand for healthcare services continues to grow around the world. To keep healthcare affordable, it will need to move into lower-cost settings such as the home whenever possible. But this is not just about moving care delivery out of the hospital. It’s about acknowledging that our health is largely shaped by what takes place before and after doctor or hospital visits. Remote digital health technology can foster a more holistic, longitudinal, and ultimately effective approach to taking care of health and health issues. An approach in which ongoing management of chronic conditions and preventative health strategies are as much a priority as providing care to the critically ill.
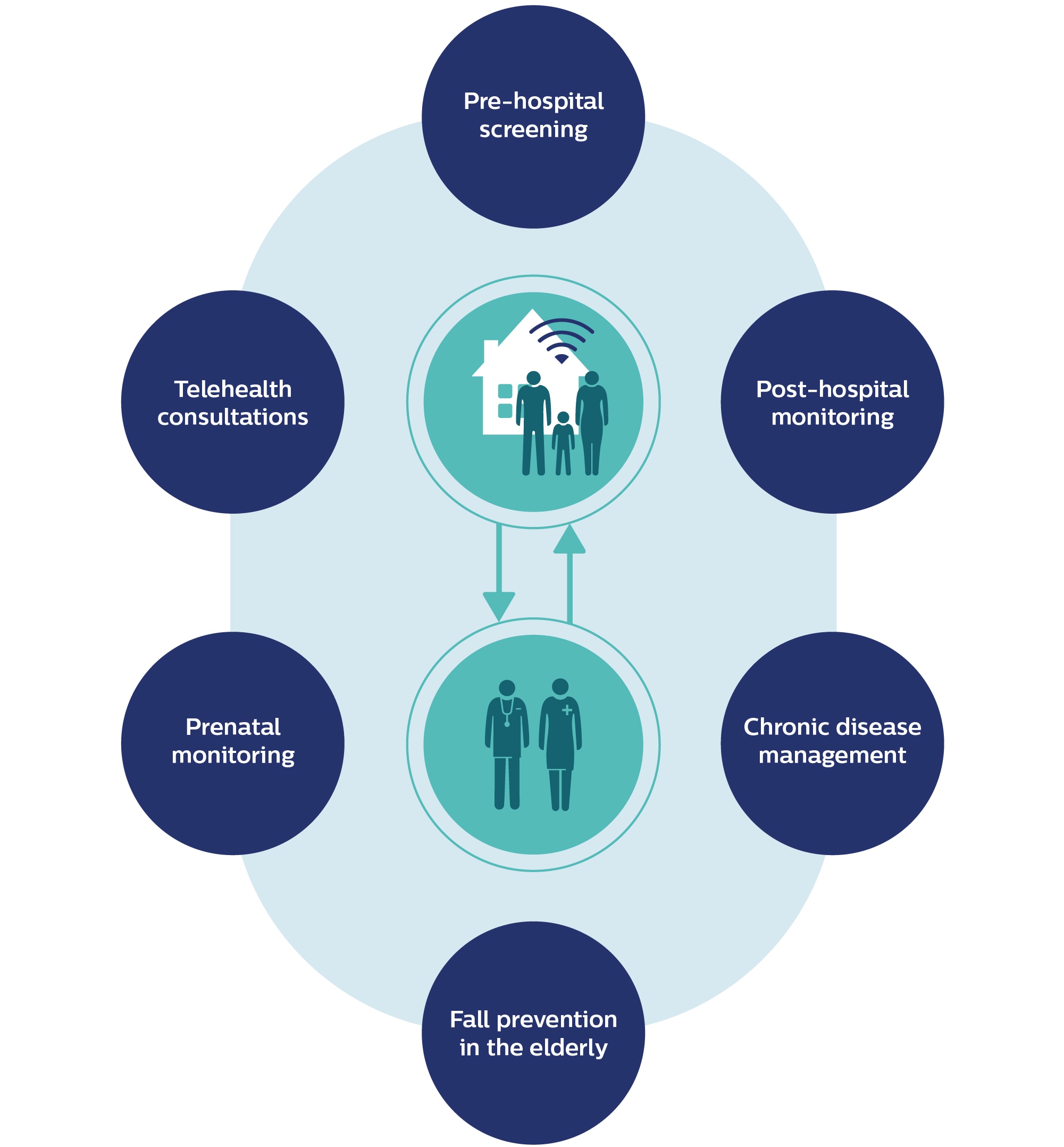
I see six areas in which this vision is already coming into fruition. Let’s explore each of them in more detail.
1. Screening and supporting patients remotely before they enter the hospital
During the COVID-19 crisis, we have seen how remote screening and monitoring of suspected Coronavirus patients can help to safeguard critical care capacity and prevent unnecessary visits to general practitioners and hospitals. Here’s how it works: Patients first complete an online questionnaire at home. Based on the results, the caregiver can assign patients to a risk class and take appropriate actions. If needed, patients can be monitored via automated follow-up surveys. Patients with a high-risk score are contacted by a call center for additional information before referring them to their general practitioner, who can then provide the necessary care or direct them to the hospital. Developed in collaboration with Dutch care providers, this remote screening solution has been used by hospitals and home care organizations to keep patients and staff safe. As a next step, patients could also receive wearable health monitoring devices to remotely track potential deterioration.

In a similar vein, forward-thinking hospitals are exploring other types of remote patient engagement prior to medical intervention – connecting with patients at home as they prepare for a procedure. For example, pre-surgery health coaching could help to get patients in optimal condition before they have elective surgery, in order to shorten hospital length of stay and prevent avoidable readmissions. The underlying vision is as simple as it is powerful: “Better in, better out.”
2. Keeping a caring eye on patients following hospital discharge
Remote health monitoring in the home can be equally valuable after patients have received care in a hospital. Following hospital discharge, patients are typically disconnected from healthcare oversight – contributing to potentially avoidable hospital readmissions that cause patient distress and cost more than $17 billion in the U.S. alone [2]. Increasingly, we will see the use of remote patient monitoring, for example using wearable sensors to keep watch of patients after hospital discharge. These sensors, which are already in use in lower-acuity hospital settings today, can collect and transmit critical data such as heart rate, respiratory rate, skin temperature, and body posture.
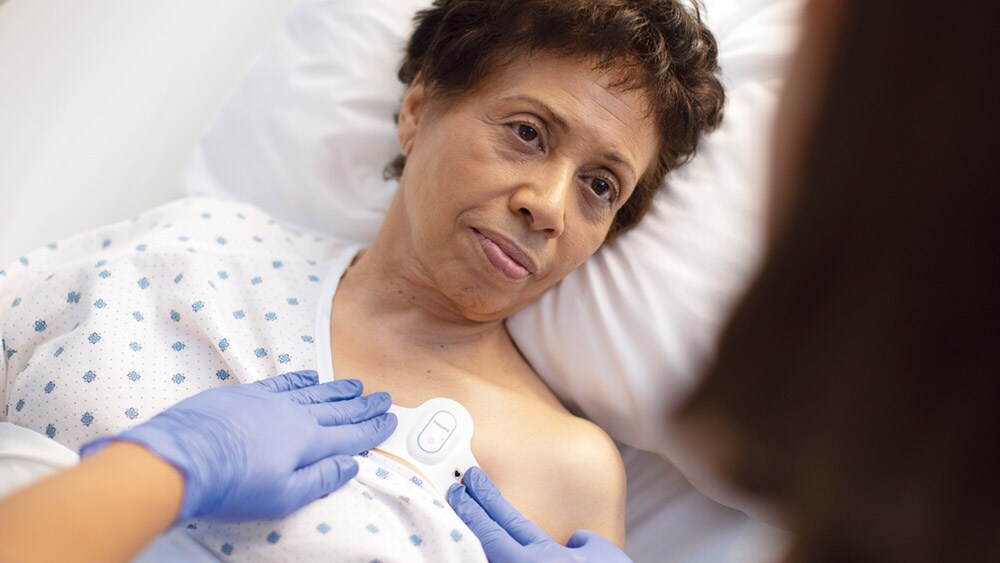
In addition, people will be able to provide regular feedback on their health and quality of life by filling out online questionnaires or talking to a chat bot – without having to leave the house. I have written before about the value of tracking such patient-reported outcomes in home monitoring of prostate cancer. In the wake of COVID-19, it is also proving useful in monitoring Coronavirus patients following hospital discharge. Bringing various health measures and patient-reported outcomes together allows healthcare providers to detect early signs of deterioration and to invite patients to the hospital for follow-up treatment when needed.
3. Empowering patients with chronic disease to manage their illness
Another group set to benefit from at-home medical technology is people with chronic diseases. About one in three people worldwide suffers from multiple chronic conditions, such as diabetes, hypertension, heart failure, or COPD [3]. Not only can these diseases severely impair quality of life for those affected, they put a heavy burden on our health systems too. In the U.S., it has been estimated that chronic diseases account for a staggering 75% of the nation’s total healthcare expenditure [4]. Home-based medical technology can help curtail those costs and improve quality of life – by tracking relevant health data, integrating them with other data sources such as electronic medical records, and translating the combined data into actionable insights. This can encourage patients to take an active role in managing their disease, while enabling care professionals to support them in a more targeted way. For example, at Philips we developed a cloud-based platform that allows homecare providers and physicians to remotely monitor patients with chronic sleep apnea, and to prioritize those in need of intervention or a change in care. Connected home devices and home care management plans can also help address one of the most frequent problems that undermines the effectiveness of chronic care: lack of treatment adherence. According to the WHO, 50% of patients who suffer from chronic disease do not adequately adhere to their treatment recommendations [5]. Smart pill dispensers can be part of the solution by notifying patients to take pre-packaged unit doses of medication. Through an assist app that comes with the pill dispenser, family and caregivers are notified, enabling them to contact the patient when he or she does not take medication – supporting adherence to the therapy plan.

4. Enabling senior people to live independently
Elderly care at home is evolving just as rapidly thanks to remote technology. Falls are a leading cause of fatal and nonfatal injuries for people over 65. In the U.S., every 11 seconds an older adult is treated in the emergency room for a fall, and every 19 minutes, an older adult dies from the consequences of a fall [6]. What if we could identify those at risk of falling before a person actually suffers an injury? Predictive analytics, using data collected via connected health technology, helps care providers do just that. It can combine data from multiple sources – including hospital-based electronic medical records, historical use of medical alert services, and auto-alerts that signaled previous falls – to identify seniors who are at risk of emergency transport in the next 30 days. This allows healthcare providers to reach out to a senior person proactively before a fall occurs, preventing unnecessary treatment in the hospital and driving down costs of transportation, acute care, and rehabilitation.

In the future, such services may be complemented by other types of monitoring that could eventually become embedded into the home itself. Researchers are exploring the possibility of mounting video or motion sensors in different locations of a smart home, specifically designed to support independent living by frail seniors [7]. These ambient sensors could work in conjunction with, or as an even less obtrusive replacement of wearable sensors or devices.
5. Providing remote prenatal care to expecting mothers
Pregnant women with specific health needs or risks are another group who may benefit from remote monitoring by healthcare professionals. For example, Philips is partnering with Babyscripts to enable maternity clinics and hospitals to remotely monitor their pregnant patients’ blood pressure, weight, and other vital signs. This allows pregnant women and care providers to manage pregnancy-associated risks in between regular antenatal care visits by alerting them to changes in a woman’s health condition. Bringing professionally supervised ultrasound monitoring into the home could be a next step. COVID-19 has further highlighted the value of remote prenatal care. It has been estimated that up to half a million women may deliver their babies in 2020 while infected with COVID-19. In fact, of those women who delivered in New York State between March 22 and April 4, 2020, 15% had COVID-19 [8]. Moreover, pregnant women who have not been diagnosed with COVID-19 are interested in ways they can minimize their time in a hospital to limit their exposure to the disease. Responding to those needs, we recently announced the introduction of a wireless and disposable electrode patch that can be placed on the mother’s abdomen. The patch enables continuous, non-invasive monitoring of maternal heart rate, fetal heart rate, and uterine activity, for up to 48 hours. It only needs to be placed once instead of being repositioned every hour, limiting the amount of required physical interactions between nurses and patients – while helping them to stay connected remotely.

6. Improving access and convenience of health services for all
Although smart connected technology can support groups with special medical needs, the ultimate aim should be to support the health and well-being of all. Technology that tracks health and lifestyle data, such as weight, blood pressure, or oral hygiene, can be further embedded into the home environment, for example via a smart mirror in the bathroom or mobile interfaces that display insights to support healthy living. Professional support will be at people’s fingertips, with telehealth services embedded into digital health applications that they can access from the comfort of their home. In oral healthcare, for example, tele-dentistry allows people to consult dentists remotely by sharing images of their teeth via their smartphone – which opens the door to remote screening, diagnosis, consultation, treatment planning, and monitoring of disease progression. This holds particular promise for people who live in rural or isolated locations, where the nearest dentist may be many miles away. COVID-19 has drastically accelerated adoption of tele-dentistry in the U.S., with many dental professionals switching to remote consultations to stay in touch with patients. Significantly, dental care providers can now submit claims and be reimbursed for patient consultations by telephone or livestreaming video. It may very well prove to be a tipping point for tele-dentistry – and it’s not hard to see how the pandemic could provide a boon to other forms of remote health consultation as well.
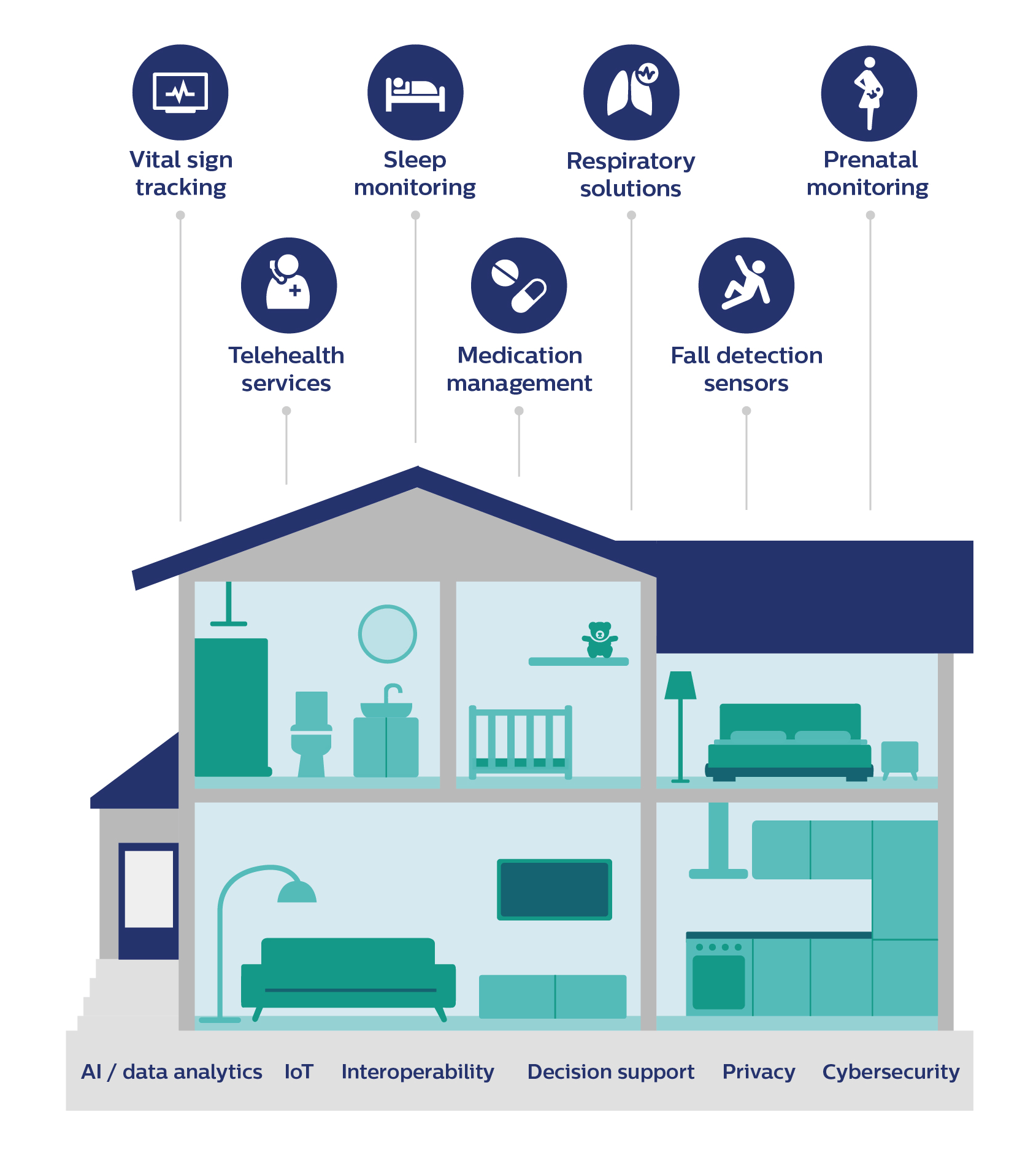
Staying in touch when it matters
Ultimately, the home as a place of care will be one in which IoT-enabled devices and sensors, combined with artificial intelligence and voice or video interfaces, are integrated seamlessly and unobtrusively to support people’s health and well-being. All linked to interoperable digital platforms that connect patients, care providers, and payers. With strict privacy and security controls in place. It will help to connect the dots across people’s health journey, supporting value-based care that is focused on long-term health outcomes rather than on acute episodes of care. At many moments along that journey, in-person care will remain indispensable – whether it is in the form of a visit from a caregiver, or a trip to the hospital or doctor’s office. But it will be reassuring to know that at the end of the day, when we retreat into our private little worlds, professional caregivers may never be far away – guarding or supporting us if and when we need them, even in the comfort of our homes. References [1] Topol, E. The patient will see you now: the future of medicine is in your hands. 2015. [2] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6669363/ [3] https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6214883/ [4] https://www.chronicdisease.org/page/whyweneedph2imphc [5] https://www.who.int/chp/knowledge/publications/adherence_report/en/ [6] https://www.ncoa.org/news/resources-for-reporters/get-the-facts/falls-prevention-facts/
Share on social media
Topics
Author

Henk van Houten
Former Chief Technology Officer at Royal Philips from 2016 to 2022